Hand-Injected Mesotherapy vs Machine Water Light Injection: Why Intimate Areas Need Human Precision
Summary
"Water light injection" is a mature facial aesthetic procedure, but its application to intimate anatomy (vulva, vestibule, vaginal mucosa) involves an asymmetry — the choice between "hand" and "machine" isn't about better-or-worse devices. It's that anatomic complexity, pain sensitivity, and individual variation determine which technique fits.
This article, anchored to the 2025 Maturitas multicenter RCT (single-session crosslinked hyaluronic acid mucosal injection) and related device studies, lays out the technical differences in depth control, customization, safety margin, and clinical scenario. This article makes no efficacy promises and does not replace physician evaluation.
1. Two Easily Confused Terms
1.1 Water Light Injection (Skin Booster Injection)
In facial aesthetics, "water light" typically means injecting low-concentration non-crosslinked or lightly crosslinked hyaluronic acid (HA — sugar molecule naturally in skin, holds water) into the dermis in shallow, multi-point, micro-dose fashion — improving hydration, luminosity, and elasticity.
1.2 Mesotherapy
Originating in 1950s France, mesotherapy (shallow micro-injection of nutrients/meds) literally means "injecting active ingredients directly into the mesoderm (dermis)." Modern clinical applications include HA, amino acids, vitamins, nucleotides, coenzymes, and custom formulations.
The full meaning of "hand-injected mesotherapy" = human-operated point-by-point injection + customizable HA / nutrient formulation + per-patient adjustment of depth and injection points.
"Machine water light" generally refers to multi-needle water light injectors (Vital Injector, Derma Shine, etc.) that deliver fixed needle count, fixed depth, and automated vacuum-assisted injection.
2. The Anatomic Challenge: Why "Uniformity" Isn't the Primary Goal
Vulvar, vestibular, and vaginal mucosa differ sharply from facial skin:
| Anatomic variable | Face | Intimate anatomy |
|---|---|---|
| Mucosa / skin thickness | Relatively uniform (except periorbital) | Highly variable (vulva vs vestibule vs vaginal mucosa) |
| Nerve density | Moderate | Very high, with marked local variation (especially vestibule) |
| Vascular distribution | Predictable | Highly individualized, varies with parity and menopausal status |
| Pain sensitivity | Consistent | Point-to-point variation is large (near clitoris vs posterior wall) |
| Mucosal mobility | Low | High (vaginal mucosa moves with posture / breathing) |
These differences mean — a "uniform injection" strategy that works well for faces can become a source of risk in intimate anatomy.
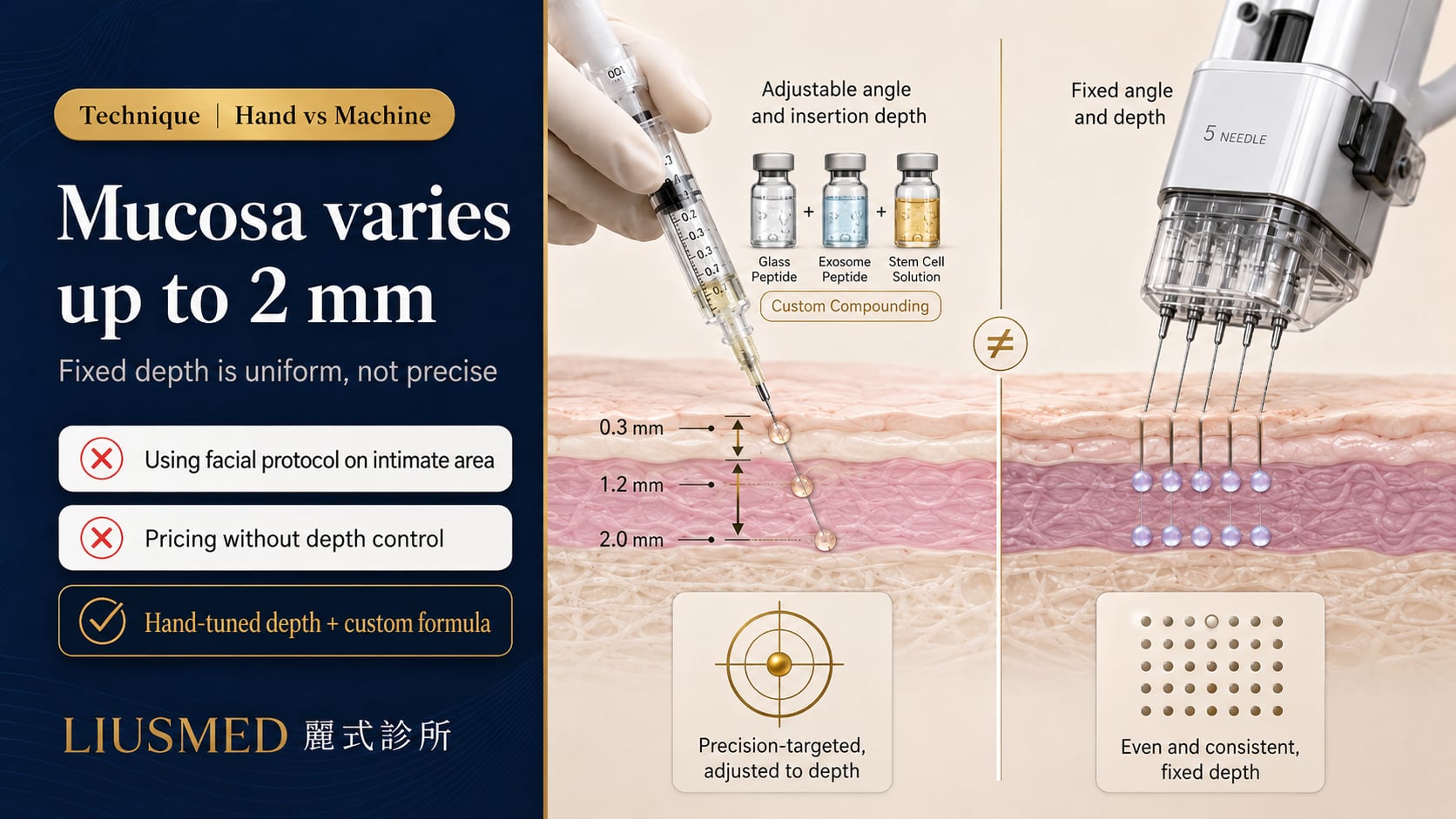
Example: machine injector fixed needle depths (commonly 0.5 mm, 1 mm, 1.5 mm settings) perform fine on the face, but in intimate anatomy, mucosal thickness can vary 0.5–2 mm between the vestibule, periurethral, and posterior wall in the same patient. That's not a variable a machine senses.
