What Is Basement Membrane (DEJ) Damage? Why It's the Root Cause of Melasma Recurrence and Pigment Drop
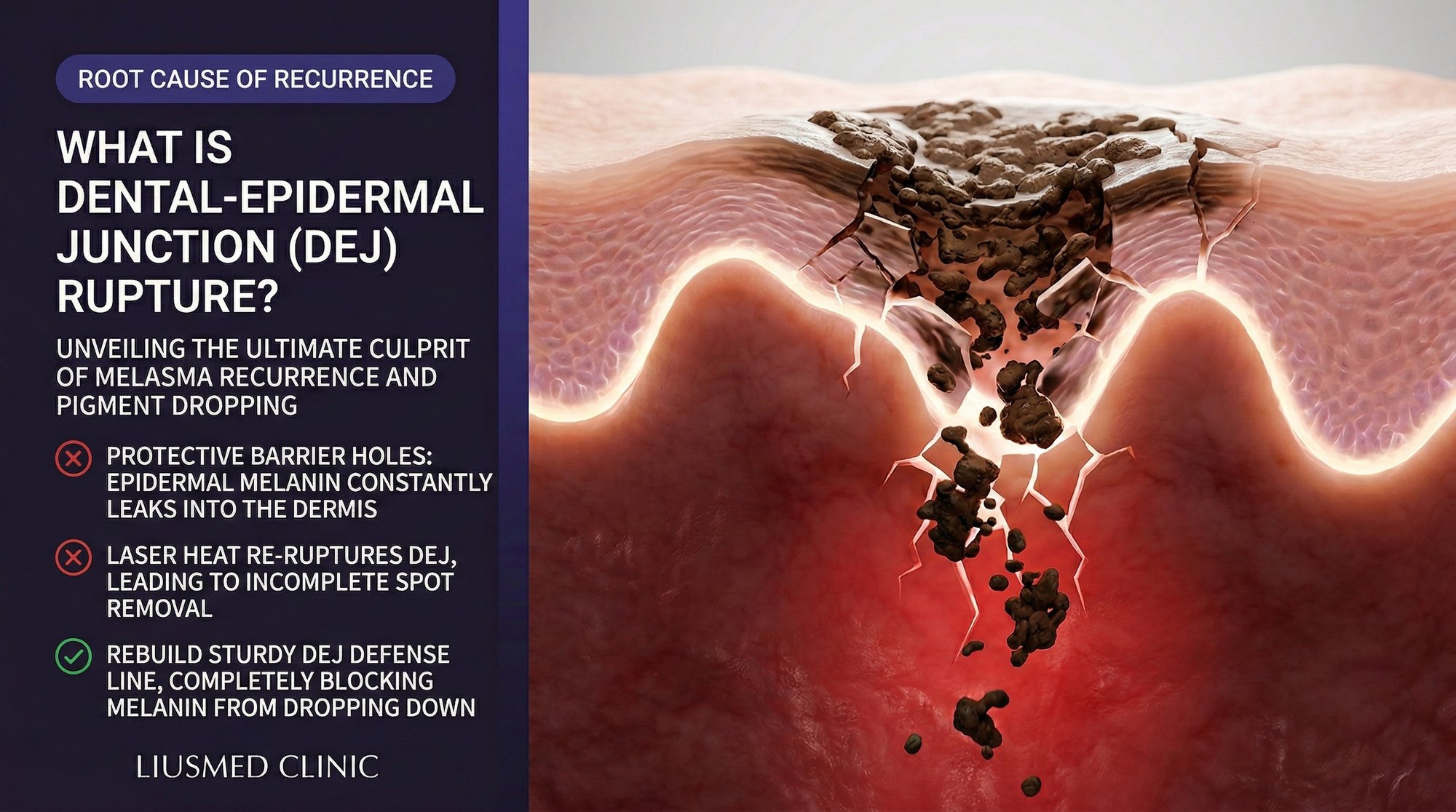
You have probably heard your dermatologist mention "dermal melasma" or "mixed-type melasma" as reasons why your pigmentation is difficult to treat. But what actually makes pigment move from the epidermis—where it belongs—into the dermis, where it becomes stubbornly resistant to conventional therapies? The answer lies in a structure so thin it is invisible to the naked eye: the dermal-epidermal junction (DEJ), also called the basement membrane zone. When this microscopic barrier breaks down, melanin granules fall through the gaps like sand through a cracked floor, lodging in the dermis where they are extraordinarily difficult to remove.
This article explains what the DEJ is, how it gets damaged, why that damage drives melasma recurrence, and how repair-focused treatments aim to restore it.
