Why Simply 'Shattering Melanin' Only Treats the Symptom: The Secret of Dermal Inflammation and Senescent Fibroblasts
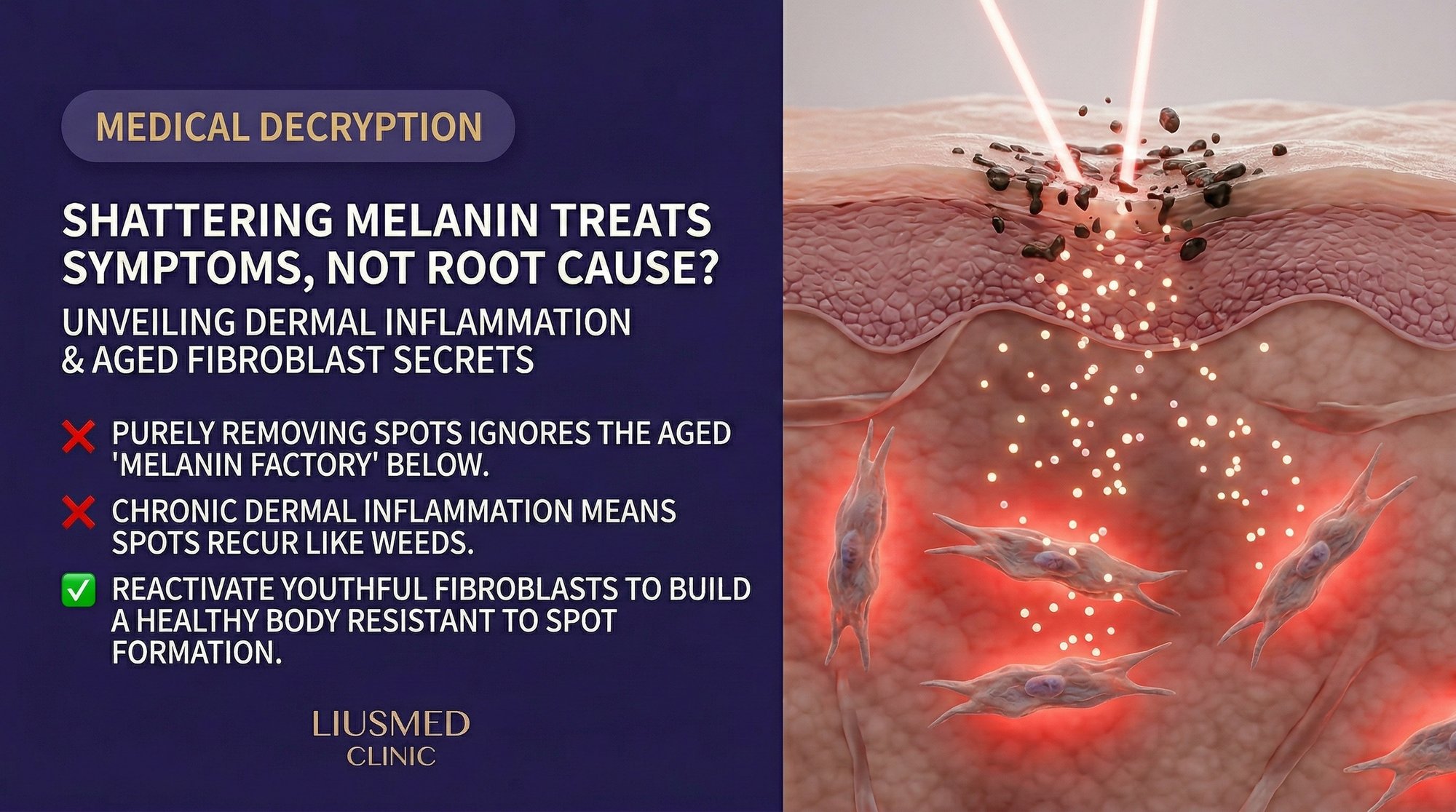
You have tried lasers, peels, and topical lightening agents. Each time the dark patches fade for a few weeks—then creep right back. The frustration is real, and you are not alone. Dermatologists worldwide report that melasma recurrence rates after conventional pigment-targeting therapies can exceed 50 percent within a year. The reason is deceptively simple: most treatments aim at the pigment itself while ignoring the inflamed microenvironment that commands melanocytes to keep producing it.
