Do Alcohol and Spicy Food Really Worsen Rosacea? Diet's Impact on Neurogenic Inflammation
The dinner was going well until the second glass of red wine. You felt the familiar warmth creeping up your neck, watched your cheeks turn crimson in the restaurant restroom mirror, and spent the rest of the evening hoping nobody noticed. The next week you ordered a mild curry thinking you were safe, only to experience the same burning flush before you finished the plate. Dietary triggers are among the most personally disruptive aspects of rosacea, yet the advice patients receive rarely goes beyond a generic "avoid alcohol and spicy food" list. The reality is far more nuanced, more individual, and more scientifically fascinating than blanket prohibition suggests.
Table of Contents
- Neurogenic Inflammation: The Bridge Between Food and Flushing
- Alcohol and Rosacea: Beyond Simple Vasodilation
- Capsaicin, Spice, and the TRPV1 (Transient Receptor Potential channels) Connection
- The Histamine Factor: Fermented Foods, Aged Cheeses, and Hidden Sources
- Hot Beverages, Cinnamaldehyde, and Other Underrecognized Triggers
- Building a Personal Dietary Trigger Map
Neurogenic Inflammation: The Bridge Between Food and Flushing
Understanding why diet affects rosacea requires understanding neurogenic inflammation, the process by which sensory nerve activation triggers an inflammatory response independent of the classical immune pathways.
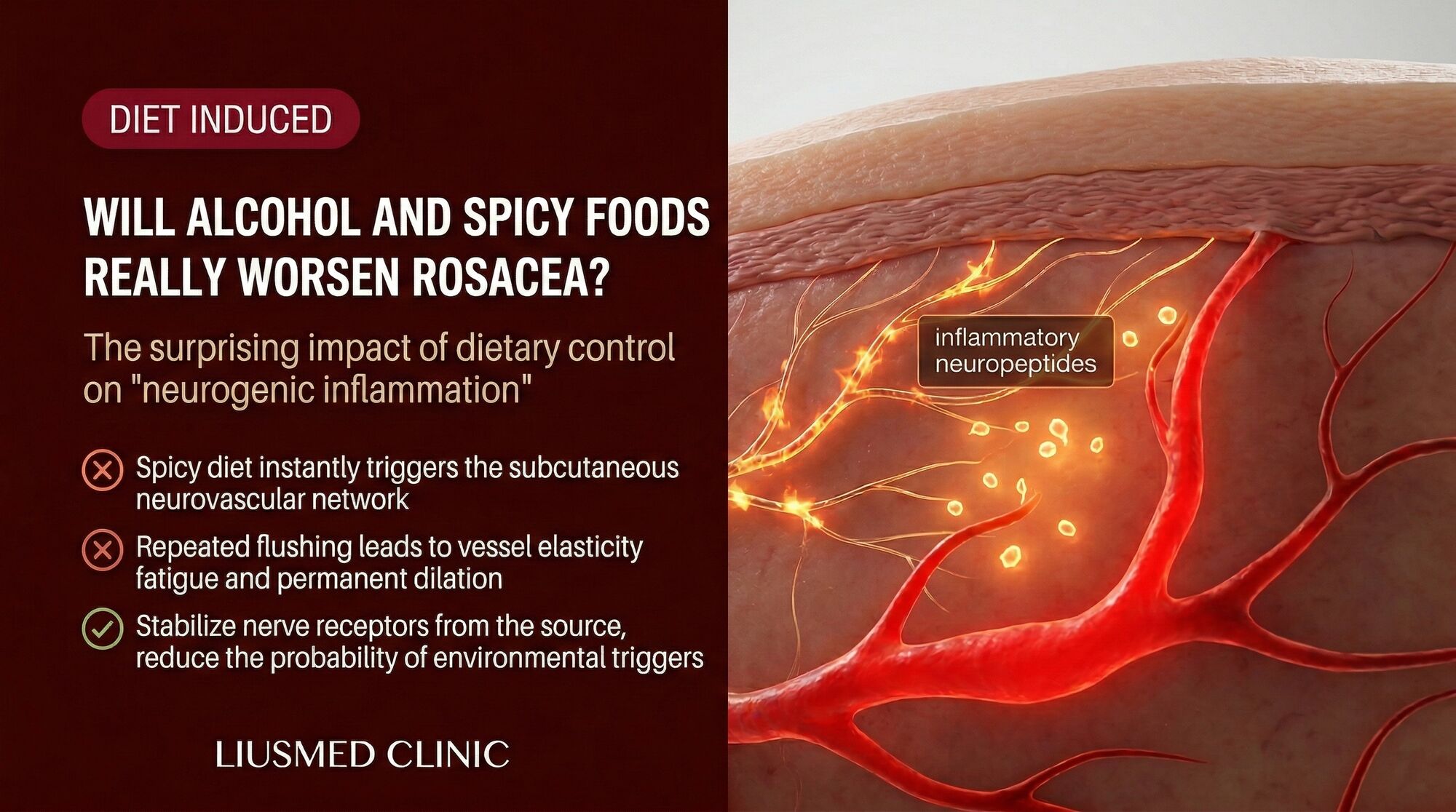
In rosacea, sensory neurons in the facial skin express abnormally high levels of transient receptor potential (TRP) channels, particularly TRPV1 (vanilloid receptor 1) and TRPA1 (ankyrin receptor 1). These channels function as molecular sensors that detect specific chemical and thermal stimuli. When activated, they cause the nerve ending to release neuropeptides, including substance P, calcitonin gene-related peptide (CGRP), and pituitary adenylate cyclase-activating peptide (PACAP), directly into the surrounding tissue.
These neuropeptides produce vasodilation (causing visible redness and the sensation of heat), increased vascular permeability (allowing plasma proteins to leak into tissue, causing edema), mast cell degranulation (releasing histamine and other inflammatory mediators), and recruitment of inflammatory cells. The result is a full inflammatory response triggered not by an immune threat but by nerve activation from dietary compounds.