Table of Contents
- Anatomy of the Dermal-Epidermal Junction
- How the DEJ Gets Damaged in Melasma
- Pigment Incontinence: When Melanin Falls Through
- Why Dermal Pigment Resists Conventional Treatment
- Rebuilding the DEJ: A Repair-Centered Approach
- Comparing DEJ-Aware vs. DEJ-Ignorant Treatment Strategies
Anatomy of the Dermal-Epidermal Junction
The dermal-epidermal junction is not a single membrane but a multi-layered zone approximately 100 nanometers thick that anchors the epidermis to the dermis. Its architecture includes four distinct layers:
- The basal cell plasma membrane of the lowermost keratinocytes, studded with hemidesmosomes that grip downward.
- The lamina lucida, an electron-lucent zone containing laminin-332 and other adhesion molecules.
- The lamina densa, a dense sheet composed primarily of type IV collagen, the structural backbone of the basement membrane.
- The sub-lamina densa zone, where anchoring fibrils (type VII collagen) extend into the papillary dermis, securing the entire structure to the underlying connective tissue.
Key molecular components include:
| Component | Function |
|---|---|
| Collagen IV | Forms the dense meshwork of the lamina densa; provides structural integrity |
| Laminin-332 | Bridges basal keratinocytes to the lamina densa via integrin receptors |
| Nidogen (Entactin) | Cross-links collagen IV and laminin networks |
| Perlecan | Heparan sulfate proteoglycan that regulates growth factor signaling across the DEJ |
| Type VII Collagen | Forms anchoring fibrils that tether the lamina densa to the papillary dermis |
| Integrin α6β4 | Transmembrane receptor on basal keratinocytes that connects to hemidesmosomes |
Beyond its structural role, the DEJ functions as a selective filter. It controls the passage of molecules, cells, and signals between the epidermal and dermal compartments. Under normal conditions, melanin granules produced by melanocytes in the basal layer are transferred upward to keratinocytes and eventually shed with normal epidermal turnover. The intact DEJ prevents melanin from migrating downward into the dermis.
When this barrier is compromised, the consequences for pigmentation control are severe.
How the DEJ Gets Damaged in Melasma
Multiple converging processes damage the DEJ in melasma-prone skin:
Ultraviolet Radiation Chronic UV exposure induces matrix metalloproteinase (MMP) expression in both keratinocytes and fibroblasts. MMP-2 and MMP-9 are particularly destructive to the DEJ because they directly cleave type IV collagen and laminin. Over years of cumulative sun exposure, the basement membrane becomes progressively thinner, more fragmented, and more permeable.
Inflammatory Mediators The chronic dermal inflammation characteristic of melasma amplifies MMP production. Mast cell tryptase, inflammatory cytokines (IL-1, TNF-alpha), and reactive oxygen species all contribute to enzymatic degradation of DEJ components. Senescent fibroblasts in the upper dermis—a hallmark of melasma skin—secrete elevated levels of MMPs as part of their senescence-associated secretory phenotype (SASP).
Hormonal Influences Estrogen and progesterone receptors are present on both melanocytes and keratinocytes. Hormonal fluctuations during pregnancy, oral contraceptive use, or perimenopause can alter the expression of DEJ adhesion molecules and increase melanocyte sensitivity to inflammatory signals. This partly explains why melasma predominantly affects women of reproductive age.
Iatrogenic Damage Aggressive treatments aimed at pigment removal can themselves damage the DEJ. Repeated laser sessions deliver thermal energy to the dermal-epidermal junction zone. Medium-depth chemical peels intentionally wound through the DEJ to stimulate remodeling. While healthy skin can repair these controlled injuries, in melasma-prone skin where DEJ regeneration is already impaired, each treatment cycle may leave the basement membrane weaker than before.
Age-Related Decline Even without external insults, DEJ component synthesis declines with age. Studies show that collagen IV density at the DEJ decreases by approximately one percent per year after age 30. In patients who also have chronic UV exposure and hormonal influences, this age-related decline accelerates baseline DEJ vulnerability.
Pigment Incontinence: When Melanin Falls Through
The term "pigment incontinence" describes the pathological process in which melanin granules escape from the epidermis through a damaged DEJ and become trapped in the upper dermis. Once in the dermis, melanin is engulfed by dermal macrophages, which become melanophages—cells loaded with pigment that can persist for months to years.
This process transforms what might have been manageable epidermal pigmentation into a much more resistant dermal pigmentation problem. The distinction matters enormously for treatment:
Epidermal melanin is continuously shed through normal keratinocyte turnover (approximately every 28-40 days). If you stop the melanocyte from overproducing, the existing epidermal pigment gradually clears on its own through this natural exfoliation cycle.