This article explains why "shattering melanin" is only half the story, what senescent fibroblasts have to do with stubborn melasma, and how a repair-first approach addresses the root cause rather than the symptom.
Table of Contents
- The Conventional Melanin-Destruction Model
- Chronic Dermal Inflammation: The Hidden Engine
- Senescent Fibroblasts and the SASP (Senescence-Associated Secretory Phenotype) Signal
- Why Laser and Peel Cycles Perpetuate Recurrence
- A Repair-First Framework for Refractory Melasma
- Comparing Destroy vs. Repair Strategies
The Conventional Melanin-Destruction Model
For decades, the dominant clinical logic for treating melasma has followed a straightforward sequence: identify excess melanin, break it apart with energy or chemistry, and let the body clear the debris. Q-switched (Q-switched laser) lasers, picosecond lasers, and chemical peels all operate on variations of this principle. Topical agents such as hydroquinone inhibit tyrosinase—the enzyme melanocytes use to synthesize melanin—while retinoids accelerate epidermal turnover to shed pigmented keratinocytes faster.
These strategies are effective at reducing visible pigment in the short term. The problem emerges when we ask a different question: why are the melanocytes overproducing in the first place?
Melanocytes do not operate in isolation. They sit at the base of the epidermis inside a complex signaling neighborhood that includes keratinocytes above, fibroblasts below, mast cells, endothelial cells, and an extracellular matrix scaffold. When that neighborhood is chronically inflamed, melanocytes receive persistent paracrine signals—stem cell factor (SCF), hepatocyte growth factor (HGF), endothelin-1, and various interleukins—that drive pigment synthesis regardless of how much melanin you remove from the surface.
Destroying the product without quieting the factory floor is a recipe for recurrence.
Chronic Dermal Inflammation: The Hidden Engine
Histological studies of melasma skin consistently reveal features that are absent in adjacent non-lesional skin: increased dermal vascularity, elevated mast cell counts, solar elastosis, and a fragmented basement membrane zone. These are not incidental findings. They point to a state of chronic, low-grade dermal inflammation that persists even when the epidermis looks calm.
This dermal inflammation creates a self-sustaining loop:
- UV exposure and heat activate keratinocytes, which release pro-inflammatory cytokines downward into the dermis.
- Mast cells degranulate, releasing histamine and tryptase that stimulate both angiogenesis and melanogenesis.
- Increased vascularity delivers more inflammatory mediators to the area, amplifying the signal.
- Fibroblasts in the upper dermis become activated and, over time, senescent—transforming from matrix-building cells into cytokine-secreting cells.
The result is a dermis that behaves like smoldering embers beneath apparently clear skin. Extinguishing the visible flame (melanin) without addressing the embers guarantees the fire returns.
Understanding this inflammatory microenvironment is precisely why the Melasma Injection Treatment protocol at Liusmed Clinic prioritizes dermal repair over pigment destruction.
Senescent Fibroblasts and the SASP Signal
Cellular senescence is a state in which cells stop dividing but refuse to die. Instead, they adopt a secretory phenotype known as the Senescence-Associated Secretory Phenotype (SASP). SASP-positive fibroblasts pump out a cocktail of inflammatory cytokines, matrix metalloproteinases (MMPs), and growth factors that reshape the tissue around them.
In melasma-affected dermis, the concentration of senescent fibroblasts is significantly higher than in matched non-lesional skin. Key SASP factors relevant to pigmentation include:
- IL-6 (Interleukin-1 beta / Interleukin-6) and IL-8: Pro-inflammatory interleukins that upregulate melanogenesis through paracrine signaling.
- MMP (Matrix Metalloproteinase)-2 and MMP-9: Enzymes that degrade the basement membrane, allowing melanin granules to drop into the dermis (so-called "pigment incontinence").
- SCF (Stem Cell Factor): A potent melanocyte activator that binds the c-KIT receptor and drives both melanocyte proliferation and dendrite extension.
