What Happens When Fat Grafting Goes Wrong? Deep Pathology Analysis of FOS, Calcified Lumps & Under-Eye Granulomas
Executive Summary
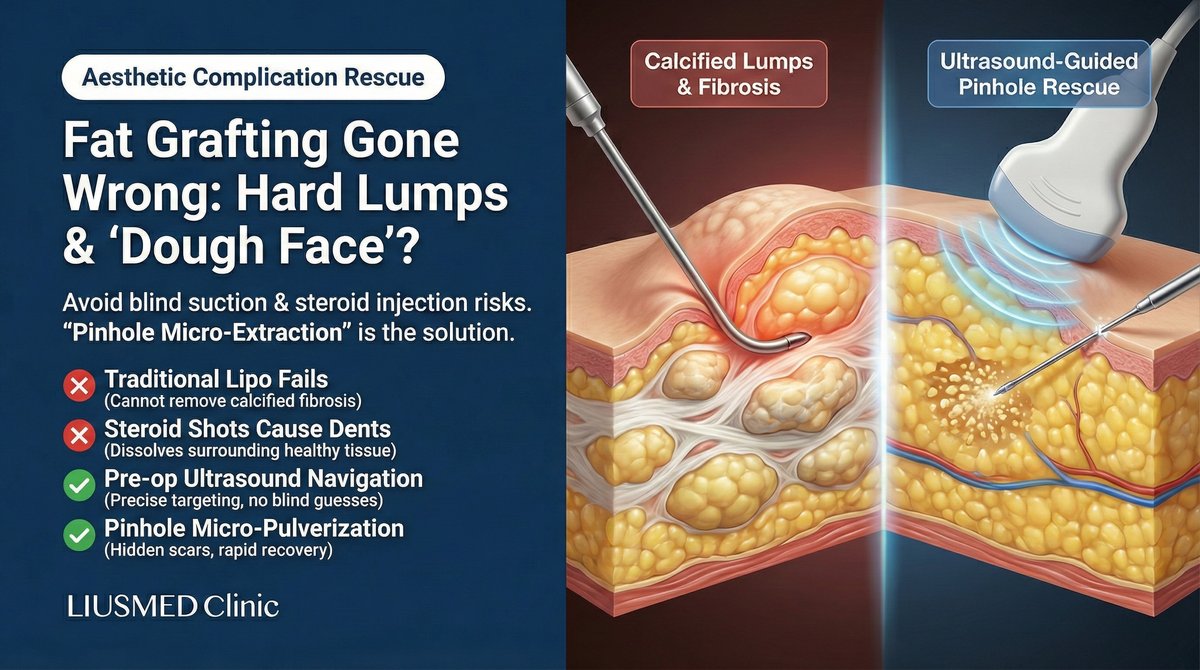
Although autologous fat grafting is heralded as "liquid gold," improper technique readily leads to Facial Overfilled Syndrome (FOS), calcified lumps, or under-eye granulomas. Dr. Ta-Ju Liu of Liusmed Clinic emphasizes that conventional liposuction or steroid injections are frequently ineffective and may even cause additional deformity. Our ultrasound-guided micro-pinhole extraction procedure precisely pulverizes and removes stubborn calcified deposits under direct visualization, restoring natural facial contours — the definitive solution for fat graft complications.
Chapter 1: The Hidden Cost of Beauty — Pathological Mechanisms Beneath the Skin
Many patients are puzzled: "Why did my fat turn hard?" or "Why does my face still look inflated even after all this time?" These outcomes are not simply a matter of bad luck — they follow a well-documented pathological pathway.
Hard Lumps and Calcified Nodules: The Battlefield of Hypoxia and Immunity
This is the complication patients fear most. According to clinical pathological analysis, when the radius of a single-point fat injection exceeds 2 mm, the core of the fat bolus cannot receive sufficient oxygen diffusion or neovascular supply within the first 48 hours, resulting in central necrosis.
Fibrous Encapsulation: Necrotic fat releases free fatty acids, triggering a sterile inflammatory response. The immune system dispatches macrophages to surround the necrotic tissue, forming a dense, rigid fibrous capsule wall. This is why the lump you feel is as hard as a "stone."
Calcification: Over time, calcium deposits accumulate within these necrotic cores, forming permanent calcification points.
Facial Overfilling (Facial Overfilled Syndrome, FOS): Destruction of Anatomical Architecture
FOS is not merely a face that looks "bigger" — it represents the loss of dynamic aesthetic quality. The root causes are over-augmentation and incorrect plane placement.
Compartment Obliteration: In pursuit of volume, excessive fat is injected into both the deep and superficial fat compartments, destroying the precisely organized "facial retaining ligament" architecture.
Expression Restriction: When fat is inadvertently injected into the muscular layer or accumulates on top of the mimetic muscles, muscular contraction meets mechanical resistance. The result is the characteristic "plastic" appearance — facial muscles bunching unnaturally with every smile.
Periorbital Complications: The Challenge of Extremely Thin Skin
The skin beneath the eye is approximately 0.5 mm thick — the thinnest skin on the entire face.
Granuloma: Uneven fat survival or focal fibrosis produces a visible "caterpillar"-like ridge that becomes apparent under directional lighting.
Permanent Edema: Excessive fat grafting compresses the delicate periorbital lymphatic network, obstructing lymphatic drainage and causing chronic, non-resolving malar edema (Malar Edema).
Chapter 2: Why Conventional Repair Methods Are Dead Ends
Faced with these challenging problems, standard market treatments frequently prove either ineffective or cause secondary harm.
