Still Swollen a Month After Filler? How to Tell Normal Swelling from a Delayed Inflammatory Reaction (DIR)
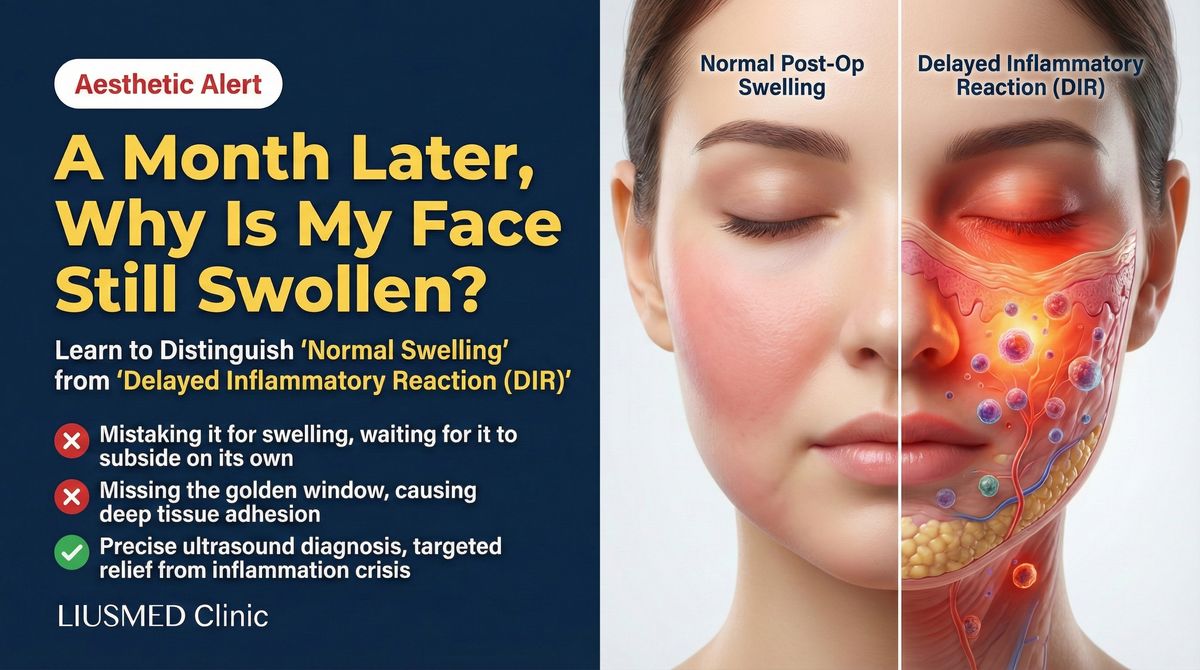
Your Face Is Still Swollen a Month After Filler—Is That Normal?
You received facial filler injections four weeks ago. The initial bruising and swelling resolved within a few days. But two or three weeks later, you noticed the treated area seemed to swell again. Some mornings it looks particularly pronounced. Sometimes the area feels slightly warm to the touch. You called your original doctor, who said, "That's normal—just give it time."
But something feels off.
That instinct is often correct. Swelling that persists beyond two weeks after filler injection—especially swelling that resolves and then returns—is likely not simple post-procedure edema. It may be a delayed inflammatory reaction (DIR) that requires active management.
Characteristics of Normal Post-Procedure Swelling
What Your Body Is Doing
Every filler injection is, by nature, a form of micro-trauma. The needle punctures skin, filler occupies tissue spaces, and local blood vessels experience mechanical compression. All of this triggers the body's normal inflammatory repair response.
Normal post-procedure swelling typically presents as follows:
| Feature | Normal Post-Procedure Swelling | Delayed Inflammatory Reaction (DIR) |
|---|---|---|
| Onset | Immediately to 48 hours post-injection | 2 weeks to several months post-injection |
| Duration | Gradually resolves over 3–14 days | Persistent or recurring |
| Distribution | Symmetric, diffuse | Focal, asymmetric |
| Texture | Soft, springs back when pressed | Firm, tender to palpation |
| Skin color | Normal or mild bruising | Pinkish-red, dusky |
| Temperature | Normal or slightly warm | Noticeably warm |
| Response to ice | Significant improvement | Limited effect |
| Trajectory | Improving daily | Fluctuating or worsening |
Key Insight: The defining characteristic of normal post-procedure swelling is continuous improvement. Even if recovery is slow, the trajectory is always toward resolution. If swelling returns after initially subsiding, or shows no improvement after two weeks, it is not normal swelling.