Crucially, the TRP channel overexpression in rosacea means that the threshold for activation is lowered. A dose of capsaicin that would cause barely perceptible warmth in a non-rosacea individual can produce an intense, prolonged flushing episode in a rosacea patient. This is not a food allergy or intolerance in the traditional sense; it is a neuroinflammatory hypersensitivity mediated by aberrant sensory nerve signaling.
The neurogenic inflammation pathway also explains why dietary triggers do not affect all rosacea patients equally. The degree of TRPV1 upregulation, the density of sensory nerve fibers in the facial skin, and the individual's baseline neurovascular reactivity all determine the threshold at which a specific dietary compound triggers a clinical response.
Alcohol and Rosacea: Beyond Simple Vasodilation
The conventional explanation that alcohol causes flushing because it dilates blood vessels is an oversimplification that fails to account for the specific and prolonged nature of alcohol-induced rosacea flares.
Alcohol affects rosacea through at least four distinct mechanisms operating simultaneously.
Acetaldehyde-Mediated Flushing. Ethanol is metabolized to acetaldehyde by alcohol dehydrogenase. Acetaldehyde is a direct vasodilator and mast cell activator. The rate of acetaldehyde accumulation depends on the individual's enzyme activity: patients with less efficient aldehyde dehydrogenase 2 (ALDH2), common in East Asian populations, experience more intense and prolonged flushing from smaller amounts of alcohol.
Histamine Content and Release. Alcoholic beverages, particularly red wine, contain significant levels of preformed histamine. Additionally, alcohol inhibits diamine oxidase (DAO), the primary enzyme responsible for degrading ingested histamine. This double effect, exogenous histamine load plus impaired histamine clearance, produces a histamine surge that activates H1 and H2 receptors on blood vessels and mast cells.
Direct TRPV1 Activation. Ethanol is a known TRPV1 sensitizer at physiologically relevant concentrations. It lowers the temperature threshold for TRPV1 activation from approximately 43 degrees Celsius to approximately 34 degrees Celsius, meaning that normal body temperature becomes sufficient to activate the receptor. This explains why alcohol-induced flushing can persist for hours after the vasodilatory effect of alcohol itself has subsided.
