Why Do Dark Spots Keep Multiplying? How to Distinguish Melasma, Freckles, and Sunspots
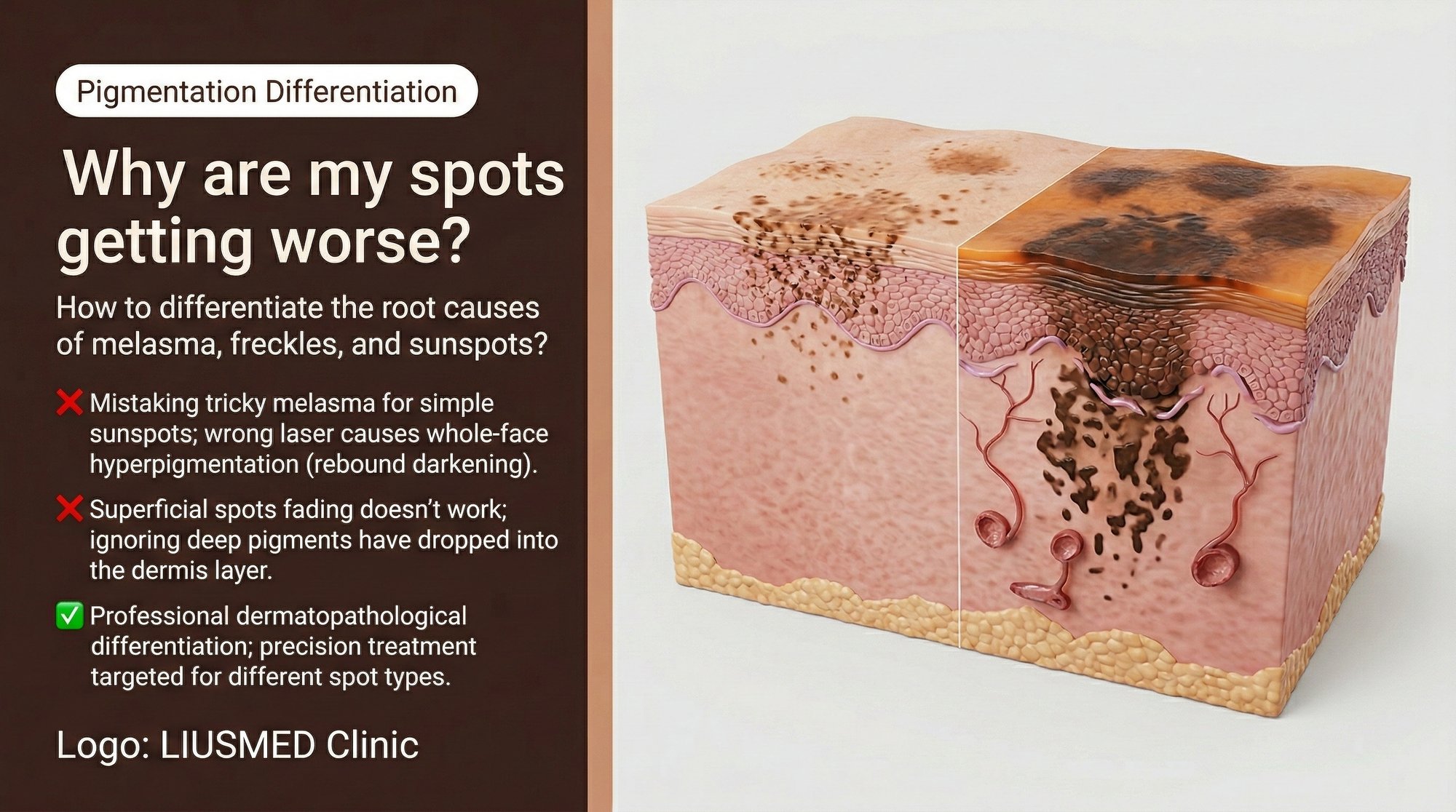
You apply whitening serums religiously, yet new dark patches appear every few weeks. You have tried laser toning, chemical peels, and vitamin C derivatives — none of them seem to stick. Before blaming your skin, consider this: you may be treating the wrong condition entirely. Melasma, freckles, and sunspots look deceptively similar to the untrained eye, but they originate from completely different mechanisms. Treating one as if it were another is the single most common reason pigmentation problems persist — or even worsen.
Table of Contents
- The Biology of Skin Pigmentation
- Melasma: The Hormonal and Vascular Pigment Disorder
- Freckles: Genetic UV Responders
- Sunspots: Cumulative Photodamage
- Side-by-Side Comparison Table
- Why Accurate Diagnosis Changes Everything
The Biology of Skin Pigmentation
Every visible dark spot on your skin is ultimately the result of melanin — a pigment produced by specialized cells called melanocytes that reside at the junction between the epidermis and dermis. Under normal conditions, melanocytes distribute melanin evenly through small packets called melanosomes, which are transferred to surrounding keratinocytes. This process gives skin its baseline colour and offers a degree of UV protection.
