What Is the Liusmed Melasma Injection? The Anti-Inflammatory and Regenerative Mechanism of PRP-Enhanced Manual Mesotherapy
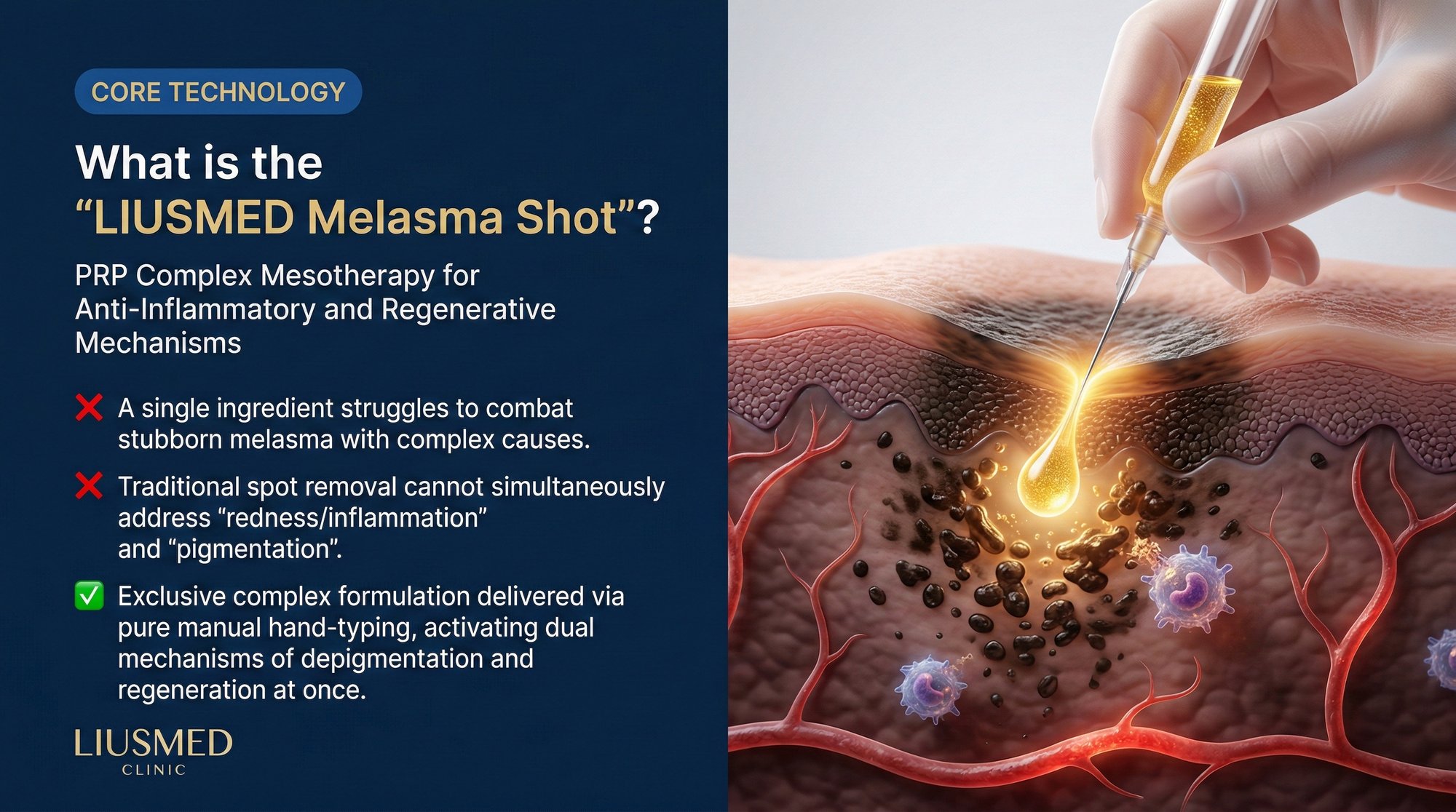
Most melasma treatments fail because they aim at the wrong target. Lasers blast pigment. Topical creams bleach the surface. But the engine driving melasma — chronic dermal inflammation, leaky blood vessels, and a broken basement membrane — keeps running underneath. The Liusmed Melasma Injection was designed to shut down that engine.
