Steroid-Thinned Skin That Won't Heal? The Steroid-Dependent Rosacea Crisis Nobody Talks About
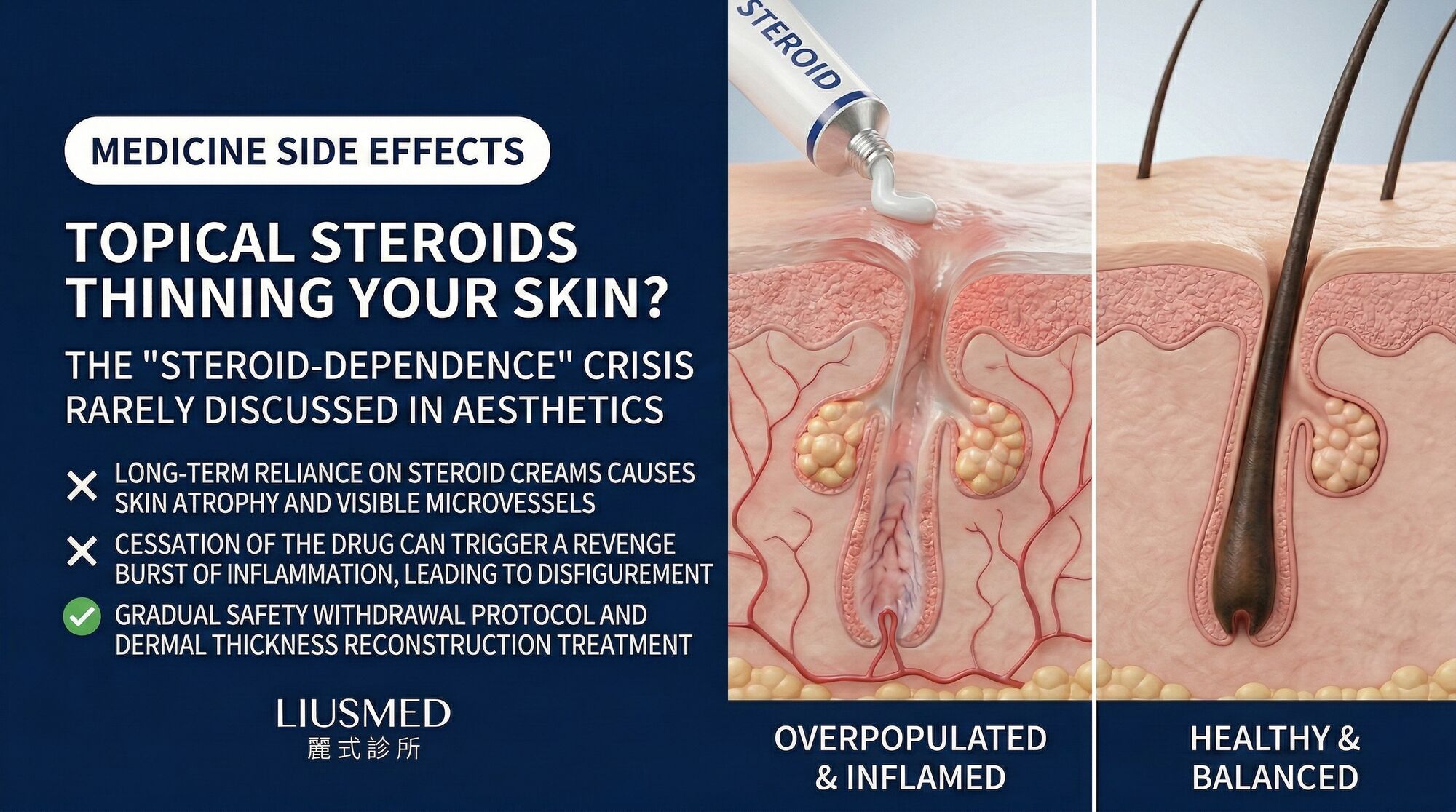
You were told to apply a thin layer twice daily. Within days the redness vanished, the burning stopped, and your skin looked calm for the first time in months. Then you tried to stop. Within 48 hours the redness came roaring back, fiercer than before, and the only thing that quieted it was another application. That is the steroid-dependent rosacea trap, and millions of patients worldwide are caught in it without understanding why.