Problems arise when melanocytes become hyperactive, when melanin is deposited deeper than it should be, or when inflammatory signals keep the pigment-production cycle permanently switched on. The clinical appearance — whether it looks like a faint brown cloud, a defined dot, or a flat dark patch — provides the first clue about which mechanism is dominant.
Understanding the depth and driver of pigmentation is not academic trivia. Epidermal pigment responds to topical agents and gentle chemical peels. Dermal pigment does not. Hormonally driven pigment recurs unless the hormonal trigger is managed. UV-driven pigment darkens with every unprotected exposure. A treatment plan that ignores these distinctions is simply guesswork.
Melasma: The Hormonal and Vascular Pigment Disorder
Melasma presents as large, symmetrical patches of brown to grey-brown discoloration, most commonly on the cheeks, forehead, upper lip, and bridge of the nose. It is overwhelmingly more common in women, particularly during or after pregnancy, oral contraceptive use, or hormone replacement therapy. However, men are not immune — roughly 10 percent of melasma cases occur in males.
What distinguishes melasma from other pigmentary conditions is its multi-factorial nature. Three drivers operate simultaneously in most patients. First, hormonal fluctuations — particularly elevated estrogen and progesterone — stimulate melanocyte activity directly. Second, UV radiation amplifies the process by triggering inflammatory mediators in the skin. Third, an often-overlooked vascular component exists: dilated blood vessels beneath the pigmented patches supply growth factors and inflammatory signals that sustain melanin overproduction.
This vascular element explains why melasma is so notoriously resistant to treatment. You can lighten the melanin with topical agents, but if the underlying blood vessels continue to feed the melanocytes, repigmentation is almost guaranteed within weeks. Dermatoscopy or Wood lamp examination can reveal the vascular reticular pattern that marks this subtype.
Melasma pigment can sit at three levels: epidermal (brown, well-defined borders), dermal (grey-blue, diffuse borders), or mixed. The deeper the pigment, the less responsive it is to surface treatments. For patients whose melasma has a significant dermal or vascular component, targeted approaches such as Melasma Injection Treatment offer a way to address the root cause rather than just the surface symptom.
Freckles: Genetic UV Responders
Freckles — known medically as ephelides — are small, flat, well-defined spots typically 1 to 5 millimetres in diameter. They are strongly associated with fair skin, red or blonde hair, and the MC1R gene variant. Freckles tend to appear in childhood and darken with sun exposure, often fading significantly during winter months.
The mechanism is straightforward: in individuals with the genetic predisposition, UV exposure triggers a burst of melanin production within existing melanocytes. Importantly, freckles do not involve an increased number of melanocytes — the cells simply produce more pigment per unit of UV stimulation than they would in someone without the genetic variant.
Because the pigment is purely epidermal and UV-responsive, freckles are the most treatable of the three conditions. Strict sun protection alone can cause noticeable fading. Topical retinoids, vitamin C, and azelaic acid can accelerate the process. IPL (intense pulsed light) and Q-switched (Q-switched laser) lasers are highly effective because the pigment sits in a superficial, accessible layer.
The critical clinical point is that freckles do not worsen with hormonal changes and do not have a vascular component. If a patient reports that their spots darkened dramatically during pregnancy or after starting birth control pills, that is melasma behaviour — not freckle behaviour — regardless of how small or scattered the spots appear.
Sunspots: Cumulative Photodamage
Solar lentigines — commonly called sunspots, age spots, or liver spots — are flat, uniformly pigmented macules ranging from a few millimetres to over a centimetre in diameter. They appear on chronically sun-exposed areas: the face, dorsal hands, forearms, upper chest, and shoulders. Unlike freckles, sunspots do not fade in winter. Once established, they are permanent without intervention.
Sunspots represent a structural change in the skin. Years of cumulative UV exposure cause a localized increase in the number of melanocytes and a thickening of the epidermis at the site. The melanocytes in a sunspot are not just overactive — there are genuinely more of them, and they have developed a permanently elevated baseline of melanin output.
This structural permanence is why sunspots do not respond to sun avoidance alone. The extra melanocytes remain in place regardless of UV exposure. Treatment requires physically removing or destroying the excess melanocytes through cryotherapy, laser ablation, or targeted phototherapy. Chemical peels and retinoids can provide modest improvement but rarely achieve complete clearance.
Sunspots are generally benign, but any lesion that is asymmetric, has irregular borders, varies in colour, or changes rapidly should be evaluated to rule out lentigo maligna, a form of melanoma that can mimic a sunspot.
