Can Picosecond Laser Truly Cure Melasma? Why It Always Comes Back After You Stop
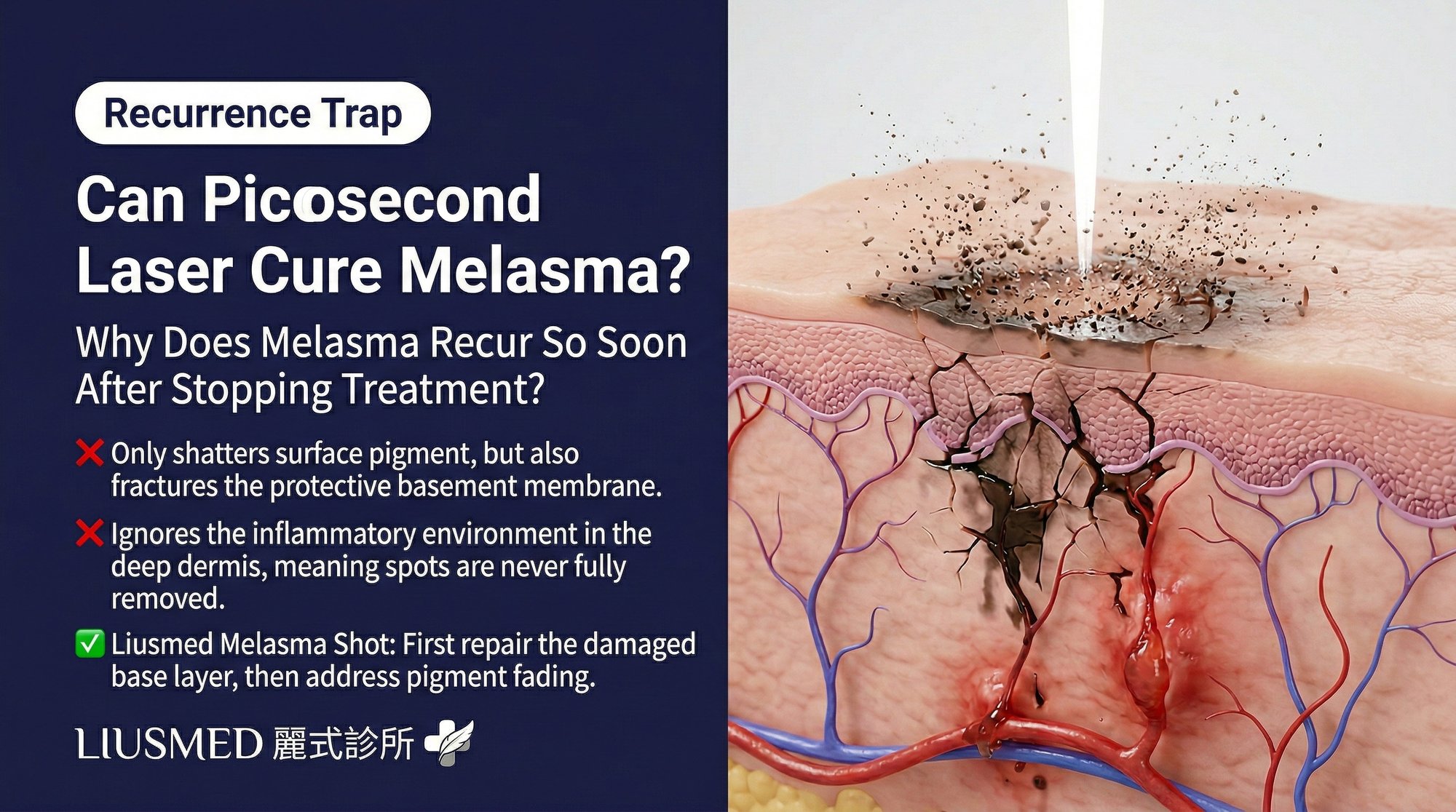
The marketing pitch is compelling. Picosecond laser, firing at trillionths of a second, shatters pigment into particles so fine that your body can sweep them away effortlessly. Clinics display dramatic before-and-after photographs. Social media influencers share their glowing skin post-treatment. The technology sounds like the logical endpoint of laser evolution: faster pulses, less heat, better results.
