How High-Concentration PRP Repairs the Damaged Basement Membrane: Evidence-Based Melasma Ecological Restoration
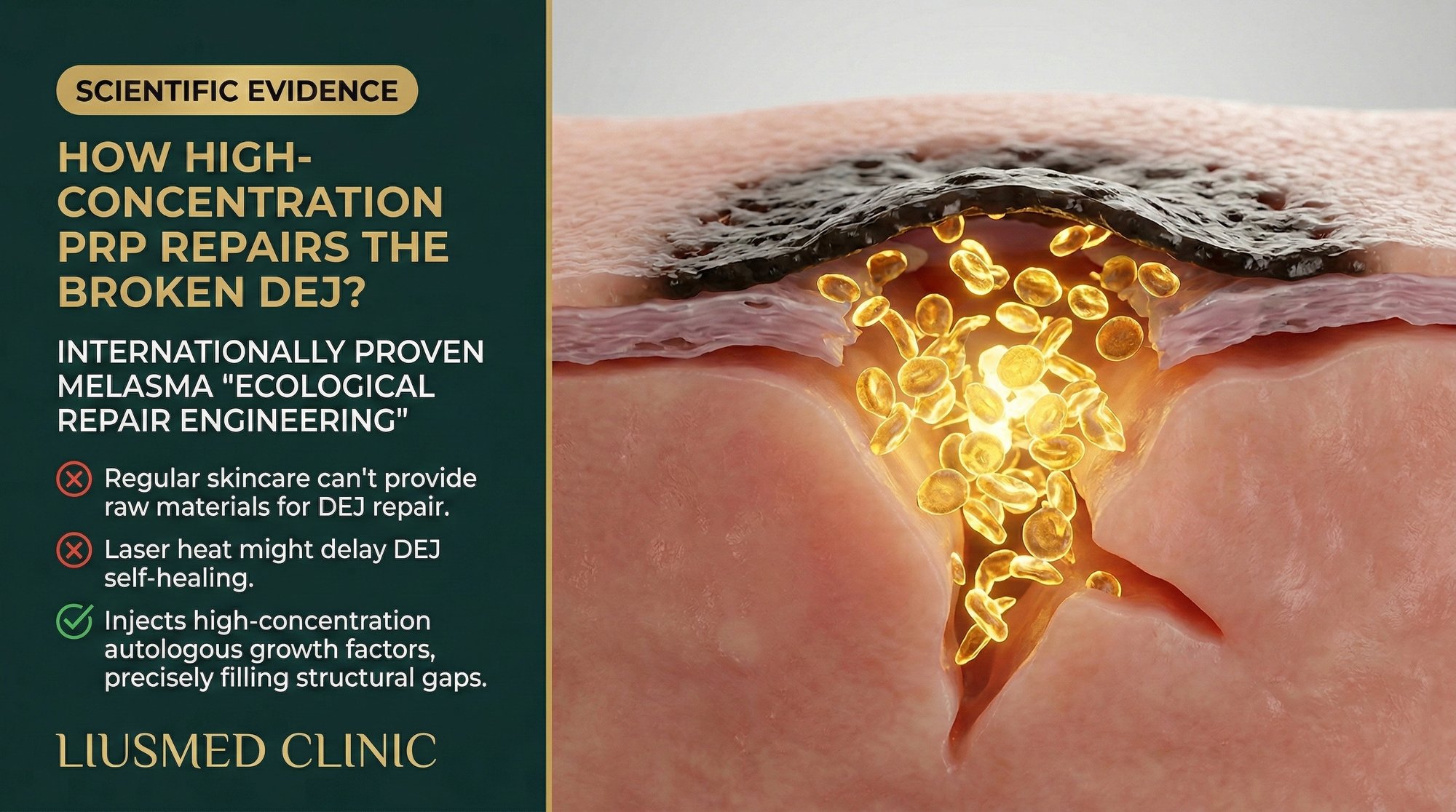
When melanin escapes through a broken basement membrane and drops into the dermis, no laser and no cream can retrieve it efficiently. The only lasting solution is to rebuild the barrier that should have kept it in place. High-concentration PRP (Platelet-Rich Plasma — concentrate of your own blood platelets rich in growth factors) offers the biological toolkit to do exactly that.
