Soolantra (Ivermectin) Die-Off Breakout: How Long Does the Purging Phase Last?
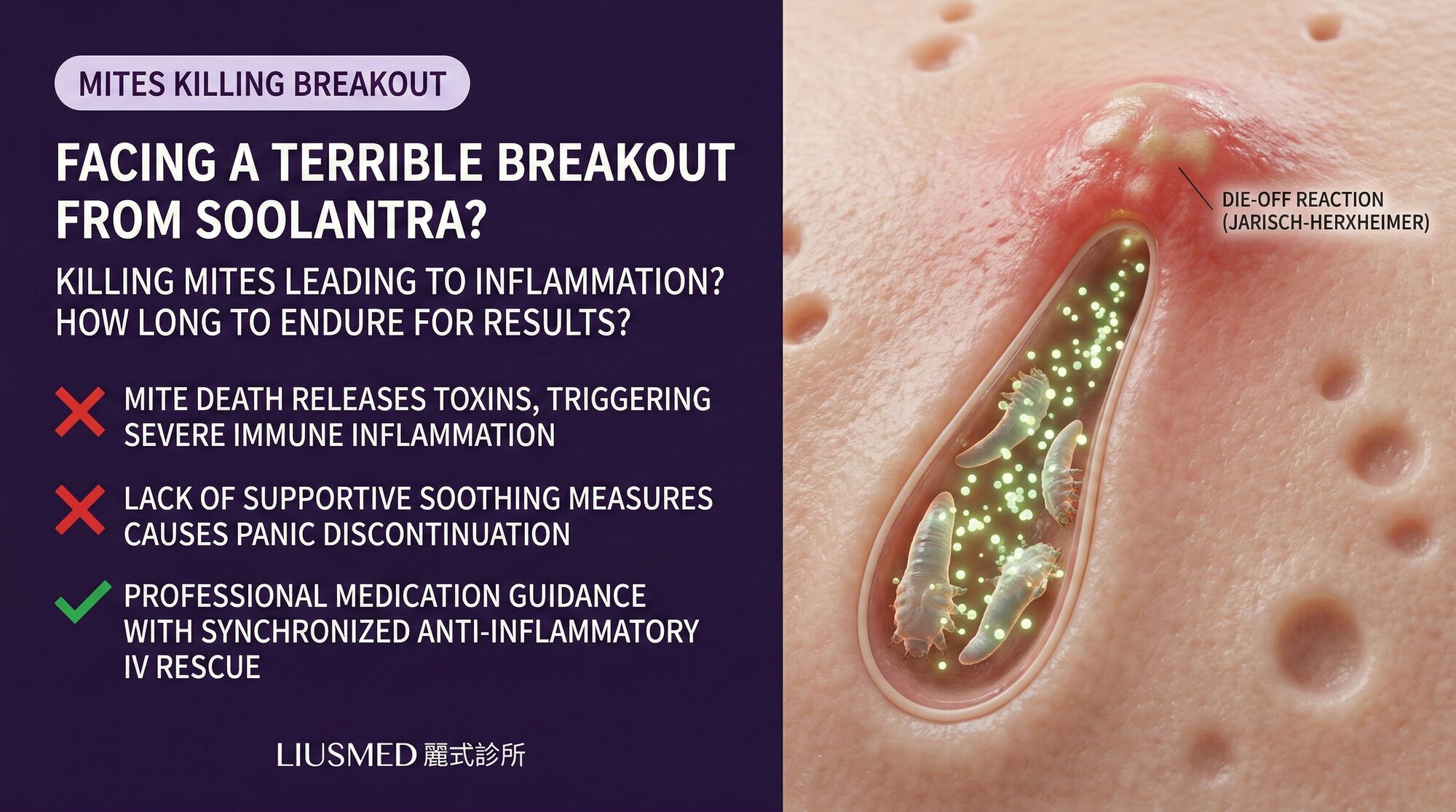
You filled the prescription with cautious optimism. Your dermatologist explained that Soolantra (ivermectin 1% cream) targets the Demodex mites living in your follicles and contributing to your rosacea inflammation. What nobody adequately prepared you for was week two, when your face erupted in more papules and pustules than you had before treatment. Your instinct screams to stop. But that breakout may actually be the clearest sign the medication is working.
