Can Rosacea Skin Handle Picosecond Laser? Debunking the "Skin Rejuvenation Laser" Marketing Myth
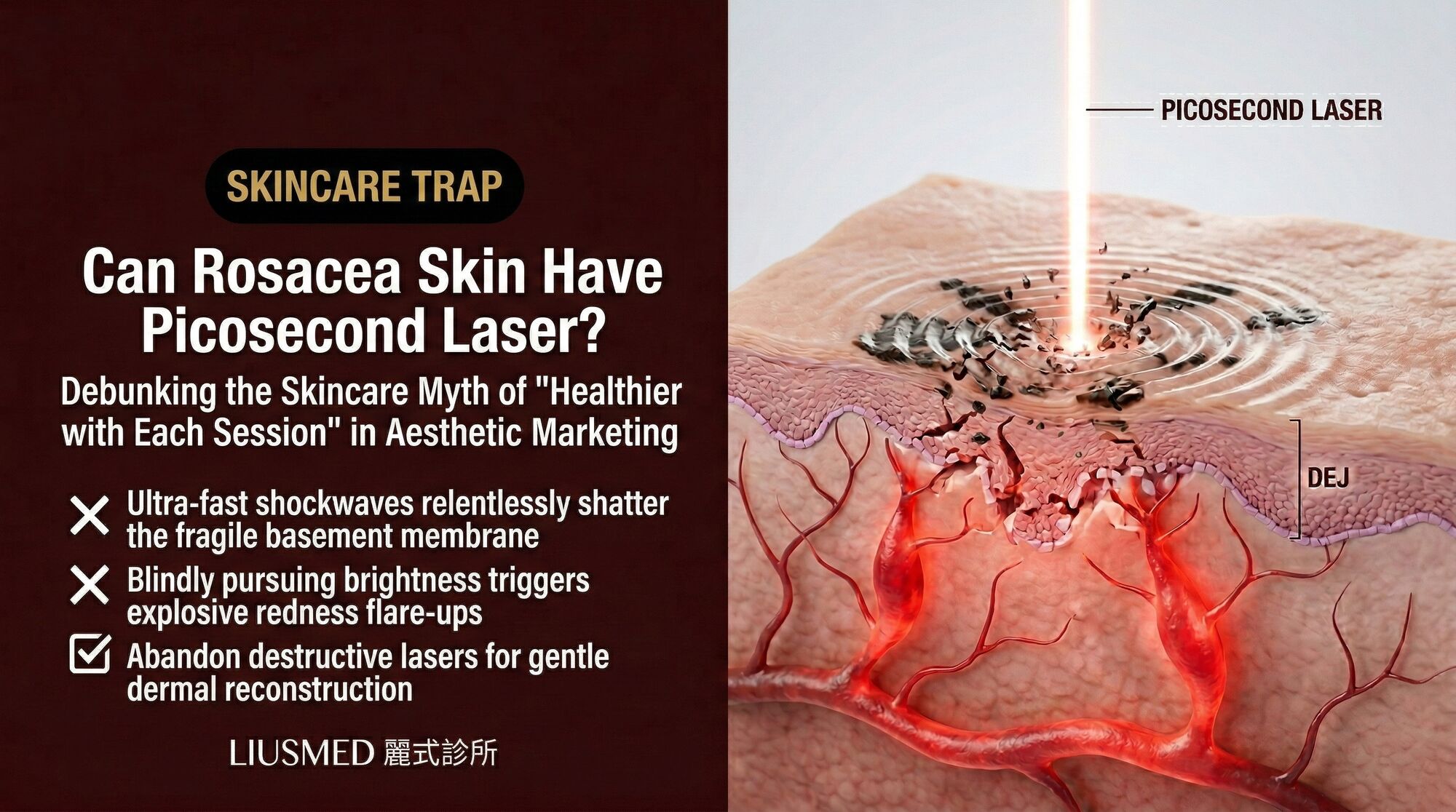
The marketing is convincing. Picosecond lasers are described as "gentle," "non-thermal," and suitable for "all skin types including sensitive skin." Social media is filled with before-and-after photos showing brighter, smoother complexions after picosecond treatments. Your clinic recommended it specifically because your skin is sensitive. It is supposed to be the safe option.
For patients without rosacea, picosecond lasers may indeed be a reasonable cosmetic tool. But rosacea is not simply "sensitive skin." It is a chronic inflammatory disease with a dysregulated immune system, compromised dermal matrix, and hyperreactive vascular network. Applying picosecond laser energy to this environment is not the gentle procedure the marketing implies — and for many rosacea patients, it triggers a cascade of events that makes their condition measurably worse.
