Why Liusmed Insists on Manual Injection Over Machine-Driven Meso Guns: The Zero-Leakage Artisan Technique
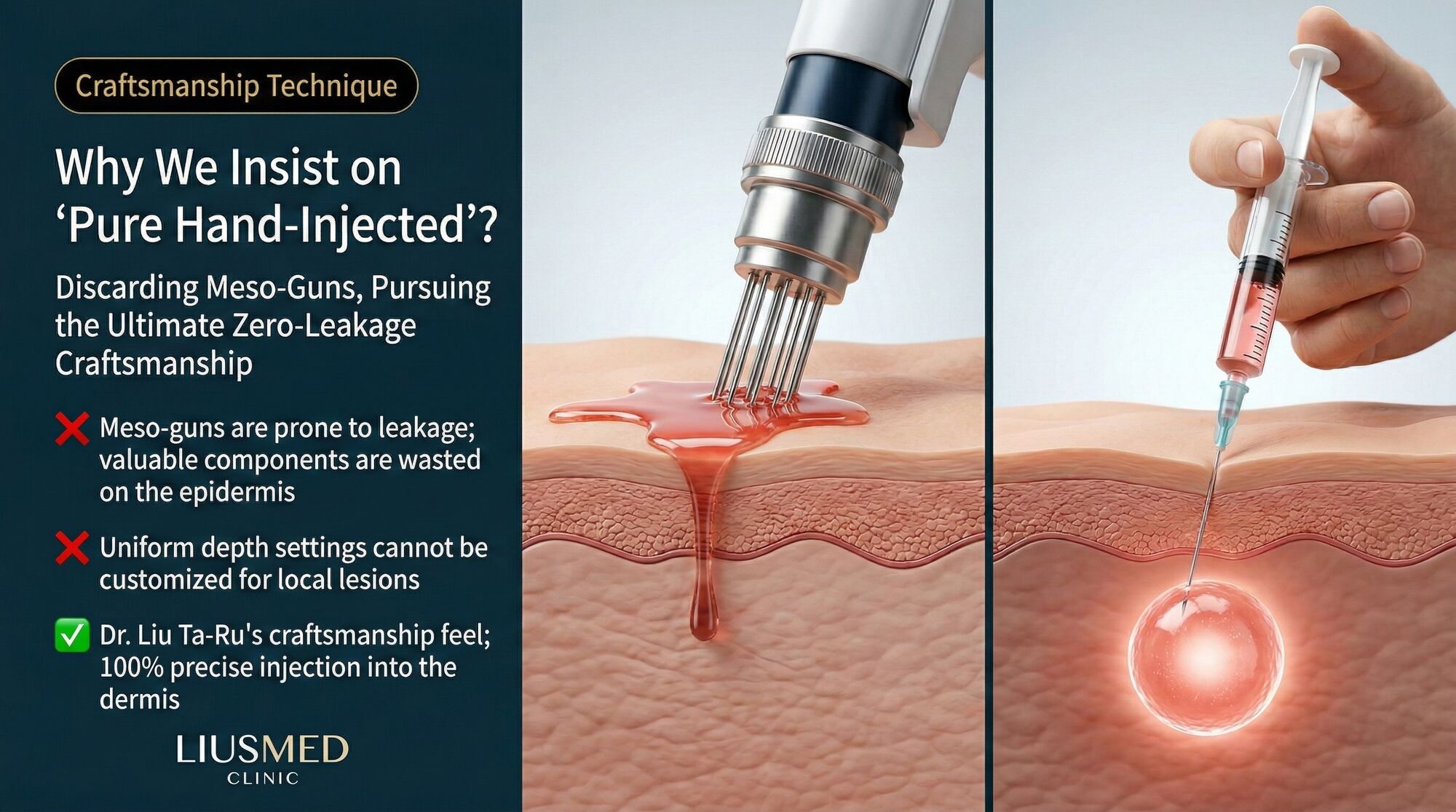
In the world of aesthetic and regenerative medicine, a quiet arms race has been underway for over a decade: the push to automate mesotherapy. Machine-driven injection devices -- variously marketed as water light guns, meso guns, vital injectors, or automated microneedling platforms -- promise speed, consistency, and reduced operator dependence. For many cosmetic applications, these devices perform adequately. But for rosacea treatment, where the target tissue is pathologically altered, the margin for error is microscopic, and the difference between therapeutic delivery and wasted product can be measured in fractions of a millimeter, automation introduces compromises that manual technique avoids entirely.
