Why You Should Never Allow Blind Aspiration or Blind Curettage for Aesthetic Complications
"I Just Wanted It Removed—How Did Things Get Worse?"
Behind this statement is often a painful treatment experience. After developing lumps or complications from filler, the patient found a practitioner willing to "take the material out," only to discover after the procedure that the depression was worse, the skin surface was uneven, or there was numbness and asymmetry.
Where did things go wrong? In most cases, the problem was that the practitioner could not see.
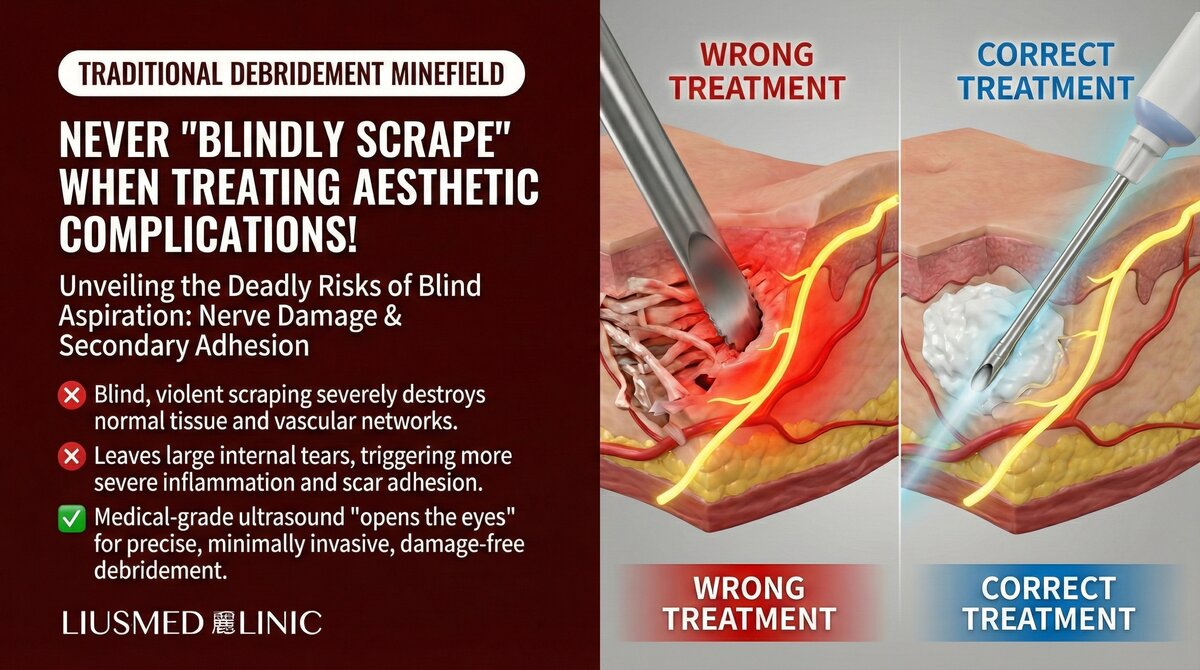
Without ultrasound or other imaging guidance, the practitioner inserts a needle, cannula, or curette into the tissue, relying on tactile feedback and experience to "feel" the filler and attempt to aspirate or scrape it out. This is known as "blind aspiration" or "blind curettage." On other parts of the body, the risk of such procedures may be manageable. But on the face—densely populated with nerves, vessels, and delicate anatomical structures—blind manipulation can produce catastrophic consequences.
What Are Blind Aspiration and Blind Curettage?
Blind Aspiration
Inserting a needle or cannula into tissue without imaging guidance, attempting to withdraw filler material through suction. The practitioner relies entirely on palpation and tactile feedback to locate the filler.
Blind Curettage
Inserting a curette or specialized instrument into tissue without imaging guidance, attempting to scrape out filler material and surrounding capsule tissue. This also relies entirely on touch and clinical judgment.
| Technique | Guidance Method | Precision | Risk Level |
|---|---|---|---|
| Blind aspiration | None—tactile only | Low | High |
| Blind curettage | None—experience only | Low | Very high |
| Ultrasound-guided aspiration | Real-time imaging | High | Low |
| Ultrasound-guided micro-extraction | Real-time imaging + precision instruments | Very high | Lowest |
Five Critical Risks of Blind Aspiration and Curettage
Risk 1: Unable to Confirm Material Type
Without ultrasound, the practitioner cannot confirm the filler material before the procedure. Different materials have different textures, tissue adhesion patterns, and optimal removal strategies. Silicone extraction is entirely different from HA (Hyaluronic Acid — sugar molecule naturally in skin, holds water) extraction, and blind manipulation cannot distinguish between them.