Table of Contents
- How Picosecond Lasers Differ from Traditional Lasers
- The Photoacoustic Effect: Not Thermal Does Not Mean Not Damaging
- Why Rosacea Skin Responds Differently to Picosecond Energy
- Marketing Claims vs. Biological Reality: A Comparison
- Clinical Patterns: What Rosacea Patients Report After Picosecond Treatment
- Safer Alternatives for Rosacea Patients Seeking Skin Improvement
How Picosecond Lasers Differ from Traditional Lasers {#how-picosecond-lasers-differ}
To understand why picosecond lasers affect rosacea skin differently than advertised, you need to understand what makes them distinct from older laser technologies.
Traditional Q-switched (Q-switched laser) lasers deliver energy in nanosecond pulses — each pulse lasting between 5 and 20 billionths of a second. Picosecond lasers deliver energy in pulses measured in trillionths of a second — approximately 100 to 1000 times shorter than nanosecond pulses.
This extreme shortening of pulse duration changes the fundamental mechanism of tissue interaction. Nanosecond lasers work primarily through photothermal effects — the target chromophore absorbs light, converts it to heat, and the heat destroys the target. Picosecond lasers work primarily through photomechanical (photoacoustic) effects — the energy is delivered so rapidly that it generates pressure waves within and around the target, physically shattering it rather than heating it.
The marketing advantage is obvious: "We do not burn your tissue; we gently shatter targets with pressure waves. Less heat means less damage, faster recovery, and suitability for sensitive skin."
This narrative is accurate for pigment removal from otherwise healthy skin. Melanosomes (pigment-containing structures) are indeed shattered more efficiently by photoacoustic forces than by heat, and the reduced thermal component does mean less collateral thermal damage to surrounding tissue.
But rosacea skin is not otherwise healthy skin. And the photoacoustic effect — while producing less heat — introduces its own set of biological consequences that are particularly problematic for chronically inflamed tissue.
The Photoacoustic Effect: Not Thermal Does Not Mean Not Damaging {#the-photoacoustic-effect}
When picosecond pulses interact with tissue, the rapid energy deposition creates microscopic cavitation bubbles and pressure waves that propagate through the dermis. In the focused mode (using diffractive or holographic lens arrays), these pressure waves are concentrated to create laser-induced optical breakdown (LIOB) — microscopic vacuoles within the dermis that trigger a wound healing response.
The marketing frames LIOB as a controlled stimulus for collagen remodeling. And in healthy skin with a normal immune response, this is a reasonable description. The microscopic vacuoles heal, new collagen is deposited, and skin texture improves.
In rosacea skin, however, the LIOB response is fundamentally different:
Exaggerated immune recruitment. Each LIOB vacuole triggers an immune response — neutrophil infiltration, macrophage activation, and cytokine release. In normal skin, this response is proportionate and self-limiting. In rosacea skin, where immune cells are already primed and inflammatory pathways are upregulated, the response is amplified. What should be a controlled remodeling stimulus becomes an inflammatory trigger.
Mast cell activation. The mechanical shock waves from photoacoustic energy are potent mast cell degranulation triggers. Mast cells respond to mechanical stimulation through mechanosensitive ion channels, and the rapid pressure changes from picosecond pulses activate these channels efficiently. In rosacea skin with its elevated mast cell density and reduced degranulation threshold, this effect is particularly pronounced.
Cathelicidin cascade. The tissue damage from LIOB activates keratinocytes and triggers upregulation of cathelicidin (LL-37) production. In rosacea skin where kallikrein-5 (KLK5) activity is already elevated, this additional LL-37 production adds fuel to the inflammatory cycle that drives both erythema and angiogenesis.
Neuropeptide release. Photoacoustic shock waves stimulate dermal sensory nerve endings, triggering release of substance P and CGRP (Calcitonin Gene-Related Peptide). These neuropeptides cause vasodilation, increase vascular permeability, and promote further mast cell degranulation — creating a neurogenic inflammation loop.
The net result is that while picosecond laser produces less thermal damage than nanosecond alternatives, it produces significant photomechanical and immunological activation that is often worse for rosacea patients than the thermal damage it avoids.
Why Rosacea Skin Responds Differently to Picosecond Energy {#rosacea-skin-responds-differently}
The fundamental issue is that rosacea is not a cosmetic condition — it is an immunological one. The distinction matters enormously for understanding why a treatment that works well for cosmetic concerns in healthy skin can be counterproductive in rosacea.
Healthy skin has what immunologists call "immune homeostasis" — a balanced state where immune surveillance is active but inflammatory responses are tightly regulated. When a controlled injury like LIOB occurs, the immune response ramps up proportionately, does its work, and returns to baseline.
