Your Body vs. Injectables: The Complete Foreign Body Immune Response
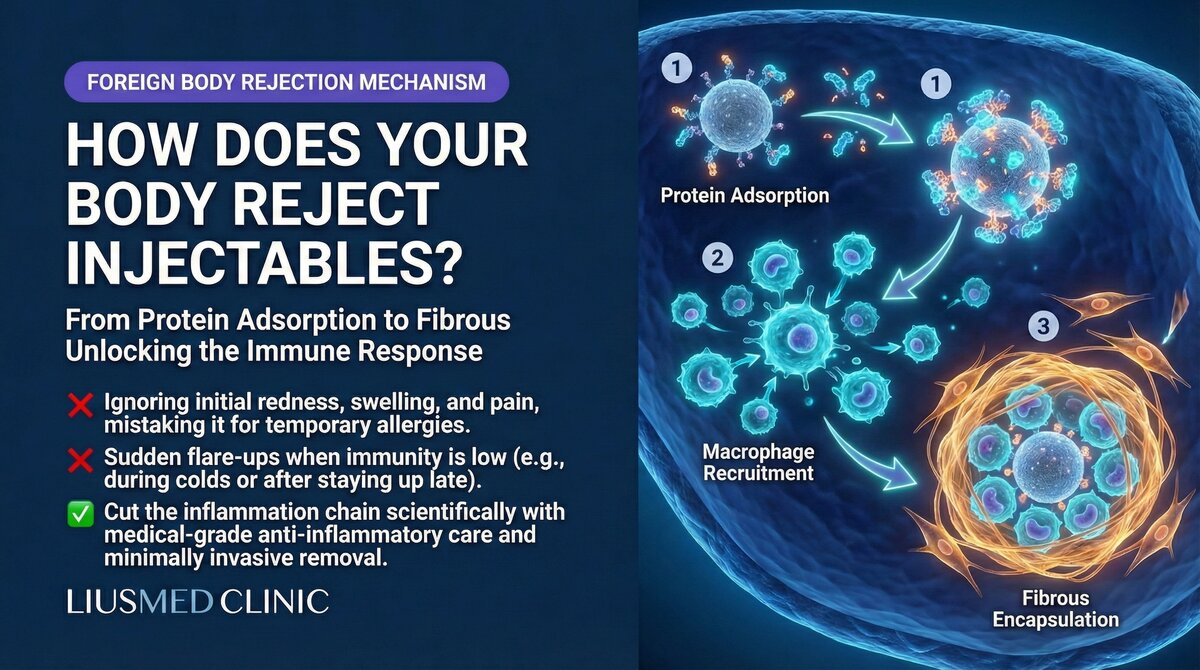
The Moment of Injection, the War Begins
You are seated in the treatment chair as the physician pushes filler into your skin. You feel mild pressure and fullness. But at the cellular level, a meticulously orchestrated immune storm has already begun.
Regardless of filler brand, material, or quality — whenever foreign material enters tissue, the immune system responds. The only differences are the intensity and duration of that response.
Key Insight: All filler injections trigger a foreign body response. The question is not "will there be a response" but "how strong, how long, and will it evolve into a clinical problem." Understanding this process is the foundation for knowing when to intervene and when to observe.
The Complete Timeline of the Foreign Body Immune Response
Phase 1: Acute Inflammation (0–72 Hours)
The injection itself causes tissue injury. Damaged cells and vascular endothelial cells immediately release signaling molecules:
Danger-Associated Molecular Patterns (DAMPs): Alarm molecules from damaged cells, including HMGB1, ATP, and heat shock proteins. These tell the immune system "something is wrong here."
Vascular response: Local capillary dilation and increased permeability. Plasma proteins leak into tissue spaces, creating the post-injection swelling patients commonly experience.
Neutrophil influx: Within hours, neutrophils are recruited from the bloodstream to the injection site as the immune system's "rapid response force."
| Timeline | Event | Clinical Manifestation |
|---|---|---|
| 0–1 hours | DAMPs release, complement activation | Injection site redness |
| 1–6 hours | Neutrophil infiltration, vasodilation | Local warmth, swelling |
| 6–24 hours | Neutrophil peak, cytokine release | Maximum swelling, mild bruising |
| 24–72 hours | Neutrophils decline, monocytes arrive | Swelling begins to subside |
Phase 2: Subacute Transition (3 Days–2 Weeks)
Neutrophils have short lifespans and undergo apoptosis after completing their mission. They are replaced by longer-lived, more versatile monocytes and macrophages.