Risk 2: Nerve Damage
The face has an extremely dense distribution of motor and sensory nerves. Blind needle or curette movements can damage these nerves, causing:
- Localized numbness or sensory disturbance
- Facial muscle weakness or asymmetry
- Mouth drooping
- Permanent nerve injury
Risk 3: Vascular Injury
The facial vascular system is complex with numerous anatomical variations. Blind manipulation can puncture critical vessels, leading to:
- Significant bleeding
- Deep hematoma
- Skin necrosis (if supply arteries are compromised)
- Vision impairment (in extreme cases)
Risk 4: Excessive Removal of Normal Tissue
One of the greatest problems with working blind is the inability to distinguish the boundary between filler and normal tissue. During blind curettage, the practitioner may inadvertently scrape away normal fat and connective tissue, causing:
- Severe tissue depression
- Irreversible volume loss
- Irregular surface contours
Risk 5: Incomplete Removal and Recurrence
Paradoxically, blind procedures can also result in insufficient removal. Because the full extent of the filler cannot be visualized, the operator may miss residual material, leading to persistent lumps that require further treatment.
Key Insight: The fundamental contradiction of blind aspiration and curettage is this: to avoid damage, the practitioner tends to operate conservatively—but conservative operation may leave material behind. To achieve thorough removal, more aggressive technique is needed—but aggressive technique without visual guidance increases the risk of damaging normal structures. Without imaging guidance, this contradiction cannot be resolved.
Common Sequelae We See After Blind Curettage
We regularly see patients in our clinic who seek help after undergoing blind curettage elsewhere. Common sequelae include:
- Irregular surface contours: Caused by uneven removal of normal tissue
- Skin tethering to deep tissue: Scar tissue pulls the skin down to deeper layers
- Residual lumps on the opposite side: Blind curettage only addressed what could be felt
- Post-operative infection: Open wounds increase infection risk
- Persistent numbness: Sensory nerves inadvertently damaged
Key Insight: The damage from blind curettage is sometimes harder to repair than the original problem. A filler lump can potentially be removed through precise minimally invasive surgery, but the tissue defects and scar adhesions caused by blind curettage multiply the complexity and difficulty of repair by several fold.
Ultrasound Guidance: The Revolutionary Shift from Blind to Seeing
High-resolution ultrasound has completely transformed how filler complications are managed. It provides more than just "better positioning"—it represents an entirely different treatment philosophy: do not begin any intervention until you can clearly see all the structures involved.
What Can Ultrasound Visualize?
- Precise filler location and depth
- Material characteristics (different materials show different echogenic signatures)
- Degree and thickness of encapsulation
- Surrounding vascular and nerve pathways
- Real-time position of surgical instruments
Ultrasound-Guided Minimally Invasive Extraction Process
- Pre-procedure scanning: Creates a complete "map" marking filler locations and structures to avoid
- Real-time guidance: Continuous ultrasound monitoring throughout the procedure confirms instrument positioning
- Precise extraction: Under visual confirmation, only filler material and necessary capsule tissue are removed
- Intraoperative verification: Real-time confirmation of clearance completeness ensures nothing is missed and nothing is over-removed
- Post-procedure follow-up: Ultrasound monitoring of recovery
For more detailed information on the minimally invasive extraction technique, see: Filler Lump Extraction Technique Explained.
Why Traditional Debridement Is Unacceptable on the Face
In certain medical contexts, debridement is necessary and effective—for example, removing necrotic tissue from deep wounds. But applying the same blind debridement logic to facial filler complications is an inappropriate transplantation of general surgical concepts into a field that demands fine-detail precision.
The face is unique because:
- Every millimeter of tissue can affect appearance
- Symmetry requirements are extremely strict
- Nerve and vessel density is far higher than elsewhere on the body
- Patient sensitivity to outcomes is extremely high
In this environment, "roughly knowing where the material is" is not sufficient. You must "precisely know where the material is, and what surrounds it."
How to Choose the Right Treatment Approach
If you are facing filler complications that require intervention, consider the following when choosing a treatment approach:
- Does the practitioner use ultrasound for pre-procedure assessment?
- Is real-time imaging guidance used during the procedure?
- Can the practitioner identify the filler material type and exact location before treatment?
- Is the treatment performed through a tiny pinhole or does it require a surgical incision?
We recommend starting with a comprehensive ultrasound evaluation to clearly understand your situation before making treatment decisions. Schedule a consultation and let us use a visible approach to find the safest solution for you.
Conclusion
In medicine, seeing is always safer than guessing. The fundamental problem with blind aspiration and curettage is not that the practitioner lacks skill—it is that the absence of visual guidance itself represents an uncontrollable risk. When ultrasound technology already enables us to clearly visualize every layer of facial anatomy, performing procedures blindly is an unnecessary gamble. Your face deserves to be seen before it is treated.
Related Services
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