So you invest. Three sessions. Five sessions. Maybe eight. And it works, or at least it appears to. Your melasma fades, your skin tone evens out, and you feel genuinely hopeful for the first time in years.
Then you stop. Three months later, the patches creep back. Six months later, they are fully reestablished. Sometimes they are even worse than before.
This is not a failure of willpower or sun protection. It is a fundamental limitation of using any energy-based device to treat a condition that is not, at its core, a pigment-excess problem.
Table of Contents
- The Picosecond Advantage: What It Actually Does Well
- Why Melasma Is Not a Pigment Problem
- The Recurrence Paradox: Clearing Pigment Without Fixing the Source
- Clinical Evidence: What the Studies Actually Show
- Picosecond Laser vs. Melasma Injection Therapy: A Comparison
- Moving Beyond the Laser Cycle
The Picosecond Advantage: What It Actually Does Well
Credit where credit is due: picosecond lasers represent a genuine technological advancement. By delivering energy in pulse durations measured in picoseconds (10^-12 seconds) rather than the nanoseconds (10^-9 seconds) of Q-switched (Q-switched laser) lasers, they achieve a predominantly photomechanical rather than photothermal effect on pigment particles.
This means they can fragment melanin into smaller particles with less collateral thermal damage to surrounding tissue. For conditions like solar lentigines (sun spots), post-inflammatory hyperpigmentation from acne, and certain types of birthmarks, picosecond lasers offer a meaningful improvement over older technology. Fewer sessions, faster recovery, and more complete clearance.
The problem arises when this technology is applied to melasma, which superficially resembles these other pigmentary conditions but is fundamentally different in its pathophysiology.
Why Melasma Is Not a Pigment Problem
This is the most important concept that patients and even some clinicians fail to grasp: melasma is not primarily a disease of excess pigment. It is a disease of dysfunctional skin microenvironment.
Research over the past decade has revealed that melasma lesions differ from surrounding normal skin in numerous ways that go far beyond melanin content. The affected areas show increased dermal vascularity, with more blood vessels and higher expression of vascular endothelial growth factor (VEGF). They demonstrate a disrupted basement membrane zone, the structural boundary between the epidermis and dermis that normally helps regulate melanocyte behavior. They contain elevated levels of inflammatory mediators, including mast cells, prostaglandins, and various cytokines. They show solar elastosis and collagen degradation in the dermis, suggesting chronic photodamage at the structural level.
Melanocytes in melasma skin are not simply overproducing pigment for no reason. They are responding rationally to a pathological environment that is constantly sending them activation signals. The excess pigment is a symptom, not the disease.
When a picosecond laser shatters and clears that excess pigment, it is performing the equivalent of mopping up water on the floor while the pipe above continues to leak. The floor looks clean temporarily, but the underlying problem guarantees that the water, or in this case the pigment, will return.
The Recurrence Paradox: Clearing Pigment Without Fixing the Source
The recurrence pattern after picosecond laser treatment for melasma follows a remarkably consistent timeline. Most patients see significant improvement during their treatment course and for one to three months afterward. Then, gradually at first and then more rapidly, the pigment returns.
This happens because the laser addresses none of the underlying drivers of melasma. The abnormal vasculature remains. The disrupted basement membrane remains. The chronic inflammatory signaling remains. The hormonal sensitivity of the affected melanocytes remains. The solar elastosis remains.
Every one of these factors continues to bombard melanocytes with activation signals, and since the melanocytes themselves were not destroyed (nor should they be, as that leads to depigmentation), they resume their hyperactive pigment production within weeks to months.
There is also evidence that the process of laser-mediated pigment clearance itself may reinforce some of these pathological signals. The phagocytic activity required to clear laser-fragmented melanin involves macrophage recruitment and local inflammatory signaling, which can paradoxically contribute to the very microenvironment that drives melasma.
Some patients describe a pattern of diminishing returns with repeated picosecond courses. The first round of treatment produces dramatic improvement. The second round, initiated after recurrence, produces moderate improvement. By the third or fourth round, the laser seems barely effective, and the intervals between recurrences grow shorter. This pattern suggests that each cycle may be making the underlying microenvironment progressively more resistant to superficial pigment clearance.
