Can You See Filler Through Your Skin? The Risks of Injecting in Thin-Skin Areas
Why You Can "See" Your Filler
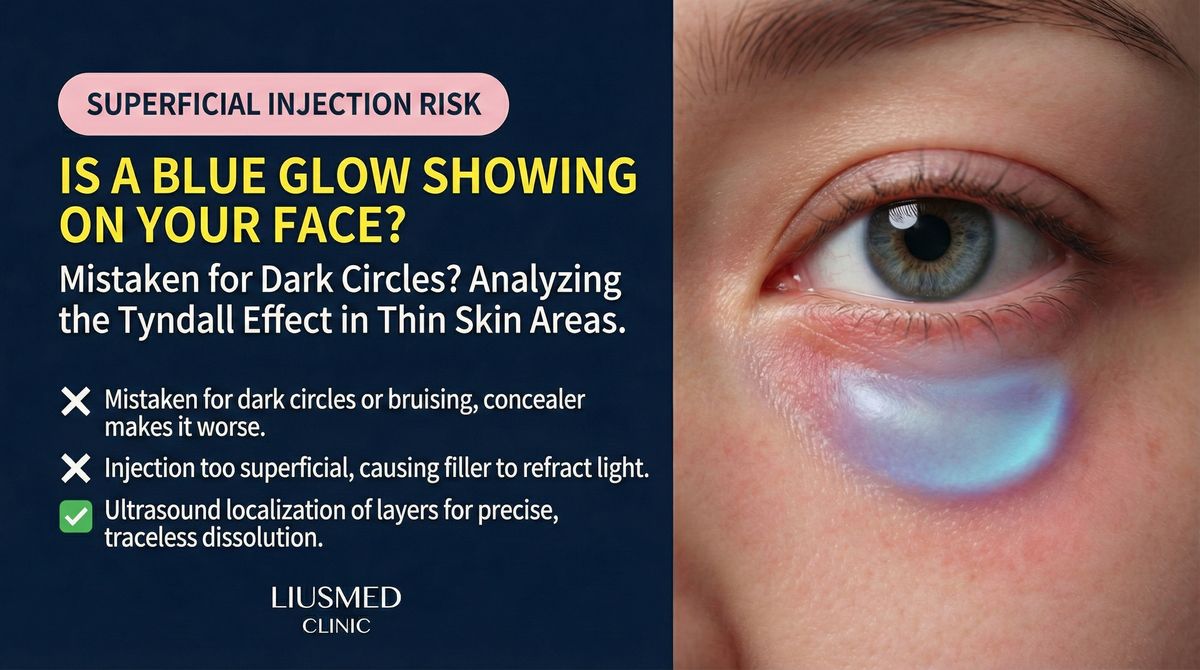
You had filler injected in your tear troughs or around the eyes. One day, turning your face at an angle in the mirror, you notice something: under certain lighting, there's a faint bluish shadow beneath the skin. At a different angle, it disappears. Or perhaps the shape of the filler is subtly visible through the thin skin, like a shallow ridge just beneath the surface.
This "seeing your filler" phenomenon is not rare in areas where skin is particularly thin.
What Is Filler Visibility
Two Common Manifestations
| Manifestation | Appearance | Most Affected Areas | Primary Cause |
|---|---|---|---|
| Tyndall effect | Bluish or blue-gray tint beneath skin | Tear troughs, lower eyelids | Hyaluronic acid scattering light |
| Contour show-through | Filler shape or edges visible | Tear troughs, temples, forehead | Injection too superficial |
| Color irregularity | Local skin tone differs from surrounding | Any thin-skin area | Filler altering light penetration |
| Surface irregularity | Visible bumps or waves | Forehead, nasal dorsum | Uneven filler distribution |
Key Insight: The Tyndall effect is an optical phenomenon—when hyaluronic acid is placed too superficially beneath the skin, incoming light is scattered by filler particles, producing a characteristic blue-gray hue. This is not infection or necrosis; it is the physics of light scattering.