Table of Contents
- Why Conventional Melasma Treatments Hit a Ceiling
- The Core Pathology: Inflammation, Vascular Dysfunction, and Barrier Collapse
- How the Liusmed Melasma Injection Works: A Three-Layer Protocol
- PRP (Platelet-Rich Plasma — concentrate of your own blood platelets rich in growth factors) as the Regenerative Catalyst: Beyond Simple Growth Factors
- Manual Mesotherapy (shallow micro-injection of nutrients/meds) vs. Machine Delivery: Why Precision Matters
- Clinical Outcomes and What to Expect
Why Conventional Melasma Treatments Hit a Ceiling
For decades, the dermatology world treated melasma as a pigment problem. The logic was straightforward: melanin is dark, so destroy the melanin. Lasers, intense pulsed light (IPL), and depigmenting agents all follow this reasoning. And for superficial sun spots or freckles, this approach works well.
Melasma, however, is not a simple pigment problem. It is an inflammatory and vascular disorder that happens to produce visible pigment as a downstream symptom. Research published over the past decade has consistently shown that melasma skin contains increased mast cell infiltration, elevated vascular endothelial growth factor (VEGF), and a structurally compromised dermo-epidermal junction.
When lasers target melanin in this environment, they generate additional heat-induced inflammation. The body responds by producing more melanin — the very substance the treatment was supposed to eliminate. This is why so many melasma patients experience the devastating cycle of temporary improvement followed by rebound hyperpigmentation.
The Liusmed Melasma Injection protocol was developed specifically to break this cycle by addressing the inflammatory microenvironment rather than chasing pigment.
The Core Pathology: Inflammation, Vascular Dysfunction, and Barrier Collapse
Understanding why the Liusmed protocol works requires understanding the three pillars of melasma pathology:
Chronic dermal inflammation. Melasma skin shows elevated levels of inflammatory mediators including prostaglandins, stem cell factor (SCF), and various interleukins. These signals continuously stimulate melanocytes to overproduce pigment, regardless of how much melanin has been removed from the surface.
Vascular dysfunction and angiogenesis. Studies using dermoscopy and histology have demonstrated that melasma lesions contain significantly more blood vessels than surrounding normal skin. These new, immature vessels leak inflammatory mediators into the dermis and create a self-perpetuating cycle of inflammation and pigment production.
Basement membrane disruption. The basement membrane zone (BMZ) acts as a critical barrier between the epidermis and dermis. In melasma, this barrier is frequently damaged, allowing melanin granules to drop into the dermis where they are engulfed by dermal macrophages — creating the stubborn dermal pigmentation that resists virtually all topical treatments.
| Pathological Feature | Role in Melasma | Conventional Treatment Response | Liusmed Protocol Response |
|---|---|---|---|
| Dermal inflammation | Drives melanocyte activation | Often worsened by laser heat | Directly suppressed by TXA + anti-inflammatory cocktail |
| Abnormal angiogenesis | Feeds inflammatory loop | Not addressed | Blocked by tranexamic acid at vascular level |
| Basement membrane damage | Allows pigment to drop into dermis | Not addressed | Repaired by PRP growth factors |
| Surface melanin | Visible symptom | Destroyed (temporarily) | Gradually cleared as root causes resolve |
| Mast cell infiltration | Releases histamine and VEGF | May be triggered by thermal injury | Reduced by anti-inflammatory protocol |
How the Liusmed Melasma Injection Works: A Three-Layer Protocol
The Melasma Injection Treatment is not a single substance injected blindly. It is a carefully sequenced, multi-layer manual mesotherapy protocol that addresses each pathological layer in turn.