Table of Contents
- The Basement Membrane: The Forgotten Structure in Melasma Treatment
- How Basement Membrane Damage Drives Refractory Melasma
- PRP Composition and the Growth Factor Cascade
- Mechanism of PRP-Driven Basement Membrane Repair
- High-Concentration vs. Standard PRP: Why Dosage Changes Everything
- Clinical Evidence and Histological Observations
The Basement Membrane: The Forgotten Structure in Melasma Treatment
The basement membrane zone (BMZ) is a thin but critically important structure that sits between the epidermis and the dermis. Composed primarily of type IV collagen, laminin, nidogen, and heparan sulfate proteoglycans, this extracellular matrix serves as both a structural scaffold and a biological filter.
In healthy skin, the BMZ performs several essential functions. It anchors the epidermis to the dermis through a complex network of hemidesmosomes and anchoring fibrils. It regulates the passage of molecules and cells between the two layers. And it acts as a physical barrier that keeps epidermal components — including melanin — from migrating into the dermis.
Despite its importance, the BMZ has been almost entirely ignored in conventional melasma treatment paradigms. The focus has remained on either destroying melanin (lasers, chemical peels) or inhibiting melanin production (topical hydroquinone, arbutin, kojic acid). Neither approach addresses the structural failure that allows melanin to become permanently trapped in the dermis.
This oversight is particularly significant because histological studies of melasma skin have consistently demonstrated BMZ abnormalities. Electron microscopy reveals gaps in the lamina densa, disrupted anchoring fibrils, and reduced type IV collagen density in melasma lesions compared to adjacent normal skin.
How Basement Membrane Damage Drives Refractory Melasma
The relationship between BMZ damage and treatment-resistant melasma can be understood through a simple analogy: the BMZ is like a dam, and melanin is the water behind it. When the dam is intact, water stays where it belongs. When the dam develops cracks, water seeps through to the other side.
In melasma, chronic ultraviolet exposure, hormonal fluctuations, and persistent inflammation gradually degrade the BMZ. As gaps form in this barrier, melanin granules and melanin-containing cell fragments pass from the epidermis into the upper dermis. Once in the dermis, melanin is phagocytosed by dermal macrophages (melanophages), creating deposits that are essentially permanent without intervention.
This is the mechanism behind what clinicians call "dermal melasma" — the deep, blue-gray pigmentation that fails to respond to topical treatments and often worsens with aggressive laser therapy. The pigment is not being actively produced in the dermis; rather, it has fallen through a broken barrier and become trapped.
The implications for treatment are profound. Even if surface melanin production is successfully reduced through topical agents, new melanin will continue to leak through the damaged BMZ with every melanogenic stimulus. This explains the frustrating pattern of partial improvement followed by relapse that defines the melasma treatment experience for millions of patients worldwide.
| BMZ Component | Normal Function | Status in Melasma | Consequence of Damage |
|---|---|---|---|
| Type IV collagen | Structural scaffold of lamina densa | Reduced density, focal gaps | Loss of barrier integrity |
| Laminin-332 | Anchors epidermis to dermis | Disrupted distribution | Weakened epidermal attachment |
| Anchoring fibrils (type VII collagen) | Connects BMZ to dermal matrix | Decreased and disorganized | Reduced structural support |
| Heparan sulfate proteoglycans | Molecular filtration | Depleted | Loss of selective permeability |
| Hemidesmosomes | Mechanical attachment | Reduced number | Epidermal-dermal separation |
PRP Composition and the Growth Factor Cascade
Platelet-rich plasma is a concentrated preparation of platelets suspended in a small volume of plasma, obtained by centrifuging the patient's own blood. The therapeutic power of PRP lies not in the platelets themselves but in the bioactive molecules stored within platelet alpha-granules.
Upon activation, each platelet releases over 300 bioactive proteins. The key growth factors relevant to BMZ repair include:
Platelet-derived growth factor (PDGF) stimulates fibroblast proliferation and migration. Fibroblasts are the primary cells responsible for producing extracellular matrix components in the dermis, including the type IV collagen that forms the structural backbone of the BMZ.
Transforming growth factor-beta (TGF-beta) is a master regulator of extracellular matrix synthesis. It directly upregulates the expression of type IV collagen, laminin, and fibronectin — all critical BMZ components. TGF-beta also modulates the inflammatory response, shifting the tissue microenvironment from chronic inflammation toward constructive remodeling.
Epidermal growth factor (EGF) promotes epithelial cell proliferation and differentiation, supporting the re-establishment of normal epidermal architecture above the repaired BMZ.