Immune Modulation. Chronic alcohol consumption alters innate immune function, increasing TLR4 signaling and NF-kB-mediated inflammatory gene expression. For rosacea patients, this amplifies the already-dysfunctional innate immune response.
| Alcoholic Beverage | Histamine Content | Other Trigger Compounds | Overall Rosacea Risk |
|---|---|---|---|
| Red wine | High | Tyramine, sulfites, tannins | Very high |
| White wine | Moderate | Sulfites | Moderate-high |
| Beer | Moderate-high | Tyramine, yeast metabolites | Moderate-high |
| Champagne/sparkling | Moderate | Carbonation enhances absorption | Moderate-high |
| Vodka (unflavored) | Low | Minimal congeners | Lower (but ethanol effects remain) |
| Whiskey/bourbon | Low-moderate | Congeners, wood-derived compounds | Moderate |
| Clear spirits (gin) | Low | Botanical compounds vary | Lower-moderate |
The key insight is that even the lowest-risk alcoholic beverages still deliver ethanol, which produces the TRPV1 sensitization and acetaldehyde effects. There is no truly rosacea-safe alcohol; there are only relatively lower-risk options consumed in minimal quantities.
Capsaicin, Spice, and the TRPV1 Connection
Capsaicin, the compound responsible for the perceived heat of chili peppers, is the prototypical TRPV1 agonist. The TRPV1 channel was, in fact, first identified and characterized through capsaicin research, earning it the original name "capsaicin receptor."
When capsaicin reaches TRPV1 receptors on facial sensory neurons, it triggers the full neurogenic inflammatory cascade described above. In rosacea patients with upregulated TRPV1 expression, the response is amplified in both intensity and duration compared to healthy individuals.
However, not all "spicy" foods are equal in their capsaicin content, and not all rosacea-relevant spice compounds work through TRPV1.
Capsaicinoids (TRPV1 pathway): Found in chili peppers (cayenne, habanero, jalapeno, Thai chili, Sichuan peppers contain a different compound). The Scoville rating of a pepper directly correlates with capsaicin content and therefore TRPV1 activation intensity. Small amounts of mild peppers (bell peppers, paprika) may be tolerated by some patients.
Piperine (TRPV1 and TRPA1 pathways): The active compound in black pepper. It activates both TRPV1 and TRPA1 channels, though with lower potency than capsaicin. Moderate use may be tolerated depending on individual sensitivity.
Allyl isothiocyanate (TRPA1 pathway): Found in horseradish, wasabi, and mustard. Activates TRPA1 rather than TRPV1, producing a different quality of burning sensation localized more to the nasal passages and eyes. Can trigger flushing in patients with TRPA1-mediated rosacea subtypes.
Gingerol (TRPV1 pathway): The pungent compound in fresh ginger. A moderate TRPV1 agonist that is less potent than capsaicin but can accumulate with larger servings. Cooked ginger (gingerol converts to shogaol and zingerone) may be better tolerated.
Cinnamaldehyde (TRPA1 pathway): Found in cinnamon, discussed in detail in the next section.
The practical implication is that patients need not eliminate all flavor from their diet. Herbs and spices that do not activate TRP channels, including basil, oregano, thyme, rosemary (topical rosemary oil is different from culinary use), parsley, cumin, turmeric (which actually has anti-inflammatory properties), and coriander, can be used freely to maintain culinary enjoyment while avoiding neurogenic triggers.
The Histamine Factor: Fermented Foods, Aged Cheeses, and Hidden Sources
Histamine-mediated flushing represents a separate but overlapping pathway from neurogenic inflammation. While neurogenic flushing is driven by nerve-released neuropeptides, histamine-mediated flushing is driven by the direct action of histamine on vascular H1 receptors, producing vasodilation and increased permeability.
Rosacea patients often have impaired histamine tolerance due to several factors: mast cell hyperreactivity produces elevated baseline histamine levels; compromised gut barrier function may increase systemic histamine absorption from food; and reduced DAO enzyme activity, whether genetic or acquired, impairs histamine degradation.
High-histamine foods are those that naturally contain histamine or promote its release:
High histamine content: Aged cheeses (parmesan, cheddar, gouda, blue cheese), fermented vegetables (sauerkraut, kimchi), cured and smoked meats (salami, bacon, smoked salmon), fermented soy products (soy sauce, miso, tempeh), vinegar and vinegar-containing condiments, and certain fish (particularly when not fresh).