The dual role of macrophages:
- M1 type (pro-inflammatory): Dominant initially, secreting TNF-alpha, IL-1-beta to maintain inflammation
- M2 type (reparative): Gradually increasing, secreting IL-10, TGF-beta to promote tissue remodeling
This M1-to-M2 polarization shift is the critical fork that determines whether the immune response "resolves" or "becomes chronic."
Phase 3: Chronic Foreign Body Response (2 Weeks–Months)
If macrophages cannot clear the filler — and they truly cannot digest synthetic materials — the response enters the chronic phase.
Foreign body giant cell formation: Multiple macrophages fuse into large multinucleated cells attempting to surround larger filler particles. For the detailed mechanism, see granuloma formation and the immune mechanism.
Fibroblast activation: TGF-beta continuously stimulates fibroblasts to synthesize collagen, forming a fibrous capsule around the filler.
Neovascularization: VEGF (Vascular Endothelial Growth Factor — new blood vessel signal) drives new vessel formation in the inflammatory zone, supplying cells and nutrients for the ongoing immune response.
Phase 4: Encapsulation and Stabilization (Months–Years)
Ultimately, the immune system adopts a "ceasefire" strategy — since it cannot destroy the enemy, it walls it off.
The fibrous capsule matures gradually, forming a relatively stable barrier separating filler from surrounding tissue. Under ideal conditions, this state can persist for years without clinical problems. Learn more about how encapsulation causes dissolvers to fail.
Key Insight: Encapsulation is the immune system's "best compromise." It is not a perfect solution — the filler is still there, immune surveillance continues. Any factor that disrupts this equilibrium (infection, trauma, immune status changes) can reignite a foreign body response that has been silent for years.
What Factors Amplify the Foreign Body Response?
Not every foreign body response leads to clinical problems. The following factors can push a "normal response" into "clinically problematic complication":
Material Factors
- Particle size: 1–10 micrometer particles most readily trigger macrophage responses
- Surface properties: Rough or charged surfaces increase protein adsorption, amplifying immune response
- Degradation products: Incomplete degradation intermediates may be more immunostimulatory than the original material
- Impurity content: Residual endotoxins or proteins from manufacturing can significantly amplify responses
Host Factors
- Genetic predisposition: Certain HLA genotypes correlate with stronger foreign body responses
- Autoimmune background: Patients with immune dysregulation have less predictable responses
- Co-infection: Biofilm formation can transform low-grade chronic inflammation into acute flares
- Systemic events: Fever, vaccination, other infections can "reawaken" silent foreign body responses
Injection Factors
- Volume: More material means greater immune system burden
- Tissue plane: Different layers have different immune reactivity
- Repeat injections: Cumulative effects may exceed the immune system's tolerance threshold
- Mixed materials: Interactions between different materials may produce unpredictable immune amplification
Treatment Logic from an Immunological Perspective
Understanding the complete foreign body immune response clarifies treatment strategy:
Medical therapy: Steroids, 5-FU, and similar drugs can modulate immune response intensity but cannot terminate the root cause. They are "symptom management tools," not "cures."
Physical removal: Removing the foreign body removes the immune response target. Ultrasound-guided minimally invasive extraction can precisely locate and remove filler, fundamentally terminating the chronic foreign body response cycle.
Timing matters: Intervening early in encapsulation makes removal relatively easier. Waiting until the capsule is fully mature and fibrosis is severe increases both technical difficulty and tissue damage risk.
| Treatment Strategy | Target | Duration of Effect | Indication |
|---|---|---|---|
| Steroid injection | Suppress inflammation | Temporary | Acute inflammation control |
| 5-FU injection | Suppress fibroblasts | Temporary | Fibrosis-dominant nodules |
| Hyaluronidase | Dissolve HA filler | Potentially lasting (if complete) | Non-encapsulated HA |
| Ultrasound-guided extraction | Remove foreign body | Lasting | All types of filler residue |
Know Your Immune System
Your immune system is not your enemy — it is a devoted guardian protecting you. Every response it mounts against filler is an action it believes protects you from foreign threats.
The problem is not the immune system, but the impossible task we impose on it: coexisting with a foreign material that will not disappear.
If you suspect your filler is triggering immune responses — lumps appearing years after injection, recurrent swelling, persistent nodules — ultrasound assessment can help confirm the situation. Contact us for evaluation. Learn about our filler repair services.
Key Insight: Your body never truly "accepts" foreign filler. It simply switches between strategies — from attack to containment to surveillance. Understanding this explains why filler problems can surface years after injection, and why the fundamental solution always remains: remove the foreign body.
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