3. Core Technical Comparison
3.1 Depth Control
Machine water light:
- Needle depth set by device (typically three-step switch)
- Vacuum-assisted tissue lift, theoretically uniform depth
- Fast (multiple points per second)
Hand-injected mesotherapy:
- Depth adjusted point-by-point by the physician based on mucosal thickness, elasticity, and vascular position
- Uses "needle-feel, then advance, then inject" progressive technique
- Slower (~3–5 seconds per point), but high single-point precision
Clinical judgment: In intimate anatomy, "correct depth at each point" matters more than "same depth at every point."
3.2 Pain and Patient Experience
Machine injector vacuum suction is itself a stimulus source. On the face, suction is cushioned by subcutaneous fat. In intimate areas (especially the vestibule), direct suction on sensitive mucosa can amplify pain.
Hand injection can:
- Adjust pace in real time to patient feedback (slow, intermittent, or pause)
- Pair with topical anesthesia + buffering technique to reduce sharp pain
- Actively avoid or re-angle near the clitoris and other high-sensitivity zones
"Real-time adjustment" is the practical core advantage of hand injection — not "hand = painless."
3.3 Customization
Machine water light:
- Uses pre-filled injector cartridges (HA + fixed adjuncts)
- Dose and composition fixed; difficult to individualize
Hand-injected mesotherapy:
- Formulation tailored to symptom classification:
- Dryness-dominant: non-crosslinked HA + vitamin B complex + amino acids
- Elasticity loss: higher-crosslinked HA + peptides
- Sensitive / fragile: lower-concentration HA + calming ingredients
- Dose individualized per mucosal thickness and injection depth
Important note: The precondition for customization is that every ingredient must be legal, traceable, and backed by human safety data. Any injection with a "secret recipe" that won't disclose ingredients is a compliance red line.
3.4 Safety Margin: Room for the Unexpected
Adverse events in intimate areas include: vascular occlusion (filler-induced vascular blockage; very rare), local hematoma, excessive swelling, infection, neurologic irritation.
| Event | Machine response | Hand response |
|---|---|---|
| Injection into small vessel | Fixed flow — hard to decompress in real time | Physician can immediately retract needle and decompress |
| Sudden pain response | Must stop machine and reset | Can pause and reassess immediately |
| Encountering fibrosis / scar | Continues per setting | Can re-angle or skip that point |
| Inappropriate depth | Preset / fixed | Adjusted per tactile feedback |
This doesn't mean machine injection is unsafe — rather, intimate anatomy's individual variables fit human-adjusted decision frequency better.