Clinical Evidence: What the Studies Actually Show
When you look beyond marketing materials and examine the peer-reviewed literature, the evidence for picosecond laser as a standalone melasma treatment is sobering.
Published studies consistently show that while picosecond laser can achieve short-term improvement in melasma severity scores (as measured by MASI or mMASI), the durability of results is poor. Follow-up periods beyond six months reveal recurrence rates exceeding sixty to seventy percent in most published cohorts. Some studies report near-complete return of pigment at twelve months post-treatment.
Critically, the studies that show the best outcomes typically involve combination approaches where picosecond laser is paired with topical therapy, oral medications, or other interventions. When you control for the contribution of these adjunctive treatments, the independent contribution of the laser itself becomes much less impressive.
There are also important questions about publication bias. Studies with positive results are far more likely to be published than those showing no benefit or harm. The true recurrence rate in routine clinical practice, outside the controlled conditions of a research study, may be even higher than the literature suggests.
None of this means that picosecond laser is a bad technology. It means that it is being applied to a condition for which it is not well-suited as a standalone treatment, and patients deserve to understand this before investing significant money and time.
Picosecond Laser vs. Melasma Injection Therapy: A Comparison
| Factor | Picosecond Laser | Melasma Injection Therapy |
|---|---|---|
| Primary Target | Melanin granules (symptom) | Inflammatory microenvironment (cause) |
| Mechanism | Photomechanical fragmentation of pigment | Direct delivery of anti-inflammatory and melanogenesis-modulating agents |
| Vascular Component | Not addressed; may worsen with repeated treatments | Directly targeted with vascular-normalizing agents |
| Basement Membrane | Not addressed; potential for collateral damage | Supports structural repair and barrier restoration |
| Recurrence Rate | High (60-70%+ within 12 months of stopping) | Lower when underlying microenvironment is successfully modulated |
| Maintenance Requirement | Ongoing sessions needed to maintain results | Reduced maintenance once microenvironment stabilizes |
| Skin Sensitivity | May increase with repeated sessions | Generally preserves or improves skin resilience |
| Cost Over Time | High due to repeated courses needed | Potentially lower due to reduced recurrence |
| Suitability for Darker Skin | Higher risk of PIH and depigmentation | Lower risk profile across skin types |
The philosophical difference is stark. Picosecond laser asks "how do we remove this pigment?" while Melasma Injection Treatment asks "why is this pigment being produced, and how do we change those conditions?" For a chronic condition like melasma, the second question is the one that leads to lasting answers.
Moving Beyond the Laser Cycle
If you are caught in the cycle of picosecond treatments followed by recurrence, recognizing the pattern is the first and most important step. The cycle persists because the treatment model is fundamentally mismatched to the disease.
Breaking free requires a shift in perspective. Instead of viewing melasma as pigment that needs to be removed, start viewing it as a signal that your skin's microenvironment in those specific areas is dysfunctional. Effective treatment must address that dysfunction.
Reassess your treatment goals. Complete permanent elimination of melasma may not be realistic for every patient, regardless of treatment approach. However, significant long-term reduction with minimal maintenance is achievable when the underlying drivers are addressed. Setting realistic expectations is not defeatist; it is the foundation for making good treatment decisions.
Evaluate your hormonal landscape. Hormonal influences, including oral contraceptives, hormone replacement therapy, pregnancy, and even thyroid dysfunction, are among the most potent drivers of melasma. No topical, injectable, or laser treatment can fully overcome active hormonal stimulation. If hormonal factors are present, they should be addressed as part of any comprehensive treatment plan.
Prioritize sun protection as treatment, not just prevention. For melasma patients, sunscreen is not a preventive measure; it is an active treatment. UV radiation is the most consistent and powerful trigger for melanocyte activation in melasma. Without rigorous daily sun protection including broad-spectrum SPF (Sun Protection Factor) 50+ and physical barriers, no treatment of any kind will produce lasting results.