- VEGF (Vascular Endothelial Growth Factor): Promotes angiogenesis, increasing local blood flow and delivering more inflammatory cells to the site.
This SASP-driven signaling explains why melasma is not simply a melanocyte disease. It is a tissue-level dysfunction in which the dermal stroma has shifted from a supportive, regenerative state to a chronic inflammatory state. Until you address the senescent fibroblast population and the damaged extracellular matrix they inhabit, the melanocytes will continue to receive "produce more pigment" commands.
Why Laser and Peel Cycles Perpetuate Recurrence
Here lies the paradox that frustrates both patients and clinicians: the very treatments designed to clear pigment can, under certain conditions, worsen the dermal inflammation that drives pigment production.
Laser-induced thermal injury, even at sub-ablative settings, triggers a wound-healing cascade in the dermis. In healthy skin, this cascade resolves cleanly. In melasma-prone skin—where the dermis is already chronically inflamed and populated with senescent fibroblasts—the additional thermal insult can:
- Stimulate mast cell degranulation, releasing more histamine and tryptase.
- Increase VEGF (Vascular Endothelial Growth Factor — new blood vessel signal) expression, promoting further vascular proliferation.
- Cause transient melanocyte activation through heat-shock protein signaling.
- Trigger additional fibroblast senescence via oxidative stress.
Chemical peels present a similar risk when applied aggressively. While superficial peels may offer modest benefit by accelerating epidermal turnover, medium-depth peels can breach the dermal-epidermal junction and provoke rebound inflammation.
The clinical pattern is familiar: initial improvement after treatment, a quiet period of several weeks, then gradual darkening that eventually matches or exceeds the baseline. Each cycle may add incremental dermal damage, making subsequent treatments progressively less effective—a phenomenon sometimes described as "treatment-resistant" melasma that is, in reality, treatment-aggravated melasma.
A Repair-First Framework for Refractory Melasma
If destruction perpetuates the cycle, the logical alternative is repair. A repair-first framework for melasma addresses the following layers:
1. Quench Dermal Inflammation Rather than adding thermal energy, deliver anti-inflammatory and vascular-stabilizing agents directly into the dermis. Tranexamic acid, for instance, inhibits plasminogen activation in the dermis, reducing both angiogenesis and mast cell activity. Intradermal delivery ensures therapeutic concentrations reach the target tissue without relying on epidermal penetration.
2. Modulate Senescent Fibroblasts Emerging strategies aim to either clear senescent cells (senolytic approaches) or suppress SASP output (senomorphic approaches). Certain growth factor cocktails and peptides can shift the fibroblast population back toward a regenerative phenotype, reducing the chronic cytokine burden on nearby melanocytes.
3. Rebuild the Basement Membrane The dermal-epidermal junction (DEJ) acts as a physical and biochemical barrier. When intact, it prevents melanin granules from dropping into the dermis and limits paracrine crosstalk between dermal and epidermal compartments. Stimulating collagen IV, laminin, and nidogen production helps restore this barrier. Learn more about DEJ damage in our companion article on basement membrane damage and pigment drop.
4. Precision Delivery Over Broad-Field Energy The Melasma Injection Treatment uses manual intradermal injection to place therapeutic agents at controlled depths and concentrations. Unlike laser energy that diffuses through tissue, injection allows the clinician to target the specific dermal layer where inflammation is most active—without collateral thermal damage to surrounding structures.
Comparing Destroy vs. Repair Strategies
| Dimension | Destroy-First (Laser / Peel) | Repair-First (Dermal Injection) |
|---|---|---|
| Primary Target | Melanin granules in epidermis/dermis | Inflamed dermal microenvironment |
| Mechanism | Photothermal fragmentation or chemical exfoliation | Anti-inflammatory, anti-angiogenic, matrix repair |
| Thermal Load on Dermis | Moderate to high | None |
| Effect on Senescent Fibroblasts | May increase senescence via oxidative stress | Aims to modulate or reduce SASP output |
| Basement Membrane Impact | Repeated energy can further degrade DEJ | Promotes DEJ component synthesis |
| Recurrence Pattern | High (often within 3-6 months) | Lower when dermal environment is stabilized |
| Best Suited For | Epidermal-dominant pigmentation, lentigines | Mixed or dermal-dominant melasma, refractory cases |
| Downtime | Variable (redness, peeling, PIH risk) | Minimal (pinpoint injection marks) |
Neither approach is universally superior. Epidermal pigmentation from sun damage may respond well to targeted laser therapy. However, for true melasma—especially the mixed or dermal-dominant variants—a repair-first strategy addresses the upstream cause rather than the downstream symptom.