Factors That Affect Normal Swelling Severity
Even with normal swelling, there is significant variation between individuals and injection sites:
- Injection site: The lips and periorbital area have loose tissue and rich vascularity, producing significantly more swelling than the cheekbones or chin
- Filler type: Highly hydrophilic hyaluronic acid products (such as certain large-molecule cross-linked formulations) cause more edema than less hydrophilic products
- Volume injected: Larger volumes create greater mechanical tissue displacement
- Individual constitution: People prone to fluid retention (e.g., those with pronounced premenstrual symptoms) tend to experience more pronounced post-procedure swelling
- Injection technique: Blunt cannula techniques generally cause less tissue disruption than sharp needle approaches
The True Nature of Delayed Inflammatory Reactions (DIR)
Red Flags Beyond "Normal Swelling"
A delayed inflammatory reaction is a clinical concept encompassing multiple pathological mechanisms. It is not a single disease but a group of abnormal inflammatory phenomena that appear after a delay following injection. DIR may be driven by:
- Biofilm formation: Bacteria organizing into dormant colonies on the filler surface (see the biofilm article)
- Foreign body granuloma: A chronic granulomatous response where the immune system identifies filler as a foreign body
- Immune-mediated reaction: Allergic or autoimmune responses triggered by filler components
- Low-grade infection: Subclinical infection with bacterial counts too low for conventional culture detection
- Mechanical irritation: Persistent inflammation from migrated filler compressing surrounding tissue
Clinical Presentation of DIR
DIR manifestations can be highly variable, but several features are common:
Early signals (2–8 weeks post-injection):
- Persistent sensation of "tightness" or "fullness" at the injection site
- Mild tenderness on palpation, but not severe pain
- Morning swelling particularly pronounced, partially improving during the day but never fully resolving
- Subtle skin redness over the surface
Progressive signals (2–6 months):
- Swelling begins to fluctuate—good for a few days, then suddenly worse
- Exacerbated by colds, fatigue, or stress
- Palpable nodules or firm lumps at the injection site
- Persistent discoloration—dusky red or dark pink
Late signals (beyond 6 months):
- Palpable lumps even during "good" periods
- Increasingly visible asymmetry
- Skin texture changes—roughness, enlarged pores
- Altered thermal sensation at the injection site
Key Insight: The most dangerous characteristic of DIR is its insidious progression. Early symptoms are frequently dismissed as "normal post-procedure reaction," causing patients to miss the optimal window for early intervention. When in doubt, err on the side of caution rather than wishful thinking.
Three Key Questions for Self-Assessment
Before you can secure a professional evaluation, these three questions can help you preliminarily assess the nature of your swelling:
Question 1: What Is the Trajectory of Swelling?
Using your phone, take a photograph at the same time, with the same lighting, and from the same angle every day. After seven days, compare them:
- If each photo looks slightly better than the previous day → likely normal swelling resolving
- If photos look roughly the same with no change → further evaluation needed
- If some days show noticeably more swelling → highly suspicious for DIR
Question 2: Does Swelling Correlate with Systemic Health?
Recall whether your swelling worsens in the following situations:
- After catching a cold or illness
- Around your menstrual cycle
- During periods of sleep deprivation or high stress
- After vigorous exercise or sauna use
- After receiving a vaccination
If swelling clearly correlates with systemic immune status, this suggests a chronic inflammatory focus at the filler site—possibly biofilm or foreign body reaction.
Question 3: What Does It Feel Like When You Press?
- Soft like gelatin, slowly bouncing back → more likely normal filler
- Firm with distinct borders → possible encapsulation or granuloma
- Dough-like, moveable but with resistance → possible filler migration
Why Ultrasound Is the Gold Standard for Diagnosis
See Before You Treat
At Liusmed Clinic, the first step in managing filler complications is always ultrasound examination—not guessing, not "trying hyaluronidase to see what happens," and certainly not blindly prescribing antibiotics.
