Beyond Blind Bombardment: How Dr. Liu's Hydro-Dissection Manual Technique Precisely Breaks Through Melasma Adhesions
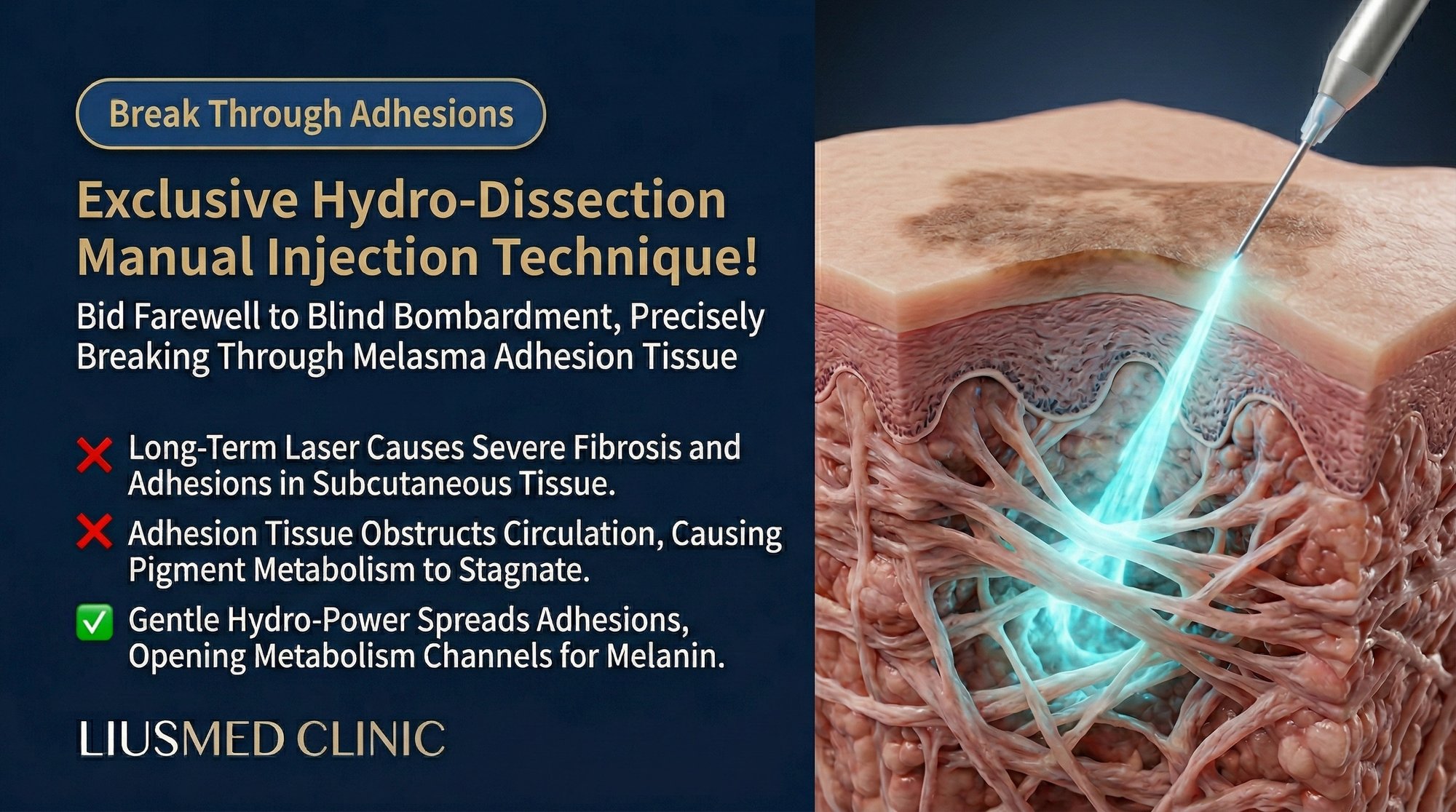
Lasers fire energy blindly through the skin surface, hoping to hit the right target at the right depth. The hydro-dissection technique works in the opposite direction — the physician's hand is the guidance system, using fluid pressure to physically separate the tissue planes where melasma lives, releasing trapped pigment and delivering treatment simultaneously.