This article explains why Liusmed Clinic made the deliberate decision to reject machine-driven injection for its rosacea protocol and what the zero-leakage artisan technique actually involves.
Table of Contents
- The Rise of Automated Meso Devices
- The Problem with Mechanical Consistency in Pathological Skin
- What Zero-Leakage Injection Actually Means
- The Manual Technique: Nappage, Papule, and Point-by-Point
- Head-to-Head: Manual vs. Machine Across Key Parameters
- Why Delivery Method Determines Treatment Outcome
The Rise of Automated Meso Devices
Automated mesotherapy devices entered the market in the early 2010s with a compelling value proposition: standardize the injection process, reduce treatment time, minimize operator skill dependence, and improve patient comfort through vacuum-assisted needle insertion. The most widely adopted devices use either a multi-needle head (typically five or nine needles in a circular or linear array) or a single-needle motorized handpiece that drives the needle in and out at high frequency while a pump delivers a preset volume per injection cycle.
For hydration treatments, skin boosters, and general rejuvenation applications where the goal is broad, relatively uniform distribution of a hydrating agent across the face, these devices work well. The active agents (typically hyaluronic acid, vitamins, or amino acid cocktails) are forgiving of minor depth variations and do not require precise compartmental delivery to achieve their intended effect.
The problem emerges when these same devices are applied to therapeutic contexts where precision is not a convenience but a requirement.
The Problem with Mechanical Consistency in Pathological Skin
Rosacea skin is not normal skin. This seemingly obvious statement has profound implications for injection technique:
Variable thickness. Chronic rosacea causes uneven dermal thinning. Areas of active inflammation may be edematous and temporarily thickened, while adjacent chronic zones may be atrophied and paper-thin. The difference in tissue thickness between an inflamed cheek and an atrophic perinasal zone can be substantial -- yet a machine delivers the same needle depth to both.
Altered tissue density. Fibrotic areas within rosacea skin offer more resistance to needle penetration than healthy tissue. Edematous areas offer less. A manually guided needle transmits this information through tactile feedback; an automated device overrides it with mechanical force.
Fragile vasculature. The dilated, structurally weakened vessels in rosacea skin are more prone to needle injury than normal dermal capillaries. A skilled manual injector can feel the subtle give when a needle approaches a vessel and adjust trajectory. A mechanical device cannot.
Inflammatory sensitivity. Rosacea skin mounts an exaggerated inflammatory response to trauma. The repetitive high-speed needle strikes of an automated device create more cumulative micro-trauma than the slow, controlled insertions of manual technique. More trauma means more post-treatment inflammation, which is counterproductive in a condition defined by excessive inflammation.
Irregular treatment zones. The nasal sidewall, the nasolabial fold, the periorbital margin, and the chin crease each present unique angles, curves, and tissue depths. A manual injector approaches each zone with adapted technique. An automated handpiece maintains the same mechanical parameters regardless of anatomical context.
The device industry addresses some of these concerns with adjustable depth settings and multi-speed motors. But adjustability is not the same as adaptability. Changing a dial before treating a new zone is fundamentally different from continuously adjusting in real time as the needle moves through heterogeneous tissue.
What Zero-Leakage Injection Actually Means
The term "zero-leakage" in the Liusmed protocol refers to a specific technical objective: ensuring that the entirety of the injected formulation remains in the target tissue plane (the papillary dermis at the dermo-epidermal junction level) rather than leaking back through the needle track to the skin surface or diffusing into the deeper reticular dermis where it is less effective.
Leakage is the silent efficiency killer in mesotherapy. When a needle punctures the skin and delivers fluid, the subsequent withdrawal of the needle leaves a channel through which fluid can escape back to the surface via hydrostatic pressure. This is especially problematic when:
- The injection volume per point is large relative to the tissue's capacity to absorb it
- The needle withdrawal is rapid, leaving the channel patent before tissue elasticity can seal it
- The injection depth is too shallow, placing the fluid bolus close to the surface with minimal tissue above to retain it
- The injection pressure is excessive, creating a higher-pressure bolus that actively seeks the path of least resistance back out
Machine-driven devices are inherently susceptible to leakage for several reasons. The rapid needle cycling (some devices operate at over 100 insertions per minute) does not allow tissue to seal between punctures. The fixed volume delivery does not account for tissue saturation. The mechanical withdrawal speed is constant regardless of tissue characteristics. And the vacuum-assisted mechanism that some devices use to stabilize the skin can actually create negative pressure that draws fluid toward the surface.