3.5 Evidence Base
As of April 2026, in intimate applications:
- Maturitas (2025) multicenter RCT (Randomized Controlled Trial — gold-standard treatment comparison study) used single-session, hand-injected, crosslinked HA mucosal injection (n=116, single-blind placebo-controlled); 12-week primary outcomes showed improvement in dryness, dyspareunia (painful intercourse), and FSFI (Female Sexual Function Index — 19-item female sexual function score).1
- Arch Dermatol Res (2025) pilot RCT (HA vs PRP) also used hand injection; HA group showed greater sexual function improvement.2
- RCT evidence for machine water light injectors in intimate anatomy is currently very limited; most studies are facial applications or small observational series.
Conclusion: High-quality RCT evidence supporting HA mucosal injection in intimate anatomy uses hand injection. This doesn't mean machine injection is necessarily ineffective — it means the existing evidence base is built on hand injection.
4. When Might Machine Injection Be Considered?
Fairly speaking, machine water light isn't "unusable" — it has applicable scenarios:
- Large-area superficial hydration of vulvar skin (not involving vaginal interior or vestibular sensitive zones)
- Known individual uniform mucosa, no significant scarring or fibrosis
- Experienced physicians who can switch to hand injection for fine-detail reinforcement
Our stance: hand injection as the primary technique for intimate anatomy; machine injection as an adjunct only in specific scenarios, physician-decided per treatment plan — not patient-selected as a "package."
5. Four Key Parameters of Hand Injection
For patients choosing hand injection, physicians should at minimum disclose the following four parameters:
5.1 Needle Gauge and Type
- Common gauges: 27G, 30G, 32G
- Needle type: sharp (point) vs blunt cannula (linear spreading)
- Intimate anatomy preference: 27–30G sharp for multi-point, shallow, submucosal injection
5.2 Injection Depth
By anatomic layer:
- Anterior vaginal wall: ~1–1.5 mm (submucosal)
- Posterior vaginal wall: ~1–2 mm
- Vestibular mucosa: 0.5–1 mm (shallow, to avoid over-stimulation)
- Vulvar skin: 1–2 mm (dermis)
5.3 Per-Point Dose and Total Volume
Reference operational parameters from BMC Women's Health 2025 PRP (Platelet-Rich Plasma — concentrate of your own blood platelets rich in growth factors) RCT: one point per 5 mm, 0.4 mL per point, total volume 4 mL.3 HA injection dose varies with product concentration and cross-linking — requires individualization.
5.4 Injection Cadence
- Single-session full-segment vs divided sessions (e.g., monthly × 3)
- Cadence determined by symptom improvement and tolerance
- Not advisable to over-dose in a single session for a "one-shot" marketing effect
6. Common Myths
Myth 1: "Machine injection is more uniform, therefore more effective." The goal in intimate anatomy isn't "uniformity" — it's "precision matched to individual symptoms and anatomy." Uniform injection may over-dose sensitive zones and under-dose thick mucosa.
Myth 2: "Hand injection hurts more." Quite the opposite — hand injection pace adjusts to patient response; comfort is often better than machine-vacuum stimulation. Pain is individualized.
Myth 3: "Machine is cheaper." Per-session consumable cost may be slightly lower with machine injection, but treatment design, customization, and long-term outcome determine total value. Choosing "cheaper" as the primary criterion in intimate anatomy is a risk decision.
Myth 4: "I can choose hand or machine myself." This is a clinical decision, not a consumer choice. Physicians should synthesize symptom classification, mucosal status, pain tolerance, and budget. If a clinic lets you "package-shop" between hand and machine, it may reflect insufficiently nuanced clinical judgment.
7. Reasonable Expectations and Risks
7.1 Reasonable expectations
- Hand-injected mesotherapy HA may improve dryness, dyspareunia, and FSFI at 12 weeks (Maturitas 2025)1
- Effects are not permanent — follow physician-recommended cadence
- Individual variation is large — no promised scale improvement magnitude
7.2 Universal risks
- Transient injection-site pain, spotting, bruising, transient swelling or increased discharge
- Very rare: infection, allergic reaction, vascular occlusion, neurologic irritation
- Contraindications: active infection, severe coagulopathy, active skin disease at treatment site, pregnancy or possible pregnancy, allergy to formulation ingredients
7.3 Our stance
- No "one-time permanent" or "rejuvenation" marketing
- Formulation ingredients fully disclosed in informed consent
- Needle gauge, depth, injection-point map, and per-point dose recorded in the chart each session
8. Seven Technical Questions to Ask Your Physician
- Will you use hand or machine? Why does that fit my symptom classification this session?