Table of Contents
- The Problem with Bombardment: Why Surface-Fired Energy Fails in Melasma
- Dermal Adhesions and Fibrosis (excess scar tissue formation): The Hidden Architecture of Chronic Melasma
- What Is Hydro-Dissection? Principles and Origins
- Dr. Liu's Adaptation: Hydro-Dissection for Melasma Treatment
- Step-by-Step: How the Technique Is Performed
- Clinical Advantages Over Conventional Approaches
The Problem with Bombardment: Why Surface-Fired Energy Fails in Melasma
Laser treatment for hyperpigmentation operates on a conceptually simple principle: fire energy through the skin surface, and the chromophore (melanin) absorbs it and is destroyed. For discrete, well-defined pigmented lesions — sun spots, lentigines, cafe-au-lait macules — this approach is remarkably effective.
Melasma presents a fundamentally different challenge. The pigment is not a discrete target sitting at a defined depth. Instead, it is diffusely distributed across variable depths within an inflamed, hypervascular dermal environment. The melanin exists in two forms: active melanin within melanocytes and keratinocytes (epidermal component) and phagocytosed melanin trapped within dermal macrophages (dermal component).
When laser energy enters this complex tissue environment, several problems arise simultaneously. The energy is absorbed non-selectively by melanin at multiple depths, generating heat that spreads through the surrounding dermis. This thermal energy triggers inflammation — the very process driving melasma in the first place. The immature, leaky vessels characteristic of melasma skin are particularly vulnerable to heat-induced damage, releasing inflammatory mediators that amplify the post-treatment response.
Furthermore, the laser beam has no way to discriminate between melanin in a melanocyte (productive target) and melanin trapped in a dermal macrophage embedded within fibrotic tissue (unproductive target). Energy deposited in fibrotic dermis generates heat without therapeutic benefit while contributing to the inflammatory rebound.
The fundamental limitation is this: surface-fired energy cannot account for the three-dimensional tissue architecture of melasma. It treats skin as a flat, uniform medium when in reality melasma creates a complex, heterogeneous microenvironment with adhesions, fibrosis, and variable pigment distribution.
Dermal Adhesions and Fibrosis: The Hidden Architecture of Chronic Melasma
Long-standing melasma is not simply a collection of excess pigment. Over months and years, the chronic inflammatory process creates structural changes in the dermis that contribute significantly to treatment resistance.
Dermal fibrosis develops as fibroblasts, stimulated by chronic inflammation, deposit excess collagen in a disorganized pattern. This creates areas of dense, stiff tissue that differ markedly from the elastic, organized collagen of normal dermis. Within these fibrotic zones, melanin-laden macrophages (melanophages) become physically trapped, unable to migrate toward lymphatic drainage pathways that would normally clear them.
Tissue adhesions form between the papillary and reticular dermis as inflammatory cross-linking binds tissue planes that are normally loosely connected. These adhesions restrict the natural mobility of the tissue, creating compartments where melanophages, inflammatory cells, and stagnant tissue fluid accumulate.
Perivasular fibrosis develops around the abnormal blood vessels in melasma skin, encasing them in a collagen sheath that protects them from the body's normal vascular pruning mechanisms. This is one reason why the hypervascular component of melasma persists even when anti-angiogenic treatments are applied topically — the target vessels are shielded by fibrotic tissue.
These structural changes explain why some melasma cases become progressively more resistant to treatment over time. It is not that the melanocytes become more active — it is that the dermal microenvironment becomes increasingly fortified, trapping existing pigment and shielding the pathological vasculature from therapeutic agents.
| Structural Change | Location | Effect on Treatment | Impact on Pigment Clearance |
|---|---|---|---|
| Dermal fibrosis | Papillary and upper reticular dermis | Blocks drug diffusion | Traps melanophages in dense matrix |
| Tissue adhesions | Between dermal layers | Creates isolated compartments | Prevents lymphatic drainage of debris |
| Perivascular fibrosis | Around dermal vessels | Shields vessels from topical agents | Maintains inflammatory vascular supply |
| Basement membrane disruption | Dermo-epidermal junction | Allows ongoing pigment leakage | Continuous new dermal pigment deposition |
| Mast cell clustering | Perivascular and perilesional | Maintains inflammatory signaling | Sustains melanocyte activation |
What Is Hydro-Dissection? Principles and Origins
Hydro-dissection is a surgical technique that uses the controlled injection of fluid to separate tissue planes. The pressurized fluid acts as a dissecting tool, finding and opening natural cleavage planes between tissue layers while preserving the integrity of the tissues on either side.
The technique has a long history in surgery. In orthopedics, hydro-dissection is used to release peripheral nerves from surrounding adhesions. In interventional pain management, it separates compressed nerves from adjacent structures. In ophthalmology, a variant of the technique is used during cataract surgery to separate the lens cortex from its capsule.