Manual injection achieves zero-leakage through technique:
- Slow insertion at a precise angle, allowing the needle to part tissue rather than tear it
- Controlled bolus delivery with thumb pressure calibrated to the resistance felt through the syringe
- Deliberate pause after delivery to allow the fluid to begin distributing before the needle is withdrawn
- Slow withdrawal with slight angulation change to allow the tissue tract to collapse and seal
- Volume limitation per point, never exceeding what the local tissue can accommodate
The result is that virtually 100% of the injected formulation remains in the target tissue. Nothing is wasted on the skin surface. Nothing pools in the wrong compartment. Every microliter reaches its intended destination.
The Manual Technique: Nappage, Papule, and Point-by-Point
The manual mesotherapy technique used at Liusmed Clinic for the Rosacea Injection Treatment employs three classical injection modalities, selected and adapted based on the treatment zone and the specific agents being delivered:
Nappage technique. The needle is held at a very shallow angle (approximately 10 to 15 degrees to the skin surface) and advanced tangentially through the superficial dermis while the operator delivers a continuous micro-stream of fluid. This creates a linear track of deposited agent at a uniform and extremely superficial depth. Nappage is used for broad-area delivery of TXA (Tranexamic Acid) and hyaluronic acid in zones where even distribution is the priority.
Papule technique. The needle is inserted perpendicularly to a depth of 1 to 2 millimeters, a small volume (0.02 to 0.05 mL) is delivered to create a visible wheal or papule in the dermis, and the needle is withdrawn slowly. The resulting papule is a controlled depot of active agent that gradually diffuses into the surrounding tissue over the following hours. This technique is used for concentrated delivery of growth factor preparations at specific points of maximum pathology.
Point-by-point technique. Individual injections are placed at precise points mapped by the treating physician based on the clinical assessment -- typically targeting zones of maximum erythema, visible telangiectasia clusters, or areas of greatest barrier dysfunction. Each point receives a customized volume based on the tissue characteristics at that specific location. This is the most operator-dependent technique and the one that benefits most from manual control.
In a typical rosacea treatment session, all three techniques may be used across different facial zones. The physician transitions between techniques seamlessly, guided by continuous visual and tactile assessment of the tissue response. This level of adaptive, zone-specific treatment is simply not possible with a mechanical device that operates in a single modality.
Head-to-Head: Manual vs. Machine Across Key Parameters
| Parameter | Manual Injection | Automated Meso Gun |
|---|---|---|
| Depth control | Continuous real-time adjustment | Fixed or stepped depth settings |
| Tissue feedback | Full tactile sensation through needle and syringe | None; mechanical override |
| Volume per point | Variable, operator-controlled (0.01-0.05 mL) | Fixed per cycle; same volume regardless |
| Leakage rate | Near zero with proper technique | 10-30% estimated surface reflux |
| Treatment speed | Slower (30-45 minutes full face) | Faster (15-20 minutes full face) |
| Operator skill requirement | High; years of training | Low; minimal technique variation |
| Adaptation to facial zones | Continuous angle, depth, and technique changes | Limited; same parameters across zones |
| Tissue trauma | Minimal; controlled insertion and withdrawal | Higher; rapid repetitive puncture |
| Post-treatment inflammation | Mild; proportional to actual therapeutic delivery | Moderate; includes trauma-driven inflammation |
| Vessel injury risk | Low; operator avoids vessels by feel | Higher; mechanical insertion is blind |
| Cost per session | Higher (time-intensive) | Lower (faster throughput) |
| Suitable for rosacea skin | Optimal; adapts to pathological variation | Suboptimal; does not accommodate tissue heterogeneity |
The speed advantage of automated devices is real and explains their commercial popularity. For clinics optimizing patient throughput in cosmetic hydration treatments, the time savings are significant. But in a therapeutic context where efficacy depends on precision delivery to a specific tissue compartment in pathologically altered skin, speed is the wrong metric to optimize.
Why Delivery Method Determines Treatment Outcome
The formulation used in the Liusmed rosacea protocol contains agents that are expensive, concentration-dependent, and compartment-specific. Consider the practical implications:
PRP (Platelet-Rich Plasma)/PLT (Platelet (count)) growth factors are autologous biological products prepared from the patient's own blood. Each milliliter represents a finite resource. Growth factor activity is dose-dependent -- half the dose does not produce half the effect; it may produce negligible effect below a threshold concentration. Losing 20% to surface leakage means the tissue concentration may fall below the therapeutic threshold despite the nominal dose being adequate.