Consider a multimodal approach. The most successful melasma management protocols combine strategies that target different aspects of the disease. This might include Melasma Injection Treatment to address the local microenvironment, topical agents to suppress surface melanogenesis, oral supplements to reduce systemic inflammation, and lifestyle modifications to minimize triggers.
Be patient with the timeline. Melasma developed over months or years. Expecting it to resolve permanently in a few weeks is unrealistic regardless of the treatment used. Meaningful, stable improvement typically requires three to six months of consistent therapy, with ongoing maintenance strategies to prevent recurrence.
Frequently Asked Questions
Q1: If picosecond laser keeps my melasma away while I am doing treatments, can I just keep doing maintenance sessions indefinitely?
While some clinics do offer indefinite maintenance protocols, this approach has several concerns. Repeated laser exposure carries cumulative risks including epidermal thinning, melanocyte destruction leading to mottled depigmentation, increased skin sensitivity, and potential PIH (Post-Inflammatory Hyperpigmentation) rebound. The cost also accumulates substantially over years. A more sustainable strategy addresses the underlying cause so that ongoing laser suppression becomes unnecessary.
Q2: I was told that the newer picosecond lasers with holographic fractional tips are different and can actually treat the dermal component. Is this true?
Fractional picosecond handpieces create laser-induced optical breakdown (LIOB) cavitation zones in the dermis, which can stimulate collagen remodeling. While this may address some of the dermal changes associated with melasma, clinical evidence specifically for melasma remains limited and recurrence is still common. The technology is promising for skin rejuvenation broadly but has not been proven to resolve the complex microenvironment abnormalities that drive melasma.
Q3: My dermatologist recommends combining picosecond with topical tranexamic acid. Is that a better approach?
Combination approaches generally outperform monotherapy for melasma. Topical tranexamic acid has anti-inflammatory and anti-angiogenic properties that may help address some of the microenvironment dysfunction. However, even in combination studies, long-term recurrence remains a significant issue. The key question is whether the laser component is adding enough benefit to justify its risks and costs, or whether the topical/systemic treatments are doing most of the heavy lifting.
Q4: How long should I wait after stopping picosecond before trying a different approach?
A minimum washout period of three months is generally recommended. This allows any subclinical inflammation from the laser treatments to resolve and gives your melanocytes time to return to a less reactive baseline state. During this period, strict sun protection and gentle skincare are essential. Some patients may need longer, particularly if they experienced any signs of PIH or skin sensitization.
Q5: Is there any type of melasma that does respond well to picosecond laser long-term?
Epidermal-predominant melasma in patients with lighter skin types (Fitzpatrick I-II) tends to respond best to laser-based treatments. However, even in this subgroup, true long-term remission without maintenance treatment is uncommon. Mixed and dermal-predominant melasma, which accounts for the majority of cases in Asian and darker-skinned patients, has consistently poor long-term outcomes with laser monotherapy.
Q6: What makes the injection approach different in terms of preventing recurrence?
The Melasma Injection Treatment approach targets the dysfunctional microenvironment that causes melanocytes to overproduce pigment. By delivering anti-inflammatory agents, vascular normalizers, and basement membrane support directly to the affected tissue, it addresses the root causes rather than just the visible symptom. When the signaling environment around melanocytes normalizes, the drive to overproduce pigment diminishes, leading to more stable results with less dependence on ongoing treatment.
About the Author
Dr. Ta-Ju Liu is the founder of Liusmed Clinic, a specialized center for regenerative medicine and minimal incision surgery in Taiwan. With extensive experience in treating patients who have experienced recurrent melasma despite multiple courses of laser therapy, Dr. Liu has developed comprehensive protocols that address the underlying microenvironment dysfunction driving persistent pigmentation. His approach integrates dermatological science with regenerative medicine principles to achieve lasting improvement.
Disclaimer
This article is provided for educational and informational purposes only and does not constitute medical advice. Individual skin conditions vary significantly, and treatment outcomes depend on numerous patient-specific factors. Always consult a qualified dermatologist or medical professional before making decisions about melasma treatment. The information presented here reflects current medical understanding as of the publication date and may be updated as new research becomes available.
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