Table of Contents
- Why Soolantra Causes an Initial Breakout
- The Demodex Connection in Rosacea
- Die-Off Reaction vs. Treatment Failure: How to Tell the Difference
- The Soolantra Purging Timeline Week by Week
- Managing Symptoms During the Die-Off Phase
- Beyond Soolantra: When Topical Therapy Is Not Enough
Why Soolantra Causes an Initial Breakout
The initial worsening experienced by many Soolantra users is a phenomenon analogous to the Jarisch-Herxheimer reaction observed in infectious disease treatment. When ivermectin kills Demodex mites within the hair follicles and sebaceous glands, the dying organisms release their internal contents, including bacteria they carry (particularly Bacillus oleronius), partially digested sebum, and waste products, directly into the surrounding dermal tissue.
This sudden release of antigenic material triggers a localized immune response. Neutrophils and macrophages rush to the sites of mite death, producing the inflammatory papules and pustules that characterize the die-off breakout. The reaction is not an allergic response to ivermectin itself but rather the immune system's response to the debris of organisms it has been coexisting with, often for years.
The intensity of the die-off reaction tends to correlate with Demodex density. Patients with higher mite loads, common in papulopustular rosacea subtypes, typically experience more pronounced initial worsening. Conversely, patients with primarily erythematotelangiectatic rosacea (subtype I) where Demodex plays a lesser role may notice minimal or no purging.
Understanding this mechanism is essential because premature discontinuation of treatment during the die-off phase is one of the most common reasons patients fail to benefit from ivermectin therapy. The breakout represents a necessary transitional phase, not a contraindication to continued use.
The Demodex Connection in Rosacea
Demodex folliculorum and Demodex brevis are microscopic mites that inhabit human hair follicles and sebaceous glands. They are present on virtually all adult human skin, but their density is markedly elevated in rosacea patients, particularly in the centrofacial region where sebaceous glands are most concentrated.
The relationship between Demodex and rosacea extends beyond simple parasitism. These mites serve as vectors for Bacillus oleronius, a bacterium that produces proteins capable of stimulating inflammatory responses through Toll-like receptor 2 (TLR2) activation. TLR2 overexpression is a well-characterized feature of rosacea pathophysiology.
Additionally, Demodex mites physically damage the follicular epithelium as they feed and reproduce. Their life cycle of approximately 14 to 16 days means that successive generations progressively erode the integrity of the pilosebaceous unit, creating a chronic low-grade inflammatory stimulus. When they die naturally, they lack sphincter muscles and therefore release their entire gut contents, including bacteria, into the follicle.
The density threshold at which Demodex transitions from commensal organism to pathogenic contributor is generally considered to be above five mites per square centimeter when measured by standardized skin surface biopsy. Many rosacea patients exceed this threshold by a factor of ten or more.
| Factor | Low Demodex Density | High Demodex Density |
|---|---|---|
| Typical mite count | < 5 per cm² | > 50 per cm² |
| Predominant rosacea subtype | Erythematotelangiectatic | Papulopustular |
| Expected die-off severity | Mild or absent | Moderate to severe |
| Die-off duration | 1-2 weeks | 3-6 weeks |
| Treatment response timeline | 4-6 weeks | 8-16 weeks |
| Likelihood of needing adjunctive therapy | Lower | Higher |
Die-Off Reaction vs. Treatment Failure: How to Tell the Difference
One of the most anxiety-provoking aspects of the Soolantra experience is uncertainty about whether the worsening represents expected die-off or genuine treatment failure. Several clinical features help distinguish these scenarios.
Timing. Die-off reactions typically begin between days 7 and 21 of treatment, corresponding to the first full Demodex life cycle after ivermectin exposure. Worsening that begins within the first 48 hours is more likely to represent irritant contact dermatitis from the cream vehicle. Worsening that first appears after six to eight weeks of use suggests treatment failure or a diagnosis other than Demodex-driven rosacea.
Lesion Character. Die-off papules and pustules tend to be small, superficial, and concentrated in areas where Demodex density is highest (nasolabial folds, cheeks, forehead, chin). They often appear in clusters corresponding to follicular distribution. In contrast, treatment failure typically manifests as persistence of pre-existing lesions without new cluster formation, or worsening of diffuse erythema without papulopustular component.