Dermal melanin has no such clearance mechanism. Melanophages in the dermis have extremely slow turnover. Without active intervention, dermal pigment can persist indefinitely. This is why patients report that their melasma "never fully goes away"—even during winter months with minimal UV exposure, the dermal component remains visible.
The clinical implication is critical: any melasma treatment that does not account for DEJ integrity is addressing only part of the problem. You can suppress melanocyte activity, accelerate epidermal turnover, and fragment epidermal melanin granules—but if the DEJ remains compromised, new melanin will continue to leak into the dermis with every episode of melanocyte activation (triggered by UV, heat, hormonal fluctuations, or inflammation).
Why Dermal Pigment Resists Conventional Treatment
Conventional melasma therapies face specific challenges when dealing with dermal pigment:
Topical Agents Cannot Reach It Hydroquinone, retinoids, azelaic acid, and vitamin C derivatives primarily act within the epidermis. The DEJ—even when damaged—still limits the diffusion of most topical molecules into the dermis. The therapeutic concentrations needed to affect melanophages deep in the papillary dermis are virtually unachievable through topical application alone.
Lasers Risk Collateral Damage To target dermal melanin, lasers must deliver energy deeper into the skin. This increases the thermal load on the dermis, potentially worsening the inflammation and MMP activity that damaged the DEJ in the first place. The paradox of using deeper-penetrating laser energy to clear dermal pigment while simultaneously risking further DEJ degradation is a central challenge in melasma laser therapy.
Chemical Peels Are Too Superficial or Too Aggressive Superficial peels do not reach dermal pigment. Medium and deep peels wound through the DEJ intentionally, which—while it can temporarily dislodge some dermal melanin—also triggers a wound-healing cascade that may produce post-inflammatory hyperpigmentation in melasma-prone skin.
Melanophage Turnover Is Extremely Slow Even if you successfully fragment dermal melanin with laser energy, the clearance of that fragmented pigment depends on macrophage activity and lymphatic drainage—processes that are sluggish in chronically inflamed tissue with impaired microcirculation.
The Melasma Injection Treatment at Liusmed Clinic addresses this challenge by targeting the dermal environment directly—reducing inflammation, modulating the signals that drive melanocyte overactivity, and supporting the molecular components needed for DEJ repair.
Rebuilding the DEJ: A Repair-Centered Approach
Restoring DEJ integrity requires a multi-pronged strategy that addresses both the acute damage and the chronic conditions that prevent natural repair:
1. Suppress MMP Overexpression Reducing the enzymatic destruction of DEJ components is a prerequisite for repair. Anti-inflammatory agents delivered intradermally can downregulate MMP-2 and MMP-9 expression by modulating the NF-kB pathway in both fibroblasts and keratinocytes. Tranexamic acid has demonstrated MMP-inhibitory effects in dermal tissue, contributing to its efficacy in melasma beyond its better-known anti-fibrinolytic properties.
2. Provide DEJ Building Blocks The synthesis of collagen IV, laminin, and nidogen requires specific growth factor signaling and adequate nutritional substrates. Targeted delivery of peptides and growth factors that stimulate basement membrane protein production can accelerate DEJ reconstitution. This is more effective when delivered intradermally, where the therapeutic agents can directly reach the fibroblasts and basal keratinocytes responsible for DEJ synthesis.
3. Reduce Dermal Inflammation Chronic inflammation is the primary driver of ongoing MMP production and DEJ degradation. Anti-inflammatory injection protocols that stabilize mast cells, reduce SASP output from senescent fibroblasts, and normalize vascular tone create a permissive environment for basement membrane repair.
4. Protect the Repairing DEJ from Further Damage Rigorous photoprotection (broad-spectrum UV plus visible light coverage) is essential during the repair phase. Any UV or visible light exposure can re-activate MMP expression and undo repair progress. Heat avoidance (saunas, hot yoga, prolonged cooking over stoves) is also recommended, as thermal stress activates similar inflammatory pathways.
5. Allow Adequate Time DEJ repair is a slow biological process. Collagen IV synthesis, cross-linking, and integration into a functional basement membrane takes weeks to months. Patients accustomed to the rapid (but temporary) results of laser treatments must understand that repair-based improvements are gradual but fundamentally more durable.