Table of Contents
- How Topical Steroids Create Dependency in Rosacea Skin
- Recognizing Steroid-Dependent Rosacea vs. Primary Rosacea
- The Biology of Rebound Flares and Skin Thinning
- Withdrawal Timelines and What to Expect
- Evidence-Based Recovery Strategies
- When to Seek Specialist Intervention
How Topical Steroids Create Dependency in Rosacea Skin
Topical corticosteroids suppress inflammation by inhibiting phospholipase A2 and reducing the release of arachidonic acid metabolites. In conditions like eczema or contact dermatitis, this mechanism provides genuine therapeutic benefit when used for short, defined courses. Rosacea skin, however, operates under a fundamentally different inflammatory paradigm centered on innate immune dysfunction and neurovascular dysregulation.
When steroids are applied to rosacea-affected skin, the initial anti-inflammatory effect masks symptoms without addressing the underlying cathelicidin overexpression or abnormal TLR2 signaling. Simultaneously, the steroid begins to suppress local cortisol production through a negative feedback mechanism. Epidermal turnover slows, the stratum corneum thins, and dermal collagen synthesis declines. Within as few as two weeks of daily application of a mid-potency steroid, measurable changes in transepidermal water loss (TEWL) can be detected.
The dependency cycle establishes itself through three overlapping mechanisms. First, tachyphylaxis develops as steroid receptors downregulate, requiring higher potency or more frequent application for the same effect. Second, vasoconstriction from the steroid suppresses visible redness, but the underlying vascular dilation worsens as nitric oxide regulatory pathways are disrupted. Third, the impaired barrier function makes the skin increasingly reactive to environmental triggers that previously caused only mild irritation.
Patients often describe a pattern of escalation: beginning with a low-potency hydrocortisone, progressing to betamethasone or clobetasol as lower-strength formulations lose efficacy, and eventually applying potent steroids around the eyes and nose where the skin is thinnest and most vulnerable.
Recognizing Steroid-Dependent Rosacea vs. Primary Rosacea
Distinguishing steroid-dependent rosacea from untreated primary rosacea is critical because the treatment approaches differ substantially. The following comparison highlights key differentiating features.
| Feature | Primary Rosacea | Steroid-Dependent Rosacea |
|---|---|---|
| Onset pattern | Gradual, triggered by known factors | Rapid worsening upon steroid cessation |
| Skin texture | Normal to slightly rough | Thin, shiny, sometimes atrophic |
| Redness distribution | Centrofacial, follows vascular pattern | Extends to application area, sharp borders |
| Telangiectasia | Moderate, develops over years | Prominent, develops rapidly |
| Burning sensation | Intermittent, trigger-linked | Constant during withdrawal |
| Papules and pustules | Present in subtype II | May appear with perioral distribution |
| Response to gentle skincare | Gradual improvement | Initially worsens before improving |
| Skin thickness on dermoscopy | Normal to mildly thickened | Visibly thinned, vessels easily visible |
A clinical history revealing prolonged topical steroid use, even intermittent use over many months, combined with the pattern of symptom rebound within 24 to 72 hours of discontinuation, is the strongest diagnostic indicator. Many patients have been prescribed steroids for what was initially diagnosed as eczema, seborrheic dermatitis, or nonspecific facial redness, only to develop iatrogenic rosacea as a consequence.
The Biology of Rebound Flares and Skin Thinning
When a topical steroid is abruptly discontinued, the suppressed inflammatory pathways reactivate in an exaggerated fashion. This rebound phenomenon occurs because the skin has adapted to exogenous anti-inflammatory input and has downregulated its own regulatory mechanisms.