The principle is consistent across all applications: fluid pressure is a gentler and more precise dissecting force than mechanical cutting or thermal energy. The fluid naturally follows paths of least resistance, preferentially separating loosely connected tissue planes while leaving densely connected structures intact. This selectivity makes hydro-dissection inherently safer and more tissue-preserving than blunt dissection or energy-based techniques.
When applied to dermal tissue, hydro-dissection offers unique capabilities. The injected fluid simultaneously separates tissue planes, dilates the space between layers (creating room for therapeutic agents to distribute), and physically displaces trapped cellular debris. If the fluid itself contains therapeutic agents — as in the Liusmed protocol — the dissection and treatment occur in a single step.
Dr. Liu's Adaptation: Hydro-Dissection for Melasma Treatment
Dr. Liu recognized that the structural pathology of chronic melasma — fibrosis, adhesions, and trapped melanophages — represented the same type of tissue problem that hydro-dissection addresses in surgical contexts. The innovation was adapting this surgical principle to the superficial dermis using manual mesotherapy technique.
In the Melasma Injection Treatment protocol, the hydro-dissection component serves multiple simultaneous purposes:
Adhesion release. The pressurized injection of the treatment cocktail physically separates fibrotic adhesions between tissue planes. This opens channels for lymphatic drainage and cellular migration, allowing trapped melanophages to be gradually cleared by the body's immune system.
Therapeutic distribution. By opening tissue planes, the fluid carries the treatment agents (TXA, PRP, anti-inflammatory cocktail) into areas that would otherwise be inaccessible. Dense fibrotic tissue that blocks topical drug penetration and resists passive diffusion is physically opened by the hydro-dissection effect, allowing direct drug contact with the pathological tissue.
Mechanical debulking. The fluid pressure physically displaces accumulated inflammatory debris, stagnant tissue fluid, and loose melanin granules from the treatment zone. This reduces the local concentration of pro-inflammatory mediators and creates a cleaner microenvironment for the regenerative process.
Tissue plane mapping. As the physician performs the injection, the resistance felt through the syringe provides real-time information about the tissue architecture. Areas of dense fibrosis resist fluid injection, requiring more pressure. Normal tissue accepts fluid easily. This tactile mapping allows the physician to identify and specifically target areas of pathological fibrosis — something no imaging technique or automated device can replicate during treatment.
Step-by-Step: How the Technique Is Performed
The hydro-dissection component of the Liusmed protocol follows a systematic approach:
Assessment phase. Before injection, the treatment area is assessed using dermoscopy and palpation. Dermoscopy identifies the vascular and pigmentary pattern, while palpation reveals areas of subclinical fibrosis (hardened tissue that can be felt but not seen). These findings create a mental map that guides the injection strategy.
Superficial pass. Using a 30G or 32G needle at a shallow angle, the physician performs an initial series of injections in the papillary dermis. This layer is where melanocyte-keratinocyte interaction occurs and where the basement membrane zone is located. The fluid in this pass contains the anti-inflammatory and TXA components. Injection resistance is noted at each point to map the fibrosis distribution.
Targeted hydro-dissection pass. Based on the resistance map generated during the superficial pass, the physician returns to areas of identified fibrosis and performs controlled hydro-dissection. The needle is advanced into the fibrotic zone and fluid is injected with deliberate pressure, separating the adhesed tissue planes. The physician can feel the moment of release as the resistance drops and the fluid begins to flow freely into the opened space.
PRP delivery pass. With the tissue planes now opened and the fibrotic barriers partially disrupted, high-concentration PRP (Platelet-Rich Plasma — concentrate of your own blood platelets rich in growth factors) is delivered into the treated zones. The pre-existing fluid channels created by the hydro-dissection allow the PRP to distribute widely through previously inaccessible tissue, maximizing contact between growth factors and target cells.
Post-treatment assessment. The treated area is examined for uniform fluid distribution (visible as slight tissue edema) and absence of excessive bleeding or hematoma. The temporary swelling from the injected fluid resolves within hours as the fluid is absorbed.
Clinical Advantages Over Conventional Approaches
The hydro-dissection manual technique offers several measurable advantages over both laser-based and standard mesotherapy approaches.
Three-dimensional treatment. Unlike lasers, which fire in a straight line from the surface, hydro-dissection distributes therapeutic agents through the full three-dimensional volume of the melasma lesion. The fluid follows natural tissue planes, reaching areas that surface-fired energy cannot access without collateral damage.
Structural remodeling. No other melasma treatment technique directly addresses dermal adhesions and fibrosis. Lasers can theoretically remodel collagen through thermal injury, but in melasma this thermal effect triggers counterproductive inflammation. Hydro-dissection releases adhesions mechanically, without thermal energy and without inflammatory consequence.