Conventional Liposuction — No Match for Fibrosis (excess scar tissue formation)
Liposuction cannulas are designed to aspirate soft, mobile fat. Against dense, fibrosed lumps, the cannula simply glides over the surface without gaining purchase. Forceful manipulation only damages the surrounding healthy tissue.
Steroid Injections (Intralesional Steroids) — Killing One Hundred Enemies, Wounding Three Thousand Allies
Steroids cannot selectively target the lump. The typical outcome: the hard core persists, while the surrounding healthy fat atrophies, creating an unsightly "volcanic crater" depression.
Laser Lipolysis — The Double-Edged Sword of Thermal Energy
Dissolving calcified deposits requires elevated laser energy settings. In thin-skinned areas such as the forehead and periorbital region, this substantially increases the risk of thermal skin burns and nerve heat injury.
Open Excision — Too High a Price
Although the most thorough approach, making a 2–3 cm incision on the face and accepting a permanent scar is simply unacceptable to patients seeking aesthetic improvement.
Chapter 3: The Medical Breakthrough at Liusmed Clinic — Micro-Pinhole Extraction
Addressing the shortcomings of traditional medicine, Liusmed Clinic has introduced microsurgical principles into aesthetic repair, pioneering the Micro-Pinhole Extraction procedure.
Step 1: Pre-Operative High-Frequency Ultrasound Guidance (Visualization)
We refuse to operate blindly. Using high-resolution soft-tissue ultrasound, we perform a full-face tomographic scan before the procedure. This precisely maps the depth, nature (liquid oil cyst versus calcified lump), and surrounding vascularity of each deposit. This "navigation map" is the cornerstone of surgical success.
Step 2: Precision Micro-Dissection
When working in high-risk zones such as the forehead (supratrochlear nerve territory) and the periorbital region, safety is the paramount principle. Using specialized minimally invasive instruments, we gently dissect the lump away from the surrounding neurovascular structures, creating a safe buffer zone before any energy is applied.
Step 3: Pinhole-Sized Micro-Fragmentation and Extraction
This is the technical heart of the procedure. We abandon the crude liposuction cannula in favor of microsurgical energy devices.
In-Situ Fragmentation: Through an incision of only 1–2 mm (pinhole-sized), typically concealed within the hairline, the hardened calcified deposits are pulverized in situ beneath the skin.
Precise Aspiration: The large "stone" is broken down into fine particles before being aspirated — completely removing stubborn calcifications that even laser cannot eliminate.
Step 4: Subtractive Aesthetics and Tissue Repositioning
To address the skin laxity that results from FOS correction, we sculpt the subcutaneous space and apply skin re-adherence techniques, allowing the skin to re-adhere naturally to the deeper tissue framework, restoring the face's original, clearly defined bony contours.
Frequently Asked Questions (FAQ)
Q: My lumps have been there for years — some may even be calcified. Can they still be removed?
Yes. The longer the lumps have been present, the harder and more calcified they typically become. Conventional liposuction cannot handle them, but through our micro-pinhole fragmentation technique, we can break down calcified tissue and extract it. We have successfully treated many long-standing cases dating back 5 or even 10 years.
Q: After extraction, will my face look hollow or the skin become loose?
This depends on the repair technique employed. We use our refined tissue repositioning technique to help the skin re-adhere. If significant laxity is present, we may recommend combining the procedure with non-invasive lifting modalities to assist skin repositioning.
Q: Can this method also treat the "caterpillar" granulomas beneath my eyes?
Yes, though the degree of technical difficulty is higher. Because the under-eye skin is extremely thin, we use more refined micro-instruments. Under ultrasound guidance, we precisely remove the superficial subdermal granulomas while preserving the normal under-eye fat pad, avoiding the creation of a tear trough depression.
Q: Does the procedure require general anesthesia? How long is the recovery?
The procedure is typically performed under local anesthesia or gentle pain-relief anesthesia. Since this is a minimally invasive procedure with only pinhole-sized incisions (concealed within the hairline or in inconspicuous locations), post-operative swelling resolves in approximately 1–2 weeks, and bruising clears within approximately 2 weeks. Hospitalization is not required, and normal daily activities can be resumed shortly after surgery.
Q: Why can't I simply use steroid injections?
The risk is too high. Intralesional steroids (scar-softening injections) commonly cause surrounding normal tissue atrophy, creating "volcanic crater" depressions, and cannot truly eliminate the calcified lump core. For facial repair, we firmly adhere to the principle that physical removal is superior to chemical atrophy.
Q: How is the procedure cost calculated?
Repair surgery is highly individualized medical care. The cost depends on the extent, number, depth, and degree of calcification of the lumps. An accurate estimate can only be provided after the physician personally evaluates you through palpation and ultrasound assessment.
About the Author
Dr. Ta-Ju Liu (劉達儒醫師)
Current Position: Director, Liusmed Clinic
Specialties: Autologous fat graft complication repair, minimally invasive calcified lump extraction, Facial Overfilled Syndrome (FOS) correction
Credentials:
- Over 20 years of experience in minimally invasive surgery
- Pioneer in the development of the Micro-Pinhole Extraction technique
- Committed to "visible medicine" — integrating high-resolution ultrasound to eliminate the risks of blind aspiration
Philosophy: "Repair is about helping you make peace with the person you see in the mirror. Using the most refined microsurgical techniques, we remove what burdens you while protecting your natural appearance — so you can rediscover yourself."
Related Services
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