Layer 1: Anti-inflammatory suppression. A precisely formulated cocktail containing tranexamic acid (TXA) and selected anti-inflammatory agents is delivered into the superficial dermis using manual injection technique. TXA works by blocking plasminogen activation, which in turn reduces the production of prostaglandins and VEGF (Vascular Endothelial Growth Factor — new blood vessel signal). This directly interrupts the inflammatory signaling cascade that drives melanocyte hyperactivity.
Layer 2: Vascular normalization. The same manual delivery ensures that TXA reaches the perivascular space where it can directly inhibit the formation of new, leaky blood vessels. Unlike oral TXA, which distributes systemically at low concentrations, intradermal injection places therapeutic concentrations exactly where pathological angiogenesis occurs.
Layer 3: Regenerative repair with PRP. High-concentration platelet-rich plasma is prepared from the patient's own blood and introduced into the treatment zone. The growth factors released by activated platelets — including PDGF (Platelet-Derived Growth Factor — platelet-released cell growth signal), TGF-beta, and EGF (Epidermal Growth Factor) — stimulate fibroblast activity, promote collagen synthesis at the dermo-epidermal junction, and support repair of the damaged basement membrane.
This three-layer approach means the protocol simultaneously suppresses the disease process, normalizes the vascular environment, and rebuilds the structural barriers that prevent recurrence.
PRP as the Regenerative Catalyst: Beyond Simple Growth Factors
PRP has gained widespread attention in aesthetics, but not all PRP applications are equal. The Liusmed protocol uses PRP in a fundamentally different way than typical "vampire facial" treatments.
First, the concentration matters. Standard PRP preparation yields approximately 2-3x baseline platelet concentration. The Liusmed protocol uses a preparation method that achieves significantly higher concentrations, which translates to a proportionally greater release of regenerative growth factors.
Second, the delivery method matters. When PRP is applied topically after microneedling (the most common aesthetic application), the majority of growth factors never penetrate deep enough to reach the damaged basement membrane zone. Manual intradermal injection places PRP directly at the target depth where basement membrane repair is needed.
Third, the timing matters. In the Liusmed protocol, PRP is introduced after the anti-inflammatory cocktail has begun suppressing the inflammatory environment. This means the regenerative growth factors are working in a calmed microenvironment rather than fighting against active inflammation — dramatically improving their effectiveness.
The regenerative cascade initiated by properly delivered PRP includes stimulation of type IV collagen synthesis (the primary structural protein of the basement membrane), recruitment of local stem cells, and modulation of the immune microenvironment toward repair rather than chronic inflammation.
Manual Mesotherapy vs. Machine Delivery: Why Precision Matters
A critical differentiator of the Liusmed protocol is the insistence on manual injection technique rather than machine-assisted delivery systems such as mesotherapy guns or automated microneedling devices.
Machine delivery systems offer speed and consistency, but they sacrifice the most important variable in melasma treatment: depth control. Melasma lesions vary in depth not only from patient to patient, but from area to area within the same patient's face. The malar region typically shows different pathology than the forehead or upper lip.
With manual technique, the treating physician can feel the tissue resistance change as the needle passes through different layers. This tactile feedback allows real-time adjustment of injection depth, ensuring that the therapeutic cocktail reaches the correct tissue plane for each specific area.
Furthermore, manual injection allows the physician to create a controlled hydro-dissection effect — using the fluid itself to gently separate tissue planes and break up areas of dermal fibrosis that trap pigment-laden macrophages. Machine delivery cannot replicate this technique.
The trade-off is that manual mesotherapy requires significantly more skill and experience than operating a machine. Each session takes longer. But for a condition as complex and treatment-resistant as melasma, this precision is not optional — it is essential.
Clinical Outcomes and What to Expect
Patients undergoing the Melasma Injection Treatment typically notice initial changes within 7 to 14 days after the first session. The earliest visible change is usually a reduction in the redness or vascular component of the melasma, reflecting the anti-inflammatory and anti-angiogenic effects of TXA.