Histamine liberators (cause mast cells to release histamine): Citrus fruits, strawberries, tomatoes, shellfish, egg whites, chocolate, and certain food additives (sulfites, benzoates, tartrazine).
DAO inhibitors (impair histamine breakdown): Alcohol (as discussed), black tea, green tea, energy drinks, and certain medications.
The histamine pathway explains why some rosacea patients experience delayed flushing, appearing 30 to 90 minutes after eating, as opposed to the rapid onset typical of TRPV1-mediated neurogenic flushing. Histamine from food must be absorbed through the gut, enter systemic circulation, and reach facial blood vessels, a process that takes longer than direct nerve activation from capsaicin reaching oral mucosa.
For patients who suspect histamine sensitivity, a structured low-histamine dietary trial of two to four weeks, followed by systematic reintroduction of individual food categories, can clarify the degree to which histamine contributes to their specific trigger profile.
Hot Beverages, Cinnamaldehyde, and Other Underrecognized Triggers
Several dietary trigger mechanisms receive less attention than alcohol and spice but may be equally important for individual patients.
Thermal Triggers. Hot beverages (coffee, tea, soup) trigger flushing not through their chemical content but through their thermal effect on TRPV1 receptors. The heat sensor function of TRPV1 activates at temperatures above 43 degrees Celsius, and the oral and pharyngeal mucosa communicate thermal information to trigeminal nerve branches that innervate the facial vasculature. The simple strategy of allowing beverages to cool to a comfortable drinking temperature before consuming them can eliminate this trigger entirely, allowing patients to enjoy coffee and tea without chemical concerns.
Cinnamaldehyde. This TRPA1 agonist found in cinnamon, chocolate, tomatoes, and citrus fruits is a potent trigger for patients with TRPA1-mediated rosacea. It is underrecognized because these foods are not traditionally included on rosacea trigger lists, and patients may not connect cinnamon rolls or chocolate desserts with their flushing episodes.
High-Glycemic Foods. Rapidly absorbed carbohydrates produce insulin spikes that can trigger reactive vasodilation. Some rosacea patients report flushing after consuming large amounts of refined sugar, white bread, or sugary beverages. The mechanism may involve insulin-mediated nitric oxide release or reactive hypoglycemia-triggered sympathetic activation.
Food Temperature Contrasts. Moving from hot food to cold beverages (or vice versa) within a short period can trigger vasomotor instability in the facial vasculature. The rapid alternation between vasodilation and vasoconstriction stimuli overwhelms the already-impaired vascular regulation in rosacea skin.
Building a Personal Dietary Trigger Map
Generic avoidance lists are a starting point but are not a replacement for personalized trigger identification. Every rosacea patient has a unique trigger profile determined by their specific combination of TRPV1 sensitivity, TRPA1 sensitivity, histamine tolerance, vascular reactivity, and environmental context.
Step 1: Establish a Baseline (2 Weeks). Adopt a bland, low-risk diet eliminating all common triggers: no alcohol, no spicy food, no fermented foods, no hot beverages, no chocolate, no citrus, no tomatoes. This establishes a baseline symptom level against which reintroduction can be measured.
Step 2: Systematic Reintroduction (1 Food Category per 3 Days). Reintroduce one trigger category at a time, maintaining a detailed diary of intake, timing, and symptom response. Allow a minimum of 72 hours between introductions to account for delayed reactions. Start with foods you most want to retain in your diet.
Step 3: Dose-Response Assessment. For foods that produce mild reactions, test whether smaller quantities or different preparations are tolerated. Many patients find that a small amount of white wine with food produces no reaction, while a full glass on an empty stomach triggers flushing. This dose-response relationship is clinically relevant and dramatically more useful than simple yes/no categorization.
Step 4: Context Documentation. Record environmental conditions alongside dietary intake. The same food may trigger flushing in a hot restaurant but cause no reaction in an air-conditioned setting, because environmental heat lowers the TRPV1 activation threshold. Stress, fatigue, and menstrual cycle phase can also modify trigger sensitivity.