Vascular endothelial growth factor (VEGF) at physiological concentrations supports the maintenance of normal microvasculature. While pathological overexpression of VEGF (Vascular Endothelial Growth Factor — new blood vessel signal) drives the abnormal angiogenesis seen in melasma, the controlled release from PRP helps normalize rather than exacerbate vascular function.
Insulin-like growth factor-1 (IGF-1) works synergistically with PDGF (Platelet-Derived Growth Factor — platelet-released cell growth signal) and TGF-beta to amplify the fibroblast response and promote matrix synthesis.
The combined action of these growth factors creates a coordinated regenerative response that no single pharmaceutical agent can replicate.
Mechanism of PRP-Driven Basement Membrane Repair
When high-concentration PRP is delivered directly to the dermo-epidermal junction via manual mesotherapy, it initiates a multi-step repair cascade:
Phase 1: Inflammatory modulation (Days 1-3). The anti-inflammatory cytokines in PRP, including hepatocyte growth factor (HGF) and lipoxin A4, begin suppressing the chronic inflammatory signals that drive ongoing BMZ degradation. Matrix metalloproteinases (MMPs) — the enzymes responsible for breaking down collagen — are downregulated. Simultaneously, tissue inhibitors of metalloproteinases (TIMPs) are upregulated, shifting the balance from matrix destruction to matrix preservation.
Phase 2: Fibroblast recruitment and activation (Days 3-7). PDGF and TGF-beta attract fibroblasts to the treatment zone and stimulate their proliferation. These activated fibroblasts begin synthesizing new extracellular matrix components, including type IV collagen precursors (procollagen IV chains) that will assemble into the lamina densa of a restored BMZ.
Phase 3: Matrix assembly and remodeling (Weeks 2-6). The newly synthesized collagen and other matrix proteins are organized into functional structures. Type IV collagen molecules self-assemble into the characteristic sheet-like network of the lamina densa. Laminin molecules integrate into the matrix, re-establishing the anchoring connections between epidermis and dermis.
Phase 4: Barrier maturation (Weeks 6-12). The repaired BMZ matures and strengthens through continued cross-linking and integration of additional matrix components. As barrier integrity is restored, the passage of melanin into the dermis is progressively blocked.
This timeline explains why patients undergoing the Melasma Injection Treatment see gradual, progressive improvement over multiple sessions rather than dramatic overnight changes. The protocol is rebuilding tissue architecture — a process that requires time and biological cooperation.
High-Concentration vs. Standard PRP: Why Dosage Changes Everything
A critical but often overlooked variable in PRP therapy is platelet concentration. Not all PRP preparations are equivalent, and the difference between standard and high-concentration PRP can determine clinical success or failure.
Standard PRP preparation methods typically yield a platelet concentration of 2 to 3 times the baseline blood level. While this represents a meaningful increase in growth factor availability, research suggests that optimal tissue regeneration requires higher concentrations.
Studies on PRP and collagen synthesis have demonstrated a dose-dependent relationship: higher platelet concentrations produce proportionally greater growth factor release and more robust fibroblast stimulation, up to a therapeutic ceiling. Below this ceiling, increasing concentration directly improves outcomes.
The Liusmed protocol utilizes preparation techniques that achieve substantially higher-than-standard platelet concentrations. This is particularly important for BMZ repair because the dermo-epidermal junction is a relatively thin structure that requires intense, localized growth factor signaling to initiate meaningful repair.
| PRP Parameter | Standard Preparation | High-Concentration (Liusmed Protocol) |
|---|---|---|
| Platelet concentration | 2-3x baseline | Significantly above standard |
| Growth factor release | Moderate | Substantially higher |
| Fibroblast stimulation | Mild to moderate | Robust |
| Type IV collagen synthesis | Detectable increase | Clinically meaningful increase |
| BMZ repair potential | Limited | Therapeutically relevant |
| Treatment sessions needed | More sessions for comparable effect | Fewer sessions for target outcome |
Clinical Evidence and Histological Observations
The evidence supporting PRP's role in basement membrane repair comes from multiple convergent lines of research.
In wound healing studies, PRP has been shown to accelerate re-epithelialization and restore BMZ architecture in both acute and chronic wounds. Histological analysis of PRP-treated wounds demonstrates earlier and more complete restoration of the lamina densa compared to untreated controls.