At the molecular level, the withdrawal triggers a surge in pro-inflammatory cytokines including interleukin-1, tumor necrosis factor-alpha, and interleukin-8. Mast cells that were stabilized by the steroid degranulate, releasing histamine and tryptase into tissue that is now thinner and more permeable. The resulting erythema, edema, and burning can be dramatically more intense than the original rosacea symptoms.
Skin thinning from chronic steroid use follows a dose-dependent and duration-dependent curve. The epidermis loses rete ridges, reducing the mechanical interlock between epidermis and dermis. Dermal collagen fibers fragment, and the ground substance loses glycosaminoglycans that normally retain moisture. Blood vessel walls weaken, contributing to easy bruising and persistent telangiectasia that may not fully resolve even after steroid cessation.
The perioral and periocular regions are disproportionately affected because the skin in these areas is inherently thinner, has a higher density of steroid receptors, and is subject to frequent mechanical stress from facial expressions and eating.
Withdrawal Timelines and What to Expect
Steroid withdrawal is not a linear process. Patients should anticipate several distinct phases, though individual variation is substantial.
Phase 1 (Days 1 to 14): Acute Rebound. This is typically the most distressing period. Intense erythema, burning, stinging, and edema are common. Skin may feel tight and appear swollen. Sleep disruption from discomfort is frequently reported. Many patients relapse during this phase by resuming steroid use.
Phase 2 (Weeks 2 to 6): Fluctuation. The acute intensity moderates but symptoms wax and wane unpredictably. Desquamation (flaking and peeling) often becomes prominent as the epidermis attempts to regenerate. Papules and pustules may appear, particularly in the perioral region.
Phase 3 (Months 2 to 6): Gradual Stabilization. Flare frequency and intensity progressively decrease. Skin texture begins to normalize, though it often remains more reactive than healthy skin. Telangiectasia established during the steroid-use period may persist.
Phase 4 (Months 6 to 18): Barrier Restoration. With appropriate supportive care, measurable improvements in TEWL and stratum corneum integrity become evident. However, patients who used potent steroids for years may experience prolonged recovery extending beyond 12 months.
A gradual tapering approach, rather than abrupt cessation, is often recommended for patients who have used potent steroids daily for more than three months. This can be achieved by progressively reducing application frequency, switching to a lower-potency steroid, or both.
Evidence-Based Recovery Strategies
Recovery from steroid-dependent rosacea requires a multi-pronged approach focused on barrier repair, inflammation management, and trigger avoidance.
Barrier Repair. The foundation of recovery is restoring the stratum corneum. Ceramide-dominant moisturizers that mimic the natural lipid ratio of the skin barrier (ceramides, cholesterol, and free fatty acids in approximately a 3:1:1 ratio) have demonstrated efficacy in clinical studies. These should be applied liberally and frequently, particularly during the acute withdrawal phase.
Anti-Inflammatory Support Without Steroids. Several non-steroidal agents have shown benefit. Azelaic acid at 15 percent concentration addresses both inflammation and papulopustular lesions through inhibition of reactive oxygen species and abnormal keratinization. Calcineurin inhibitors such as tacrolimus or pimecrolimus can bridge the transition off steroids, though their use should be time-limited and monitored. Niacinamide (vitamin B3) at concentrations of 4 to 5 percent reduces TEWL and supports ceramide synthesis.
Trigger Management. During recovery, the skin's threshold for irritation is dramatically lower than normal. Patients should minimize exposure to temperature extremes, wind, alcohol-containing skincare products, fragrance, and known dietary triggers. Mineral-based sunscreens with zinc oxide are generally better tolerated than chemical sunscreen filters during this period.
Regenerative Approaches. For patients with significant dermal thinning, Rosacea Injection Treatment protocols that target the neurovascular component of rosacea while supporting tissue regeneration can accelerate recovery beyond what topical therapy alone achieves. These approaches address the deeper structural damage that topical barrier repair cannot reach.
When to Seek Specialist Intervention
Self-managed withdrawal is appropriate for patients with short-duration, low-potency steroid use. However, specialist intervention becomes important in several scenarios.