For patients whose dietary triggers are extensive despite systematic identification and management, the underlying neurovascular hyperreactivity may be severe enough to warrant direct intervention. Rosacea Injection Treatment approaches that reduce baseline neurovascular sensitivity can raise trigger thresholds, allowing patients to reintroduce foods that were previously intolerable. This represents a fundamentally different approach from lifelong dietary restriction, targeting the disease mechanism rather than avoiding its triggers.
Frequently Asked Questions
Q1: Is there any type of alcohol that is completely safe for rosacea?
No alcoholic beverage is completely free of rosacea-triggering potential because ethanol itself sensitizes TRPV1 receptors and generates acetaldehyde. However, unflavored clear spirits (vodka) in small quantities, consumed with food and followed by water, represent the lowest-risk option. Red wine consistently ranks as the highest-risk due to its combined histamine content, sulfite levels, and tannin concentration. Some patients achieve adequate tolerance with strict limits (one small drink, with food, in a cool environment), while others find that any amount triggers a response.
Q2: Can eliminating dietary triggers alone control my rosacea?
Dietary trigger management can significantly reduce flare frequency and severity but is unlikely to control rosacea completely as a standalone strategy. Rosacea is a multifactorial disease with environmental, immunologic, microbial, and genetic components that extend far beyond dietary triggers. Dietary optimization works best as one element within a comprehensive management plan that includes barrier care, topical treatment, and potentially procedural intervention.
Q3: I have heard that gut health affects rosacea. Should I take probiotics?
The gut-skin axis is an active area of research, and associations between small intestinal bacterial overgrowth (SIBO), Helicobacter pylori infection, and rosacea have been documented. Some studies show rosacea improvement following SIBO treatment or H. pylori eradication. Probiotics may support gut barrier integrity, but no specific strain or formulation has been validated for rosacea treatment. If you suspect gut-related contributions to your rosacea, seek evaluation for SIBO and H. pylori rather than self-treating with over-the-counter probiotics.
Q4: Does caffeine worsen rosacea, or is it just the heat of the coffee?
Research on caffeine and rosacea suggests that caffeine itself may actually have a mild protective effect through vasoconstriction and antioxidant properties. A large observational study found an inverse association between coffee consumption and rosacea risk. The trigger is typically the thermal effect of hot beverages rather than the caffeine. Switching to iced or room-temperature coffee eliminates the thermal trigger while retaining any potential caffeine benefit. However, adding dairy, flavored syrups, or chocolate to coffee introduces other potential trigger compounds.
Q5: My flushing seems worse during my menstrual cycle. Is there a hormonal-dietary interaction?
Estrogen influences TRPV1 expression and vascular reactivity, and many female rosacea patients report cyclical variation in trigger sensitivity. During the late luteal phase (premenstrual period), when estrogen drops rapidly, some patients experience lower flushing thresholds, meaning foods that are tolerated mid-cycle may trigger reactions premenstrually. Tracking your cycle alongside your food diary can reveal these patterns and allow preemptive dietary adjustment during high-sensitivity phases.
Q6: Will an anti-inflammatory diet like Mediterranean or anti-histamine diet help my rosacea long-term?
A Mediterranean-style diet rich in omega-3 fatty acids, vegetables, whole grains, and olive oil provides anti-inflammatory benefits that may support rosacea management. Reducing processed foods, refined sugars, and omega-6-heavy vegetable oils decreases systemic inflammatory load. A combined Mediterranean and low-histamine approach is reasonable for motivated patients, though the evidence base is largely extrapolated from general anti-inflammatory research rather than rosacea-specific clinical trials.
About the Author
Dr. Ta-Ju Liu is the founder of Liusmed Clinic, specializing in regenerative medicine and minimal incision surgery. His holistic approach to rosacea management integrates dietary optimization, evidence-based topical therapy, and targeted interventional treatments. Dr. Liu emphasizes personalized trigger identification over generic avoidance lists, recognizing that each patient's rosacea responds to a unique combination of dietary and environmental factors.
Disclaimer
This article is provided for educational and informational purposes only and does not constitute medical advice, diagnosis, or nutritional counseling. Dietary modifications should be discussed with a qualified healthcare provider, particularly for patients with existing nutritional deficiencies, eating disorders, or metabolic conditions. Individual responses to dietary triggers vary substantially, and the information presented represents general patterns rather than universal rules. No doctor-patient relationship is established through reading this content.
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