Pigment lightening follows more gradually, typically becoming apparent after 2 to 3 sessions spaced 3 to 4 weeks apart. This slower timeline reflects the fact that the protocol is not destroying pigment directly but rather shutting down pigment production and allowing the body's natural turnover mechanisms to clear existing melanin.
Most patients achieve satisfactory improvement within 4 to 6 sessions. However, because melasma is a chronic condition influenced by hormonal status, UV exposure, and genetic predisposition, a maintenance strategy is essential for long-term results.
The recovery profile is notably mild compared to laser treatments. Most patients experience mild redness and pinpoint injection marks that resolve within 24 to 48 hours. There is no significant downtime, and patients can return to normal activities immediately. Crucially, there is no risk of post-inflammatory hyperpigmentation — the complication that makes laser treatment of melasma so problematic.
Frequently Asked Questions
Q1: How is the Liusmed Melasma Injection different from laser toning for melasma?
Laser toning targets melanin with thermal energy, which can trigger rebound inflammation and worsened pigmentation in melasma patients. The Liusmed Melasma Injection targets the inflammatory and vascular root causes driving melanin overproduction. Rather than destroying pigment from the outside, it shuts down the mechanisms that produce excess pigment in the first place, while simultaneously repairing the structural barriers that prevent recurrence.
Q2: Is PRP safe for melasma treatment?
PRP is derived from the patient's own blood, making allergic reactions virtually impossible. The preparation process concentrates platelets and growth factors while removing red and white blood cells. When delivered by trained physicians using proper sterile technique, PRP has an excellent safety profile with decades of clinical use across multiple medical specialties.
Q3: Why is manual injection preferred over machine-assisted delivery?
Manual injection allows the physician to adjust depth, pressure, and volume in real time based on tactile feedback from the tissue. Melasma varies in depth and severity across different facial zones, and this precision ensures the therapeutic agents reach the correct tissue plane. Machine delivery offers speed but sacrifices the depth control that is critical for effective melasma treatment.
Q4: Can I continue using my current skincare products during treatment?
Most gentle skincare routines can continue. However, active ingredients such as retinoids, high-concentration vitamin C, and chemical exfoliants should be paused for 48 hours before and after each session. Your treating physician will provide specific guidance based on your current regimen during the consultation.
Q5: How long do results last after completing the treatment course?
With proper sun protection and a maintenance skincare regimen, results can be sustained for 12 months or longer. Because melasma is a chronic condition, periodic maintenance sessions (typically every 3 to 6 months) are recommended to reinforce the anti-inflammatory and regenerative benefits. Hormonal changes, unprotected sun exposure, and certain medications can influence longevity of results.
Q6: Is the Liusmed Melasma Injection suitable for darker skin tones?
Yes. One of the significant advantages of this protocol over laser-based treatments is its safety across all Fitzpatrick (Fitzpatrick Skin Type) skin types. Because the treatment does not generate thermal injury, the risk of post-inflammatory hyperpigmentation — which disproportionately affects darker skin tones — is essentially eliminated. The anti-inflammatory mechanism is beneficial regardless of skin type.
About the Author
Dr. Ta-Ju Liu is the founder of Liusmed Clinic and a specialist in regenerative medicine and minimal incision surgery. With extensive clinical experience in PRP-based therapies and manual mesotherapy techniques, Dr. Liu developed the Liusmed Melasma Injection protocol to address the root inflammatory and vascular causes of melasma that conventional treatments fail to resolve. Liusmed Clinic is dedicated to evidence-based, minimally invasive approaches that prioritize tissue repair and long-term outcomes over short-term cosmetic fixes.
Disclaimer
This article is provided for educational and informational purposes only. It does not constitute medical advice, diagnosis, or treatment. Individual results vary, and all medical procedures carry inherent risks. Consult a qualified healthcare professional before making any decisions regarding medical treatment. The information presented reflects clinical experience and published research as of the date of publication and may not reflect the most current developments.
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