Patients who have used potent (class I or II) steroids on the face for more than six months require supervised tapering. Those experiencing severe psychological distress from withdrawal symptoms benefit from a structured treatment plan with realistic timeline expectations. Cases where periocular skin thinning raises concerns about ocular complications warrant ophthalmologic co-management.
When standard withdrawal support fails to produce improvement after three to four months, or when rebound flares remain severe despite compliant barrier repair protocols, advanced interventions should be considered. The combination of persistent neurovascular dysfunction and structural barrier compromise may require targeted treatments that go beyond what conventional topical therapy can address.
Patients traveling from overseas for treatment should review the Rosacea Injection Treatment protocol details to understand what a comprehensive evaluation involves and how treatment planning accommodates recovery timelines.
Frequently Asked Questions
Q1: Can I use hydrocortisone 1% safely on rosacea for short periods?
Even low-potency hydrocortisone is not recommended for rosacea. While the dependency risk is lower than with potent steroids, rosacea skin is uniquely susceptible to steroid-induced changes. The initial improvement is deceptive and typically leads to longer and more frequent use. Non-steroidal alternatives such as azelaic acid or targeted Rosacea Injection Treatment address inflammation without creating dependency.
Q2: How can I tell if my skin is thinned from steroids?
Steroid-thinned skin typically appears shiny and somewhat translucent, with blood vessels visible beneath the surface. It bruises easily, and you may notice that the skin wrinkles or creases more readily when gently compressed. Dermoscopy or high-frequency ultrasound can quantify epidermal and dermal thickness if clinical assessment is uncertain.
Q3: Will my skin ever fully recover from steroid damage?
Most patients achieve substantial recovery with appropriate management. Epidermal thickness and barrier function typically normalize within 6 to 18 months after steroid cessation. However, established telangiectasia (dilated blood vessels) usually persists and may require vascular laser treatment. Dermal collagen recovery is slower and may remain incomplete in cases of prolonged high-potency steroid use.
Q4: Should I taper steroids gradually or stop abruptly?
For patients who have used steroids for less than four weeks, abrupt cessation is generally manageable. For longer-duration use, a gradual taper over two to four weeks reduces the severity of the rebound flare. Common tapering strategies include reducing application frequency from twice daily to once daily to every other day, or switching to a lower-potency formulation before discontinuing.
Q5: Can calcineurin inhibitors like tacrolimus replace steroids long-term?
Calcineurin inhibitors can serve as a useful bridge during steroid withdrawal, but they are not intended as permanent replacements. They carry their own considerations including initial application-site burning, theoretical long-term immunosuppression concerns, and cost. They should be used under dermatologic supervision for a defined period as part of a comprehensive recovery plan.
Q6: My doctor keeps prescribing steroids for my facial redness. What should I do?
Seek a second opinion from a dermatologist experienced in rosacea management. Steroid prescriptions for chronic facial redness represent a diagnostic and therapeutic mismatch that perpetuates the problem. A specialist can confirm whether your condition is primary rosacea, steroid-dependent rosacea, or another diagnosis, and implement an appropriate non-steroidal treatment plan.
About the Author
Dr. Ta-Ju Liu is the founder of Liusmed Clinic, where he specializes in regenerative medicine and minimal incision surgery. With extensive clinical experience treating complex dermatologic conditions including steroid-damaged rosacea skin, Dr. Liu integrates evidence-based pharmacologic strategies with advanced tissue regeneration techniques. His approach focuses on addressing the structural and neurovascular roots of skin damage rather than suppressing symptoms alone.
Disclaimer
This article is provided for educational and informational purposes only and does not constitute medical advice, diagnosis, or treatment. Individual skin conditions vary significantly, and treatment outcomes depend on numerous patient-specific factors. Always consult a qualified healthcare professional before modifying any medication regimen, including discontinuing topical steroids. No doctor-patient relationship is established through reading this content.
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