Background Erythema. During a genuine die-off reaction, the background redness may actually begin to improve even as new papules appear. This paradoxical pattern, where the inflammatory component improves while the infectious component produces a temporary flare, is a strong indicator that the medication is working.
Symptom Trajectory. Die-off reactions have a characteristic arc: initial worsening, peak intensity around weeks two to three, followed by progressive improvement. If the breakout continues to worsen linearly beyond week four without any plateau or improvement, reassessment is warranted.
Response to Continued Use. Perhaps the most definitive test is the response to persistence. Patients experiencing true die-off who continue treatment typically see clear improvement by weeks six to eight. This requires trust in the process, ideally supported by photographic documentation to objectively track changes that may be difficult to perceive day-to-day.
The Soolantra Purging Timeline Week by Week
While individual variation exists, the following timeline represents a common trajectory for patients experiencing a moderate die-off reaction.
Weeks 1-2: Calm Before the Storm. Many patients notice modest improvement during the first week as ivermectin's anti-inflammatory properties reduce existing erythema. This creates a false sense that treatment will be straightforward, making the subsequent breakout more psychologically jarring.
Weeks 2-3: Peak Purge. New papules and pustules emerge, often in areas that were previously clear. Patients frequently describe this as the worst their skin has ever looked. Stinging, burning, and increased sensitivity to temperature changes are common accompanying symptoms. This phase is when most premature discontinuations occur.
Weeks 3-4: Plateau. The rate of new lesion formation slows. Existing papules begin to flatten and resolve. The overall severity stabilizes, though the skin still appears significantly affected. Continued patience is critical during this phase.
Weeks 4-8: Progressive Clearing. Gradual but measurable improvement becomes evident. Papules resolve faster than they form. Background erythema diminishes. Skin texture begins to smooth. Patients who document their progress with weekly photographs can typically identify clear improvement by comparing week-four images to week-eight images.
Weeks 8-16: Consolidation. Continued use further reduces Demodex populations and allows the follicular epithelium to heal. Many patients achieve their best response in this window. Treatment guidelines generally recommend a minimum of 12 to 16 weeks before assessing overall efficacy.
Beyond Week 16: Maintenance. For patients who respond well, ongoing use at reduced frequency (every other day or two to three times weekly) may be recommended to prevent Demodex recolonization.
Managing Symptoms During the Die-Off Phase
Several strategies can reduce discomfort during the purging period without compromising treatment efficacy.
Gentle Cleansing. A non-foaming, fragrance-free cleanser used with lukewarm water removes excess sebum and surface debris without stripping the compromised barrier. Avoid scrubbing, exfoliating, or using cleansing devices during the die-off phase.
Barrier Support. A ceramide-based moisturizer applied 15 to 20 minutes after Soolantra helps counteract the drying effect of the cream base and supports barrier integrity during the period of increased transepidermal water loss.
Anti-Inflammatory Adjuncts. If burning and stinging are severe, discuss the addition of azelaic acid 15% (applied at a separate time of day from ivermectin) with your treating physician. Azelaic acid addresses inflammation through a different mechanism and can complement ivermectin's antiparasitic action.
Thermal Management. Cool (not cold) compresses applied briefly to flaring areas can provide immediate symptomatic relief by causing transient vasoconstriction. Avoid hot water, steam, and saunas during the purging phase.
Sun Protection. Mineral-based sunscreen with zinc oxide provides broad-spectrum protection while also offering mild anti-inflammatory benefit. The compromised barrier during die-off makes UV-induced flaring more likely.
Psychological Support. The die-off phase is genuinely distressing. Having realistic expectations, support from a knowledgeable clinician, and photographic documentation of baseline and progress can prevent the discouragement that leads to premature treatment abandonment.
Beyond Soolantra: When Topical Therapy Is Not Enough
Ivermectin is effective for many patients with Demodex-driven papulopustular rosacea, but it has limitations. It primarily addresses the parasitic component without correcting the underlying neurovascular dysregulation, innate immune overactivation, or barrier dysfunction that characterize rosacea as a systemic condition.