In dermatological research, studies examining PRP for skin rejuvenation have documented increased type IV collagen deposition at the dermo-epidermal junction, improved anchoring fibril density, and enhanced overall BMZ integrity on histological examination.
Clinical observations from patients treated with the Melasma Injection Treatment are consistent with these findings. Serial dermoscopic imaging shows progressive reduction in the blue-gray dermal pigment component, which correlates with improved BMZ barrier function preventing further pigment migration into the dermis.
Patients who have undergone previous unsuccessful laser treatments often show the most dramatic responses to the PRP-based protocol. This likely reflects the fact that their melasma was driven primarily by BMZ failure and dermal pigment trapping — mechanisms that lasers cannot address but that PRP-driven regeneration targets directly.
The ecological restoration metaphor is apt: rather than trying to remove pollution from a river (destroying pigment), the Liusmed approach repairs the dam (BMZ) that was allowing contamination in the first place. Once the barrier is restored and the inflammatory environment is normalized, the skin's own clearance mechanisms can gradually process the existing dermal pigment.
Frequently Asked Questions
Q1: What exactly is the basement membrane, and why does it matter for melasma?
The basement membrane is a thin layer of specialized proteins (primarily type IV collagen and laminin) that sits between the outer skin layer (epidermis) and the deeper layer (dermis). It acts as a physical barrier. When it is damaged — as is consistently seen in melasma — melanin pigment can leak from the epidermis into the dermis, creating deep, stubborn discoloration that resists conventional surface treatments.
Q2: Can topical products repair the basement membrane?
Topical products face a fundamental delivery challenge: they cannot penetrate deeply enough to reach the dermo-epidermal junction in therapeutically meaningful concentrations. Some topical ingredients (such as retinoids) can indirectly support collagen synthesis, but the concentrations and the precision needed for BMZ repair require direct intradermal delivery — which is why the Liusmed protocol uses manual injection to place PRP exactly at the target depth.
Q3: How is PRP prepared for this treatment?
A small volume of the patient's blood is drawn and processed using centrifugation to separate and concentrate the platelets. The Liusmed protocol uses specific preparation parameters optimized for high platelet yield and growth factor concentration. The entire preparation is performed in-clinic under sterile conditions, and the PRP is used immediately to ensure maximum bioactivity.
Q4: Are there any risks of using PRP for melasma treatment?
Because PRP is derived from the patient's own blood, the risk of allergic reaction or immune rejection is essentially zero. The primary risks are those associated with any injection procedure: temporary redness, minor bruising, and pinpoint injection marks. These typically resolve within 24 to 48 hours. There is no risk of the post-inflammatory hyperpigmentation that makes laser treatment problematic for melasma patients.
Q5: How many sessions are needed to see basement membrane repair?
Tissue regeneration is a gradual biological process. Most patients begin to see clinical improvement (reduced pigmentation depth and intensity) after 2 to 3 sessions. Meaningful BMZ repair, as reflected by sustained pigment reduction and resistance to rebound, typically requires 4 to 6 sessions. The exact timeline varies based on individual healing capacity, melasma severity, and adherence to the post-treatment protocol.
Q6: Can this treatment be combined with other melasma therapies?
The PRP-based BMZ repair protocol can be complemented by appropriate topical agents (such as broad-spectrum sunscreen, gentle antioxidants, and barrier-supporting moisturizers) to protect the healing tissue and support the regenerative process. However, aggressive treatments such as chemical peels, high-energy lasers, or strong retinoids should be avoided during the active treatment phase, as they can counteract the repair process by inducing additional inflammation.
About the Author
Dr. Ta-Ju Liu is the founder of Liusmed Clinic and a specialist in regenerative medicine and minimal incision surgery. His clinical work focuses on applying evidence-based regenerative principles — including advanced PRP therapy and manual mesotherapy techniques — to conditions that conventional dermatological treatments fail to resolve. Liusmed Clinic is committed to treating the root pathology of skin conditions rather than managing surface symptoms.
Disclaimer
This article is provided for educational and informational purposes only. It does not constitute medical advice, diagnosis, or treatment. Individual results vary based on numerous factors including the severity and duration of the condition, individual healing capacity, and adherence to treatment protocols. Consult a qualified healthcare professional before making any decisions regarding medical treatment. The information presented reflects clinical experience and published research as of the date of publication.
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