Rosacea skin lacks this homeostatic balance. The immune system is in a state of chronic low-grade activation, with elevated baseline levels of inflammatory cytokines (IL-1beta, TNF-alpha, IL-6), upregulated innate immune pathways (TLR2, cathelicidin), and impaired regulatory mechanisms that would normally resolve inflammation.
When picosecond laser creates LIOB vacuoles in this pre-inflamed environment, the immune response does not follow the controlled trajectory seen in healthy skin. Instead:
- The inflammatory ramp-up is faster and more intense than expected
- The peak inflammatory response is higher, with greater neutrophil infiltration and cytokine release
- The resolution phase is prolonged or incomplete, leaving the tissue more inflamed than before treatment
- The angiogenic signals generated during wound healing are amplified by the pre-existing pro-angiogenic environment
This pattern — exaggerated inflammation with impaired resolution — is the hallmark of rosacea's response to virtually any controlled tissue injury, whether thermal, mechanical, or photoacoustic. The mechanism of injury matters less than the immunological context in which it occurs.
Marketing Claims vs. Biological Reality: A Comparison {#marketing-vs-reality}
| Marketing Claim | Biological Reality in Rosacea Skin |
|---|---|
| "Non-thermal, so safe for sensitive skin" | Photoacoustic forces trigger mast cell degranulation and neuropeptide release independent of heat |
| "Stimulates natural collagen remodeling" | LIOB creates wound-healing response that is dysregulated in rosacea, often producing more inflammation than remodeling |
| "Suitable for all skin types" | Rosacea is not a skin type — it is a chronic inflammatory disease with fundamentally different immune responses |
| "Minimal downtime" | Initial appearance may be acceptable, but delayed inflammatory flares at 48–96 hours are common in rosacea patients |
| "Improves skin texture and tone" | May temporarily improve surface texture while simultaneously worsening underlying dermal inflammation |
| "Less aggressive than traditional lasers" | Less thermal aggression, but photomechanical and immunological aggression can be equally or more problematic |
| "Progressive improvement with multiple sessions" | Rosacea patients often show progressive worsening with cumulative immune activation across sessions |
| "Backed by clinical studies" | Studies typically exclude rosacea patients or fail to differentiate rosacea from general skin sensitivity |
The gap between marketing narrative and biological reality is not because picosecond laser manufacturers are being dishonest. Most claims are accurate for their intended population — cosmetic patients with healthy skin seeking improvement in pigmentation, fine lines, or overall skin quality. The problem is the extrapolation of these claims to rosacea patients, for whom the underlying biology produces fundamentally different outcomes.
Clinical Patterns: What Rosacea Patients Report After Picosecond Treatment {#clinical-patterns}
Based on clinical observation of rosacea patients who have undergone picosecond laser treatment, several consistent patterns emerge:
The delayed flare. Unlike thermal laser reactions that peak within 24 hours, picosecond-triggered rosacea flares often appear 48 to 96 hours post-treatment. This delay corresponds to the timeline of adaptive immune recruitment and cathelicidin upregulation. The delay can make it difficult for patients to connect the flare to the treatment, and practitioners may attribute it to external triggers.
The papulopustular eruption. Some rosacea patients develop papules and pustules in the treated area within one to two weeks of picosecond treatment, even if their baseline rosacea was primarily erythematotelangiectatic (redness-dominant). The LIOB-triggered immune response can shift the disease phenotype from vascular to inflammatory, representing a genuine worsening of the condition.
The sensitivity escalation. Products and environmental exposures that were tolerated before treatment become intolerable afterward. This reflects both barrier disruption from the treatment itself and upregulated neurogenic inflammation from photoacoustic stimulation of nerve endings.
The "it helped at first" trajectory. Perhaps the most confusing pattern for patients: the first one or two picosecond sessions may produce genuine improvement, likely from mild collagen stimulation and pigment clearance. This early success leads to continued treatment, but sessions three through six progressively worsen the rosacea as cumulative immune activation overwhelms the cosmetic benefits.
Safer Alternatives for Rosacea Patients Seeking Skin Improvement {#safer-alternatives}
Rosacea patients who want to improve skin quality — texture, tone, luminosity — are not wrong to want these things. The challenge is finding approaches that achieve cosmetic improvement without triggering or amplifying the underlying inflammatory disease.
Barrier-first approach. Before any aesthetic intervention, the skin barrier should be optimized. A competent stratum corneum reduces transepidermal water loss, decreases sensitivity, and provides a more stable foundation for any subsequent treatment. This alone often produces noticeable improvement in skin quality.
Low-concentration topical retinoids. Carefully titrated retinoids (starting at very low concentrations with gradual increase) can improve skin texture and promote healthy collagen remodeling without the immune activation of laser-based approaches. The key is extremely slow introduction and careful monitoring for flare activity.