Frequently Asked Questions
Q1: If melanin destruction is not enough, why do lasers sometimes seem to work for melasma?
Lasers can reduce visible pigment in the short term by fragmenting melanin granules. In patients with predominantly epidermal melasma and minimal dermal inflammation, this may produce lasting results. The problem arises in mixed or dermal-dominant melasma where chronic inflammation and senescent fibroblasts continuously drive melanocyte activity. For these patients, laser results tend to be temporary and may worsen with repeated sessions.
Q2: What exactly are senescent fibroblasts, and how do they affect my skin?
Senescent fibroblasts are dermal cells that have stopped dividing but remain metabolically active. Instead of building collagen and elastin, they secrete inflammatory cytokines, matrix-degrading enzymes, and growth factors—collectively called the Senescence-Associated Secretory Phenotype (SASP). This secretory output stimulates melanocytes, degrades the basement membrane, and promotes abnormal blood vessel growth, all of which perpetuate melasma.
Q3: Can I address dermal inflammation with topical products alone?
Topical agents face a significant delivery challenge: the stratum corneum is designed to keep molecules out. Most topical anti-inflammatory or lightening agents achieve their highest concentrations in the epidermis, with limited penetration into the mid-dermis where the inflammatory process is most active. Intradermal injection bypasses this barrier entirely, delivering therapeutic agents directly to the target tissue at controlled concentrations.
Q4: How does the Liusmed melasma injection protocol differ from standard mesotherapy?
Standard mesotherapy often uses automated devices (mesoguns or microneedling pens) that distribute product across a broad area at a uniform depth. The Melasma Injection Treatment at Liusmed Clinic uses manual hand injection, allowing the physician to adjust depth, volume, and spacing in real time based on the specific characteristics of each treatment zone. This precision reduces waste, minimizes unnecessary trauma, and concentrates the therapeutic payload where it is needed most.
Q5: How long does it take to see improvement with a repair-first approach?
Because the repair-first approach targets the underlying dermal environment rather than simply bleaching surface pigment, the timeline is different from laser treatments. Most patients begin to notice gradual, progressive lightening over four to eight weeks as inflammation subsides and the basement membrane begins to recover. The key advantage is that results tend to be more stable and less prone to the rapid rebound common after energy-based treatments.
Q6: Is it ever appropriate to combine laser treatment with dermal repair?
In selected cases, a carefully sequenced combination can be beneficial—for example, using low-fluence laser to address residual epidermal pigment after the dermal environment has been stabilized through injection therapy. The critical point is sequencing: repair the soil first, then cautiously address remaining surface pigment. Applying aggressive laser to an actively inflamed dermis risks triggering the recurrence cycle described in this article.
About the Author
Dr. Ta-Ju Liu is the founder of Liusmed Clinic in Taipei, Taiwan, where he leads a practice dedicated to regenerative medicine and minimal incision surgery. With dual expertise in dermatology and surgical repair, Dr. Liu developed the clinic's signature repair-over-destruction philosophy after observing that many refractory skin conditions—including melasma, rosacea, and filler complications—share a common root in chronic tissue-level inflammation. His clinical approach prioritizes restoring the skin's native repair mechanisms rather than adding further injury through aggressive interventional techniques.
Disclaimer
This article is provided for educational and informational purposes only and does not constitute medical advice, diagnosis, or treatment. Individual results vary based on skin type, condition severity, and treatment compliance. Always consult a qualified dermatologist or medical professional before beginning any treatment for melasma or other skin conditions. The information presented reflects the clinical perspective of the author and Liusmed Clinic as of the publication date.
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