- If hand — sharp needle or blunt cannula? What gauge?
- Is the formulation crosslinked or non-crosslinked HA? Mixed with other ingredients? What are they?
- What's the per-point dose, depth, and spacing you anticipate?
- Will you adjust technique specially near the clitoris, vestibule, and other sensitive zones?
- How is topical anesthesia performed? Expected pain level?
- If I experience marked discomfort during treatment, how will you adjust?
9. Eight Commonly Asked Questions
Q1. Hand injection is slower — will it take too long? Full intimate-area injection takes about 20–40 minutes — 10–15 minutes longer than machine injection. But that "extra time" is the core value — physician-body communication and per-point judgment.
Q2. Will I see effects immediately? Most patients feel mucosal hydration and elasticity improvement within 1–2 weeks; the Maturitas 2025 RCT primary endpoint was at 12 weeks1. Immediate sensation after a single session does not equal long-term efficacy.
Q3. Will hand injection affect my daily routine? Generally advise avoiding sexual activity, swimming, bathtub soaking, and vigorous exercise for 48–72 hours. Follow individual physician's post-treatment instructions.
Q4. Who is not suitable for hand-injected mesotherapy? Active infection, severe coagulopathy, active skin disease, pregnancy or possible pregnancy, and allergy to formulation ingredients. PCOS, diabetes, and other metabolic conditions require individual physician assessment.
Q5. Can hand injection and PRP be done together? In principle, yes — same-session layered or sequential sessions. Whether to combine is physician-judged per symptom classification, coagulation, allergy, and infection history. No add-ons for the sake of it.
Q6. Will it feel "puffy" afterwards? Brief mild swelling is a normal post-treatment response, usually resolving within 48 hours. If it persists beyond a week, or is accompanied by pain / abnormal discharge, return for reassessment promptly.
Q7. Treatment cadence? Depends on symptom severity and product properties. The Maturitas 2025 RCT primary endpoint was 12-week follow-up after a single injection; in practice, some patients need a booster at 3–6 months.
Q8. Why can't I just choose machine injection myself? The complex anatomy and pain sensitivity of intimate areas mean that "one-click uniform injection" isn't appropriate as a primary strategy. This is a clinical judgment, not a consumer choice.
10. Back to Process: Our Technical Position
We chose hand-injected mesotherapy as the primary injection technique for female intimate regeneration for three reasons:
- Evidence base: Maturitas 2025 multicenter RCT and recent HA injection studies all used hand injection
- Safety margin: Intimate anatomy requires the decision frequency of real-time human adjustment
- Customization: Different formulations and doses per symptom classification (dryness / elasticity / sensitivity)
→ Service page: Female Intimate PRP + Hand-Injected Mesotherapy → Related reading: Female Intimate Regenerative Therapy — Complete Overview of Four Modalities
If you'd prefer to understand before deciding, ask 3 anonymous questions via LINE. We won't record your real name until you decide to book an in-person evaluation — no selling, no promises, no "machine is more uniform" or "hand is more premium" marketing lines. Technique choice — based on your body.
References
Medical Disclaimer
This article is for health education reference only and does not replace gynecology / urogynecology evaluation. All injection techniques carry risks — outcomes vary individually and no specific result can be guaranteed. All treatment decisions should rest on individual physician evaluation, informed consent, and shared decision-making.
Related Services
Footnotes
-
Marchand Lamiraud F, et al. Cross-linked hyaluronic acid vaginal injection in postmenopausal women: a multicenter, single-blind, placebo-controlled RCT. Maturitas, 2025. DOI (Digital Object Identifier): 10.1016/j.maturitas.2025.108264 ↩ ↩2 ↩3
-
Ragy S, et al. Hyaluronic acid vs platelet-rich plasma injection for vulvovaginal atrophy: a pilot RCT. Archives of Dermatological Research, 2025. DOI: 10.1007/s00403-025-03820-z ↩
-
Hamid ASA, et al. Platelet-rich plasma vs saline injection for postmenopausal VVA (Vulvovaginal Atrophy): double-blind RCT (n=60). BMC Women's Health, 2025. DOI: 10.1186/s12905-025-04076-5 (injection-point map and per-point dose serve as reference for hand injection practice) ↩
Want to learn more?
Schedule a consultation for professional evaluation and advice