Anti-inflammatory microenvironment treatment. Approaches like Rosacea Injection Treatment address the underlying dermal inflammation that both drives rosacea and makes aesthetic treatments risky. By calming the immune microenvironment first, subsequent cosmetic improvements become both safer and more effective.
LED photobiomodulation at specific wavelengths. Low-level light therapy at anti-inflammatory wavelengths (particularly 830 nm near-infrared) at low fluences can support mitochondrial function and reduce inflammation without the photoacoustic or photothermal effects of higher-powered devices. The evidence is more limited than for laser, but the risk profile is substantially more favorable for rosacea.
Time and patience. This is the least marketable but most honest recommendation. Rosacea skin that has been subjected to repeated inflammatory stimuli — whether from lasers, harsh products, or environmental triggers — needs time to recover. Sometimes the most impactful cosmetic intervention is six months of doing nothing beyond gentle barrier support.
The desire for better-looking skin is legitimate and understandable. But for rosacea patients, the path to better-looking skin runs through disease control, not around it. Any cosmetic treatment applied to uncontrolled rosacea — no matter how "gentle" the marketing claims — risks making the disease worse and the skin more difficult to manage.
Frequently Asked Questions
Q1: My dermatologist specifically recommended picosecond laser for my rosacea. Are they wrong?
Not necessarily wrong, but potentially working with incomplete information. Picosecond laser training and marketing materials focus heavily on its reduced thermal profile compared to traditional lasers, which is accurate. What is less emphasized in training is the photoacoustic and immunological activation profile, particularly in chronically inflamed tissue. If your dermatologist is open to discussion, sharing your concerns about immune activation in rosacea may lead to a more nuanced treatment plan.
Q2: I had one picosecond session and my skin seems fine. Should I continue?
Proceed with caution. A single session without adverse effects is not a reliable predictor of long-term tolerance. The cumulative immune activation pattern means that sessions two through four carry progressively higher risk. If you choose to continue, extend the interval between sessions to at least eight weeks, monitor carefully for the delayed flare pattern (48–96 hours post-treatment), and have a clear stopping criterion defined in advance.
Q3: What about the picosecond "toning" mode at very low fluence? Is that safe for rosacea?
Low-fluence toning reduces both thermal and photoacoustic effects, which does improve the safety profile. However, reduced does not mean eliminated. Even sub-threshold fluences produce some degree of mast cell activation and neuropeptide release in highly sensitive tissue. For patients with well-controlled, stable rosacea, cautious toning may be tolerable. For patients with active or reactive rosacea, even toning mode carries meaningful risk.
Q4: The clinic showed me before-and-after photos of rosacea patients treated with picosecond laser. Were those fake?
Likely not fake, but potentially unrepresentative. Several factors can make before-and-after photos misleading: short follow-up periods that capture the initial improvement but not the delayed worsening; selection of patients who happened to respond well (publication bias); differences in lighting, camera settings, or skin preparation between before and after photos; and inclusion of patients with facial redness from other causes (not true rosacea) who respond differently.
Q5: If picosecond laser is risky for rosacea, why do so many clinics offer it for this condition?
The combination of effective marketing, genuine efficacy in non-rosacea populations, high patient demand for "gentle laser" options, and the commercial appeal of treating a large patient population creates strong incentives to offer picosecond for rosacea. Additionally, many aesthetic practitioners do not have specialized training in rosacea immunology, so the nuances of immune activation in chronically inflamed tissue may not be part of their clinical framework.
Q6: How long should I wait after a bad picosecond laser experience before trying a different treatment approach?
A minimum of three months is advisable, with six months being more appropriate if you experienced significant flaring or sensitivity escalation. During this recovery period, focus exclusively on barrier repair and anti-inflammatory support. Do not introduce any new active ingredients or device treatments. The goal is to allow the immune activation triggered by the picosecond treatment to fully resolve before introducing any new intervention.
About the Author
Dr. Ta-Ju Liu is the founder of Liusmed Clinic, a practice dedicated to regenerative medicine and minimal incision surgery. Having treated hundreds of rosacea patients who experienced worsening after various laser protocols, Dr. Liu advocates for an immunology-first approach to rosacea management. Liusmed Clinic prioritizes understanding each patient's inflammatory status before recommending any energy-based or interventional treatment, ensuring that therapeutic decisions are guided by disease biology rather than device availability.
Disclaimer
This article is provided for educational and informational purposes only and does not constitute medical advice, diagnosis, or treatment. Picosecond laser technology is an established medical device with legitimate clinical applications. This article specifically addresses its application in the context of rosacea, a chronic inflammatory condition with unique biological characteristics. Individual responses to treatment vary. All treatment decisions should be made in consultation with a qualified healthcare provider.
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