High-resolution ultrasound directly reveals:
- Exact filler location: Is it in the correct tissue plane, or has it migrated?
- Filler morphology: Is it evenly distributed, or has it aggregated into masses?
- Surrounding tissue status: Is there inflammatory fluid collection? Abnormal vascularity?
- Capsule presence: Is the filler surrounded by a fibrous capsule? (See encapsulation and dissolver failure)
This is the core of our "see before you treat" philosophy. Managing filler complications without ultrasound guidance is like operating in the dark—you do not know what you are treating, and you cannot confirm whether your treatment is reaching the right target.
What Ultrasound Can Differentiate
| Ultrasound Finding | Possible Diagnosis | Recommended Approach |
|---|---|---|
| Uniform hypoechoic mass, no vascularity | Normal filler presence | Observation or hyaluronidase |
| Hypoechoic mass with hyperechoic rim | Encapsulated filler | Ultrasound-guided pinhole extraction |
| Surrounding fluid collection and increased vascularity | Active inflammation/infection | Antibiotics + ultrasound-guided drainage |
| Irregular hyperechoic focus with posterior shadowing | Calcification or foreign body granuloma | Ultrasound-guided pinhole extraction |
| Filler not in original injection plane | Filler migration | Assess migration path, plan extraction |
Key Insight: Two patients presenting with "still swollen after one month" may show completely different findings on ultrasound—and the correct treatment depends on what you see, not what you assume.
Common Management Mistakes
1. "Just Wait and See"
For genuine DIR, waiting only allows progression. Untreated early inflammation may advance to fibrosis and tissue degeneration, increasing the complexity of subsequent treatment.
2. Repeated Courses of Antibiotics
If biofilm is the cause of swelling, antibiotics can only temporarily suppress active bacteria escaping from the biofilm surface—they cannot eradicate the dormant core colony. Repeated antibiotic courses also increase the risk of antibiotic resistance.
3. Blind Hyaluronidase (enzyme that dissolves HA filler) Injection
Without ultrasound guidance, you cannot confirm:
- Whether hyaluronidase has actually reached the filler
- Whether the filler is encapsulated (in which case hyaluronidase cannot contact the filler at all)
- Whether you are dissolving native tissue that should not be dissolved
4. Vigorous Massage
If swelling is caused by filler migration or biofilm, massage will only spread the filler further or exacerbate the inflammatory response.
When to Seek Immediate Medical Attention
The following situations require urgent care—do not continue waiting:
- Skin blanching or turning purple: May indicate vascular occlusion, the most critical filler complication
- Severe pain that continues to intensify: Suggests acute infection or vascular compromise
- Fever accompanied by injection site redness and swelling: Indicates risk of systemic infection
- Sudden blurring or loss of vision: The most critical scenario—filler embolization into the ophthalmic arterial system
- Purulent discharge or skin breakdown at the injection site: Infection has penetrated to the skin surface
Our Approach at Liusmed Clinic
When you come to Liusmed Clinic with "still swollen a month after filler," our standard evaluation process includes:
- Detailed history: Injection timing, filler type, volume, treating physician, and the chronological pattern of swelling
- High-resolution ultrasound scan: Confirming filler location, morphology, and surrounding tissue status
- Clinical diagnosis: Integrating history with ultrasound imaging to differentiate between normal edema, DIR, infection, encapsulation, migration, and other conditions
- Treatment plan: Developing an individualized treatment strategy based on the diagnosis
- Follow-up: Post-treatment ultrasound monitoring to confirm improvement
When filler removal is indicated, we employ ultrasound-guided pinhole extraction—under real-time ultrasound guidance, precisely removing the problematic filler through a single, minimally invasive entry point. No incisions. No scraping. No blind dissolving.
A Message for Those Who Are Worried
If you are experiencing persistent swelling after injection, I understand your anxiety. You may have searched countless articles online, each one making you more frightened. What I want you to know is this: the vast majority of filler complications, when correctly diagnosed and promptly managed, show significant improvement.
The key is not fear—it is action. Do not let "maybe it will resolve on its own" delay the optimal window for treatment.
If you are unsure about your situation, schedule a consultation and let us use ultrasound to see exactly what is happening. When you can see it, you can treat it.
Related Reading
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