Which Areas Are Most Vulnerable
High-Risk Thin-Skin Zones
Skin thickness varies dramatically by location. These areas have the thinnest skin and highest risk of filler visibility:
- Tear troughs and lower eyelids: Among the thinnest skin on the entire face, with virtually no subcutaneous fat buffer
- Periorbital region: Including the upper eyelid and the area below the brow tail
- Temples: Especially in lean individuals, where thin skin overlies the temporalis muscle
- Nasal dorsum and tip: Thin, high-tension skin where filler shapes are easily seen
- Upper forehead: Areas with minimal subcutaneous tissue
Key Insight: Skin thickness varies not only by location but also by individual. Aging, sun damage, and chronic corticosteroid use all thin the skin further, increasing the risk of filler becoming visible over time—even if it wasn't visible initially.
Factors That Make Filler Visible
It's Not Just About Injection Depth
While injection too superficial is the most common cause, other factors contribute to or worsen filler visibility:
- Inappropriate product selection: High-viscosity, large-particle products are more visible through thin skin
- Excessive volume: Even at the correct depth, over-injection can push filler toward the surface
- Filler migration: Filler originally placed at the correct depth may gradually shift toward more superficial planes
- Tissue atrophy: With aging, tissue covering the filler thins, making previously invisible filler gradually apparent
- Cumulative layering: Repeated injections in the same area can push some filler into superficial planes
The Value of Ultrasound Assessment
For filler visibility issues, ultrasound provides:
- Precise depth measurement: Exactly how many millimeters below the surface the filler sits, compared to the optimal depth
- Layer confirmation: Whether filler is in the dermis, subcutaneous tissue, or deeper planes
- Volume and distribution assessment: How much filler remains and how evenly it is distributed
- Multi-session layering: How fillers from different sessions have stacked
- Overlying tissue status: The thickness and integrity of the tissue covering the filler
Why Blind Dissolution Isn't the Best Approach
In thin-skin areas, especially the tear trough, blindly injecting dissolving enzyme carries risks:
- Over-dissolution can create hollowing worse than the original problem
- Difficult to control the precise zone of dissolution
- No confirmation that the problematic filler has actually been addressed
Ultrasound guidance enables precise targeting of only the area that needs treatment, avoiding both over- and under-correction.
Treatment Strategies
For Tyndall Effect
- Hyaluronic acid: Ultrasound-guided precise enzyme injection, targeting the most superficial filler layer. See Tyndall effect treatment for details.
- Prevention: The tear trough zone requires low-viscosity, small-particle products injected at the supraperiosteal plane rather than superficially.
For Contour Show-Through
- For HA (Hyaluronic Acid — sugar molecule naturally in skin, holds water): Targeted local enzyme dissolution of the visible component
- For non-HA fillers: Ultrasound-guided extraction of the superficial portion
- For migration-caused visibility: The underlying cause must be identified before planning treatment
For Cumulative Visibility
Problems caused by years of repeated injection may require staged treatment: remove the most superficial filler first, observe recovery, then reassess whether further treatment is needed.
Prevention: Wisdom for Thin-Skin Areas
- Respect anatomical differences: Not every area tolerates the same product and same depth
- Product matching: Thin-skin areas require low-viscosity, highly hydrophilic, small-particle products
- Less is more: The margin for error in thin-skin areas is minimal—conservative volume is the safe strategy
- Depth first: Inject as deep as feasible, using the body's natural tissue coverage to conceal filler
- Regular reassessment: As aging and tissue changes progress, previously appropriate filler may become visible
Key Insight: The best filler result is one where no one can tell you've had filler. In thin-skin areas, this requires not just technical skill but product wisdom, volume restraint, and long-term monitoring.
If you can see filler beneath your skin, schedule a consultation. Ultrasound can precisely measure filler depth and distribution, guiding the most appropriate treatment plan. See also the filler repair evaluation process.
Related Reading
- Tyndall Effect in Tear Troughs: The Blue-Gray Shadow Solution
- Why Do Fillers Migrate?
- The Filler Repair Evaluation Process
Related Services
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