Side-by-Side Comparison Table
| Feature | Melasma | Freckles | Sunspots |
|---|---|---|---|
| Typical size | Large patches (2-10 cm) | Small dots (1-5 mm) | Medium macules (5-20 mm) |
| Shape | Irregular, cloud-like | Round, well-defined | Round to oval, defined borders |
| Distribution | Symmetrical (bilateral) | Scattered, sun-exposed areas | Isolated or clustered |
| Colour | Brown to grey-brown | Tan to light brown | Medium to dark brown |
| Depth | Epidermal, dermal, or mixed | Epidermal only | Epidermal |
| Age of onset | 20s-40s | Childhood | 40s and older |
| Hormonal link | Strong | None | None |
| UV response | Worsens significantly | Darkens seasonally | Stable once formed |
| Winter fading | Minimal | Significant | None |
| Vascular component | Often present | Absent | Absent |
| Topical response | Partial, often temporary | Good | Modest |
| Laser response | Risky — can worsen | Excellent | Good |
| Recurrence after treatment | High without maintenance | Moderate with UV exposure | Low if fully treated |
Why Accurate Diagnosis Changes Everything
The consequences of misdiagnosis are not trivial. Consider the patient who treats melasma with aggressive laser toning intended for sunspots. The thermal energy triggers post-inflammatory hyperpigmentation, and the melasma paradoxically darkens. Or the patient who spends years applying hydroquinone for what they believe is melasma, when the spots are actually solar lentigines that would respond far better to a single session of targeted phototherapy.
Accurate diagnosis requires more than a visual glance. A proper evaluation includes Wood lamp examination to assess pigment depth, dermatoscopy to check for vascular patterns, and a thorough medical history covering hormonal status, medication use, UV exposure habits, and family history of pigmentary conditions.
At Liusmed Clinic, the diagnostic process also considers the vascular microenvironment beneath the pigmented area. If dilated vessels are feeding the melanocytes, no amount of topical lightening will produce lasting results. In such cases, Melasma Injection Treatment targets the vascular and inflammatory drivers simultaneously, addressing the soil rather than just the weed.
The bottom line is simple: if you have been treating dark spots for more than three months without meaningful improvement, the first question to ask is not whether you need a stronger product — it is whether you have the right diagnosis.
Frequently Asked Questions
Q1: Can I have melasma and sunspots at the same time?
Yes. It is entirely possible — and quite common — for a patient to have concurrent melasma and solar lentigines, especially in individuals over 40 with significant sun exposure history. Each condition requires its own treatment strategy. Attempting to treat both with a single modality often leads to suboptimal results for one or both conditions.
Q2: My dark spots appeared after I started birth control pills. Are they freckles?
Almost certainly not. Freckles are genetically determined and typically appear in childhood. Pigmentation that emerges or worsens after starting oral contraceptives is characteristic of melasma. The estrogen and progesterone in hormonal contraceptives are known melasma triggers. Consult a dermatologist to confirm the diagnosis before beginning treatment.
Q3: Will strict sun protection alone clear my melasma?
Sun protection is absolutely essential for melasma management and will prevent worsening, but it rarely clears established melasma completely. This is because hormonal and vascular factors continue to drive melanin production independently of UV exposure. Sun protection should be the foundation of any melasma treatment plan, but most patients will need additional targeted therapy.
Q4: Why did my melasma get worse after laser treatment?
Certain laser modalities — particularly aggressive ablative lasers and some Q-switched lasers — can trigger post-inflammatory hyperpigmentation in melasma-prone skin. The thermal injury creates inflammation, which stimulates melanocytes to produce even more pigment. This is why melasma requires cautious, evidence-based treatment approaches rather than aggressive energy-based devices.
Q5: Are over-the-counter whitening products effective for any of these conditions?
Over-the-counter products containing ingredients like vitamin C, niacinamide, or alpha arbutin can provide modest improvement for epidermal freckles and mild melasma. They are generally insufficient for sunspots (which involve structural melanocyte changes) or dermal melasma (where the pigment is too deep for topical agents to reach effectively).
Q6: How do I know if my melasma has a vascular component?
Vascular melasma often presents with a reticular (net-like) pattern visible under dermatoscopy, and the affected area may show background redness or telangiectasia. If your melasma worsens with heat, alcohol, spicy food, or emotional stress — triggers that dilate blood vessels — a vascular component is likely. A specialized evaluation at a clinic experienced in pigmentary disorders can confirm this through dermoscopic and Wood lamp examination.
About the Author
Dr. Ta-Ju Liu is the founder and lead physician at Liusmed Clinic, specializing in regenerative medicine and minimal incision surgery. With advanced training in ultrasound-guided procedures, vascular assessment, and tissue regeneration, Dr. Liu approaches pigmentary disorders as systemic conditions requiring precise diagnosis and multi-target treatment rather than surface-level cosmetic interventions. Liusmed Clinic integrates diagnostic imaging, vascular evaluation, and targeted injection therapies to address the root causes of treatment-resistant melasma.
Disclaimer
This article is provided for educational and informational purposes only and does not constitute medical advice, diagnosis, or treatment. Individual skin conditions vary significantly, and the information presented here may not apply to your specific situation. Always consult a qualified dermatologist or medical professional before starting any treatment for pigmentary disorders. Results from any treatment mentioned in this article are not guaranteed and may vary from person to person.
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