Microbotox must reach neural terminals in the papillary dermis to produce its anti-neurogenic effect. If injected too deep, it diffuses into the reticular dermis and may reach the underlying muscle, causing unwanted facial movement changes. If it leaks to the surface, it is wasted entirely. The margin between effective intradermal delivery and problematic deep diffusion is measured in tenths of millimeters.
Tranexamic acid achieves its anti-angiogenic effect through local concentration at the VEGF (Vascular Endothelial Growth Factor — new blood vessel signal) signaling site. Systemic absorption dilutes TXA to sub-therapeutic concentrations. Every drop that leaks from the target site is a drop that fails to suppress angiogenic signaling where it matters.
The formulation is only as effective as the delivery system that places it. A perfect cocktail delivered imprecisely produces mediocre results. A well-designed formulation delivered with zero-leakage precision into the correct tissue plane produces the outcomes that justify the treatment.
This is why Liusmed Clinic views manual injection not as a nostalgic attachment to traditional technique but as a clinical requirement for therapeutic mesotherapy in rosacea. The Rosacea Injection Treatment protocol was designed around manual delivery because the tissue demands it.
Frequently Asked Questions
Q1: Is manual injection more painful than a meso gun?
Paradoxically, many patients find manual injection less painful. The slow, controlled needle insertion of manual technique causes less acute tissue trauma than the rapid-fire needle strikes of an automated device. Additionally, the operator can pause or adjust if the patient reports discomfort at a specific point. Topical anesthetic cream is applied before all sessions, and the fine-gauge needles used (30-32 gauge) minimize sensation.
Q2: Does manual injection take significantly longer than machine treatment?
Yes. A full-face manual mesotherapy session for rosacea typically takes 30 to 45 minutes, compared to 15 to 20 minutes with an automated device. However, the relevant comparison is not time per session but outcomes per treatment course. If manual injection delivers a higher effective dose to the target tissue per session, fewer total sessions may be required to achieve the same outcome, partially offsetting the time difference.
Q3: How do I know my physician is skilled enough for manual mesotherapy?
This is a legitimate concern. Manual mesotherapy is highly operator-dependent, and results vary significantly with skill level. Indicators of expertise include specialized mesotherapy training (not just basic injection courses), specific experience with rosacea patients (not just cosmetic treatments), willingness to discuss technique in detail, and clinical photography demonstrating consistent outcomes across multiple patients. At Liusmed Clinic, rosacea injection is performed personally by Dr. Liu, who has refined the technique over years of dedicated practice.
Q4: Can a machine with adjustable settings match manual precision?
Current automated devices cannot replicate the continuous, real-time adaptation that manual injection provides. Adjustable settings allow the operator to change parameters between zones, but within a zone, the device delivers identical parameters to every point. Manual injection adjusts within a single pass based on tissue feedback at every insertion point. Future devices with real-time tissue sensing and adaptive depth control may narrow this gap, but as of 2026, no commercially available device offers this capability.
Q5: What happens to the product that leaks out during machine-driven injection?
Leaked product appears on the skin surface as a thin film of fluid after the needle withdraws. It is typically wiped away or absorbed by gauze during the procedure. This product does not contribute to the therapeutic effect. Some practitioners argue that surface product is absorbed transdermally, but the molecules used in rosacea mesotherapy (botulinum toxin, growth factors, tranexamic acid) are too large for meaningful transdermal absorption through intact epidermis.
Q6: If manual injection is superior, why do most clinics use machines?
The primary drivers are economic and logistical. Automated devices allow clinics to treat more patients per hour, require less operator training, and produce more consistent (though less precise) results across a range of skill levels. For cosmetic hydration treatments where precision is less critical, this trade-off is reasonable. For therapeutic applications in pathological skin, the calculation reverses: precision matters more than throughput, and the machine's advantages become liabilities.
About the Author
Dr. Ta-Ju Liu is the founder of Liusmed Clinic, a practice built on the principles of regenerative medicine and minimal incision surgery. Dr. Liu's commitment to manual mesotherapy technique reflects a broader clinical philosophy that prioritizes precision and tissue-level outcomes over procedural speed. His expertise in manual injection for rosacea has been developed through years of dedicated practice, continuous technique refinement, and rigorous outcome documentation.
Disclaimer
This article is provided for educational and informational purposes only and does not constitute medical advice, diagnosis, or treatment. The comparison between manual and automated injection techniques reflects the clinical perspective of Liusmed Clinic and may not represent the views of all practitioners. Individual results depend on disease severity, operator skill, and patient-specific factors. Always consult a qualified healthcare provider before beginning any new treatment.
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