Comparing DEJ-Aware vs. DEJ-Ignorant Treatment Strategies
| Dimension | DEJ-Ignorant Strategy | DEJ-Aware Repair Strategy |
|---|---|---|
| Treatment Focus | Melanin granules (epidermal and dermal) | Dermal environment + basement membrane integrity |
| DEJ Impact | May further damage through thermal or chemical injury | Actively promotes DEJ component synthesis |
| MMP Activity | Often increases MMP expression through wound-healing cascade | Reduces MMP overexpression through anti-inflammatory delivery |
| Pigment Drop Prevention | Not addressed | Core objective—sealing the epidermal-dermal barrier |
| Dermal Melanin Clearance | Relies on laser fragmentation + slow macrophage clearance | Reduces new dermal melanin deposition; supports gradual clearance via improved microcirculation |
| Recurrence Rate | High—DEJ remains compromised, allowing continued pigment leakage | Lower—repaired DEJ prevents new pigment from entering dermis |
| Timeline to Visible Results | Fast initial improvement, rapid rebound | Gradual improvement, more stable long-term outcome |
| Ideal Patient Profile | Purely epidermal pigmentation without DEJ compromise | Mixed or dermal melasma with documented basement membrane fragmentation |
Frequently Asked Questions
Q1: How can I tell if my DEJ is damaged?
DEJ integrity cannot be assessed visually from the skin surface. Clinical clues include: melasma that has persisted for many years, a bluish-gray hue to the pigmentation (suggesting dermal melanin), resistance to topical treatments and laser, and rapid rebound after initial clearing. Dermoscopy can sometimes differentiate epidermal from dermal pigment patterns. Definitive assessment requires skin biopsy with PAS staining to visualize the basement membrane—though this is rarely performed in routine clinical practice.
Q2: Can the basement membrane repair itself without treatment?
In theory, the DEJ has regenerative capacity—basal keratinocytes and dermal fibroblasts can synthesize collagen IV, laminin, and other components. In practice, however, the chronic inflammatory environment in melasma skin continuously degrades these components faster than they can be rebuilt. Effective repair requires first addressing the inflammatory drivers (MMP overexpression, mast cell activity, senescent fibroblast SASP) to create conditions under which natural DEJ regeneration can proceed.
Q3: Will oral collagen supplements help rebuild my DEJ?
Oral collagen peptides have shown modest benefits for overall skin hydration and dermal collagen density in some studies. However, there is no evidence that orally ingested collagen peptides specifically target DEJ reconstruction. The basement membrane requires type IV collagen (distinct from the type I and III collagen typically found in supplements) and precise assembly with laminin, nidogen, and perlecan—a process regulated by local growth factor signaling, not systemic supplementation.
Q4: How does the Melasma Injection Treatment support DEJ repair?
The injection protocol delivers anti-inflammatory and reparative agents directly into the upper dermis—the precise location where DEJ degradation occurs. By reducing local MMP activity, stabilizing mast cells, and providing signaling molecules that promote basement membrane protein synthesis, the treatment creates a favorable microenvironment for DEJ reconstitution. Manual hand injection allows depth-specific placement that automated devices cannot match.
Q5: If I repair my DEJ, will the dermal melanin that already dropped through eventually clear?
Existing dermal melanin within melanophages clears very slowly. However, once the DEJ is restored and new pigment is no longer dropping into the dermis, the existing dermal melanin gradually diminishes as melanophages undergo normal (albeit slow) turnover and are removed via lymphatic drainage. The process takes months, but the trajectory is toward progressive lightening rather than the cyclical pattern of darken-treat-darken seen with conventional approaches.
Q6: Does retinol or tretinoin help with DEJ repair?
Retinoids can upregulate type IV collagen and laminin expression, and they are among the few topical agents with evidence supporting DEJ improvement. However, retinoids also thin the stratum corneum and can provoke irritation in sensitive, melasma-prone skin—potentially triggering the very inflammation that damages the DEJ. If retinoids are used, they should be introduced gradually at low concentrations and combined with robust barrier support and anti-inflammatory measures.
About the Author
Dr. Ta-Ju Liu is the founder of Liusmed Clinic in Taipei, Taiwan, where he leads a practice dedicated to regenerative medicine and minimal incision surgery. With dual expertise in dermatology and surgical repair, Dr. Liu developed the clinic's signature repair-over-destruction philosophy after observing that many refractory skin conditions—including melasma, rosacea, and filler complications—share a common root in chronic tissue-level inflammation. His clinical approach prioritizes restoring the skin's native repair mechanisms rather than adding further injury through aggressive interventional techniques.
Disclaimer
This article is provided for educational and informational purposes only and does not constitute medical advice, diagnosis, or treatment. Individual results vary based on skin type, condition severity, and treatment compliance. Always consult a qualified dermatologist or medical professional before beginning any treatment for melasma or other skin conditions. The information presented reflects the clinical perspective of the author and Liusmed Clinic as of the publication date.
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