Enhanced drug delivery. The tissue planes opened by hydro-dissection create channels that dramatically improve the distribution and penetration of therapeutic agents compared to standard intradermal injection. This means each molecule of TXA and each platelet in the PRP preparation reaches more pathological tissue.
Melanophage liberation. By breaking the fibrotic cage surrounding trapped melanophages, hydro-dissection allows the body's lymphatic system to gradually clear these pigment-laden cells. This mechanism of pigment reduction is entirely different from melanin destruction by laser — it works with the body's clearance systems rather than against them.
Physician-guided precision. The tactile feedback inherent in manual technique provides treatment information that no device can generate. The physician's hand serves simultaneously as sensor, guidance system, and delivery tool — adapting in real time to the unique tissue architecture of each patient.
| Treatment Aspect | Laser Toning | Standard Mesotherapy | Hydro-Dissection Manual Technique |
|---|---|---|---|
| Addresses fibrosis | No | Partially (drug effect only) | Yes (mechanical + pharmaceutical) |
| Adhesion release | No | No | Yes |
| Drug distribution depth | N/A | Limited to injection point | Extended through opened tissue planes |
| Melanophage clearance | Attempts melanin destruction | Indirect (reduces production) | Direct mechanical liberation |
| Real-time tissue feedback | None | Minimal | Extensive tactile mapping |
| Inflammatory risk | High (thermal injury) | Low | Very low |
| Collagen remodeling | Thermal (inflammatory) | Growth factor-mediated | Mechanical + growth factor-mediated |
Frequently Asked Questions
Q1: What does hydro-dissection feel like during treatment?
Patients typically feel a sensation of pressure or fullness as the fluid is injected and distributes through the tissue. The sensation is distinct from the pinprick of the needle itself. Some patients describe it as a temporary swelling feeling. The sensation resolves quickly as the fluid is absorbed, usually within a few hours after treatment.
Q2: Is hydro-dissection safe? Can it damage nerves or blood vessels?
The technique uses fine needles at superficial dermal depth (less than 1 mm from the skin surface). At this depth, there are no significant nerve trunks or large blood vessels. The fluid pressure used is controlled and gentle — sufficient to separate tissue planes but not to cause tissue disruption. The technique has been used safely in various surgical specialties for decades.
Q3: How is this different from regular mesotherapy injections?
Standard mesotherapy delivers a drug at a point and relies on passive diffusion for distribution. Hydro-dissection uses the injected fluid as an active tool to physically separate tissue planes, break adhesions, and create channels for enhanced drug distribution. The result is broader, deeper, and more uniform drug delivery to the pathological tissue.
Q4: Can any practitioner perform hydro-dissection for melasma?
The technique requires significant experience with manual mesotherapy and a detailed understanding of facial dermal anatomy. The tactile skills needed to interpret tissue resistance and adjust injection parameters in real time cannot be learned from textbooks alone. Physicians trained specifically in this technique by Dr. Liu's methodology are best qualified to perform it.
Q5: How many sessions include the hydro-dissection component?
In the Melasma Injection Treatment protocol, the hydro-dissection component is incorporated into every treatment session. However, the intensity and focus of the hydro-dissection varies based on the degree of fibrosis present. Early sessions may require more aggressive adhesion release, while later sessions focus more on maintenance and regenerative support.
Q6: Will the adhesions come back after treatment?
The adhesions formed in chronic melasma are a product of the inflammatory environment. As the anti-inflammatory and regenerative components of the protocol normalize the dermal microenvironment, the conditions that created the adhesions are progressively eliminated. With continued treatment and appropriate maintenance, recurrence of significant fibrosis is uncommon provided that the inflammatory triggers (UV exposure, hormonal factors) are managed.
About the Author
Dr. Ta-Ju Liu is the founder of Liusmed Clinic and a specialist in regenerative medicine and minimal incision surgery. Drawing on his surgical training and experience with tissue dissection techniques, Dr. Liu adapted hydro-dissection principles for dermatological application, creating a treatment approach that addresses the structural pathology of melasma that other treatments cannot reach. Liusmed Clinic combines surgical precision with regenerative medicine to deliver outcomes that transcend conventional dermatology.
Disclaimer
This article is provided for educational and informational purposes only. It does not constitute medical advice, diagnosis, or treatment. The hydro-dissection technique described requires specialized training and should only be performed by qualified medical professionals. Individual results vary based on the severity, duration, and specific characteristics of each patient's condition. Consult a qualified healthcare professional before making any treatment decisions.
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