Patients who complete a full 16-week course with minimal improvement, or who experience recurrent flares despite maintenance therapy, may benefit from a more comprehensive treatment approach. The neurovascular component of rosacea, involving abnormal TRPV1 (Transient Receptor Potential channels) channel activation, calcitonin gene-related peptide (CGRP) release, and impaired vasoregulation, requires interventions that go beyond antiparasitic treatment.
Rosacea Injection Treatment protocols that target the deeper inflammatory and vascular mechanisms can address treatment-resistant cases where topical ivermectin has reached its therapeutic ceiling. These approaches work at the level of the dermal vasculature and neural pathways that drive persistent flushing, erythema, and trigger hypersensitivity.
For patients whose die-off reaction was severe enough to suggest very high Demodex density, combining ivermectin with a targeted in-clinic treatment approach may accelerate recovery and reduce the total duration of the purging phase. This combined strategy addresses both the parasitic trigger and the tissue environment that allowed excessive Demodex proliferation in the first place.
Frequently Asked Questions
Q1: Can I use makeup to cover the die-off breakout?
Yes, but choose mineral-based, non-comedogenic formulations and apply them over your moisturizer. Avoid silicone-heavy primers and heavy liquid foundations that can occlude follicles. Remove makeup thoroughly at the end of each day using a gentle micellar water or oil-based cleanser followed by a mild wash. The goal is to minimize additional follicular occlusion during the period when mite debris is being cleared from the pilosebaceous units.
Q2: Should I use Soolantra more frequently to speed up the die-off?
No. Applying ivermectin more than once daily does not accelerate mite clearance and increases the risk of irritant dermatitis, which compounds the die-off inflammation. The recommended once-daily application provides sufficient drug concentration within the pilosebaceous unit. Increasing frequency increases side effects without improving efficacy.
Q3: Is it safe to take oral ivermectin simultaneously with Soolantra?
Some dermatologists do prescribe a single oral dose of ivermectin (200 micrograms per kilogram) alongside topical treatment for cases with very high Demodex density. However, this should only be done under direct medical supervision. The combined approach can intensify the die-off reaction significantly, and the decision requires weighing the severity of the infestation against the patient's ability to tolerate an amplified purging phase.
Q4: I had a die-off reaction, improved, then worsened again at week 10. What happened?
This pattern can occur because Demodex eggs (which are not killed by ivermectin) hatch approximately two weeks after being laid, producing a new generation of mites. A second, usually milder die-off wave around weeks 8 to 12 reflects ivermectin eliminating this second generation. This is actually a positive sign indicating ongoing parasitic clearance and typically resolves more quickly than the initial purge.
Q5: My Soolantra breakout left post-inflammatory marks. Will they fade?
Post-inflammatory erythema (pink or red marks) and post-inflammatory hyperpigmentation (brown marks) from die-off papules typically fade over two to six months. Consistent sun protection is the single most important factor in preventing these marks from persisting. Azelaic acid, niacinamide, and vitamin C can support the fading process. Avoid aggressive treatments like chemical peels or intense laser during active rosacea management.
Q6: Can I use Soolantra if I have steroid-dependent rosacea?
Yes, and ivermectin is actually an excellent option during steroid withdrawal because it provides anti-inflammatory benefit through a non-steroidal mechanism while also addressing the elevated Demodex populations that often accompany steroid-damaged skin (steroid-induced local immunosuppression allows mite proliferation). However, be aware that the die-off reaction may be more intense due to the higher mite burden, and the compromised barrier from steroid damage makes the skin more reactive overall.
About the Author
Dr. Ta-Ju Liu is the founder of Liusmed Clinic, specializing in regenerative medicine and minimal incision surgery. His clinical practice encompasses the full spectrum of rosacea management, from initial pharmacologic therapy through advanced interventional treatment for refractory cases. Dr. Liu emphasizes patient education and realistic timeline expectations as essential components of successful rosacea treatment.
Disclaimer
This article is provided for educational and informational purposes only and does not constitute medical advice, diagnosis, or treatment. The information presented should not be used to self-diagnose or modify prescribed medication regimens. Soolantra (ivermectin 1% cream) is a prescription medication that should be used under the supervision of a qualified healthcare professional. Always consult your physician before starting, stopping, or changing any treatment.
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

