Hyaluronidase Failed After 3 Injections? 7 Reasons Why Dissolving Enzymes Don't Work
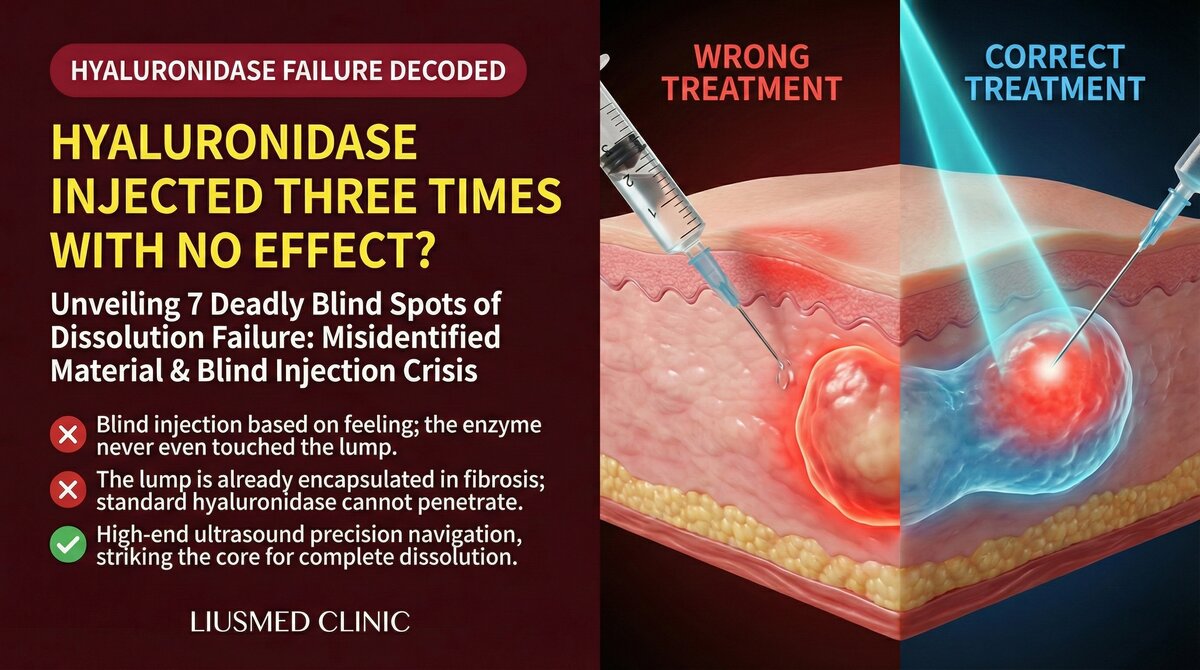
Three Rounds of Dissolving Enzymes and the Lump Is Still There
This is one of the most common frustrations we hear in our clinic. Patients arrive exhausted and confused, telling us: "I have already had three—even five—rounds of hyaluronidase at other clinics, and the lump has not changed at all." Some begin to suspect their body chemistry is unusual. Others are told to "just keep trying a few more rounds."
The truth is that hyaluronidase is not a universal solution. It has a specific mechanism of action and a defined scope of effectiveness. In clinical practice, dissolving enzyme failure is far more common than most people realize. Among patients who come to our clinic for help, over sixty percent have already attempted at least one round of hyaluronidase elsewhere without improvement.
This article provides a complete analysis of the seven most common reasons hyaluronidase fails, helping you understand the root of the problem rather than continuing to try blindly.
Reason 1: The Material Is Not Hyaluronic Acid
This is the most fundamental and most frequently overlooked cause. Hyaluronidase (enzyme that dissolves HA filler) has a highly specific mechanism—it can only cleave the particular chemical bonds within hyaluronic acid molecules. If the injected material is not HA (Hyaluronic Acid — sugar molecule naturally in skin, holds water), the dissolving enzyme will have absolutely no effect.
Common misidentification scenarios include:
| Actual Material | Patient's Belief | Hyaluronidase Effect |
|---|---|---|
| Calcium hydroxylapatite (Radiesse) | "I think it was HA" | Completely ineffective |
| Poly-L-lactic acid (Sculptra) | "I am not sure" | Completely ineffective |
| Polycaprolactone (Ellanse) | "The clinic said it could be dissolved" | Completely ineffective |
| Silicone / unregulated injectables | "It was done years ago" | Completely ineffective |
| HA (already encapsulated) | "It is definitely HA" | Extremely limited effect |
Key Insight: Many patients do not know the exact material that was injected, especially when treatments were performed years ago at different clinics. Without clear material documentation, using hyaluronidase is essentially blind treatment. High-resolution ultrasound examination is the essential first step in confirming material identity.
Reason 2: Encapsulation Has Created a Physical Barrier
Even when the material is confirmed as hyaluronic acid, if the body has formed a dense fibrous capsule around the filler (encapsulation), hyaluronidase cannot penetrate this biological wall to reach the HA molecules inside.
This is analogous to trying to dissolve sugar inside a sealed glass jar by pouring water over the outside. No matter how much water you pour, the sugar inside remains untouched. For a detailed explanation of the encapsulation mechanism, see our article: Encapsulation: Why Dissolvers Fail.
High-risk factors for encapsulation include:
- More than one year since injection
- History of repeated inflammation
- Use of permanent or semi-permanent fillers
- Excessive injection volume or concentration
Reason 3: Insufficient Dosage or Imprecise Injection Location
The effectiveness of hyaluronidase is highly dependent on two factors: adequate dosage and precise injection placement. Common failure patterns in clinical practice involve overly conservative dosing or injection into the wrong tissue plane.
The Dosage Dilemma
Many practitioners tend to be conservative with hyaluronidase dosing, concerned that excessive amounts may over-dissolve native hyaluronic acid in surrounding healthy tissue. This concern is valid, but the result is often a dose too small to produce meaningful results.
Positional Errors
A more common problem is that without imaging guidance, practitioners rely on experience or palpation to estimate the filler's location and depth. However, filler may have already migrated from its original injection site. When hyaluronidase is injected into the wrong tissue layer, it simply cannot contact the filler material.
Key Insight: Hyaluronidase injection without ultrasound guidance is fundamentally a blind procedure—the practitioner cannot confirm whether the needle has actually reached the filler location. This is precisely why we insist that all filler treatments must be performed under real-time ultrasound monitoring.
Reason 4: Biofilm Has Formed on the Filler
Biofilm is a thin, colony-forming bacterial layer that establishes itself on the filler surface. Once biofilm is present, it not only protects bacteria from antibiotic attack but also alters the local tissue environment around the filler, leading to chronic inflammation and tissue overgrowth.
When biofilm is present, even if hyaluronidase can dissolve a portion of the HA, the problem cannot be fundamentally resolved—because the lump is caused not only by the filler itself but also by the surrounding inflammatory tissue and bacterial colonies. For more information on biofilm, see: Biofilm and Recurrent Filler Swelling.
Reason 5: Mixed Material Injections
Some patients have received multiple injections of different materials in the same area over time. For example, HA may have been injected first, followed by calcium hydroxylapatite or a collagen stimulator. In these cases, hyaluronidase can only dissolve the HA component, while the non-HA portions remain and maintain the lump's shape.
| Mixed Scenario | What Hyaluronidase Can Address | Remaining Problem |
|---|---|---|
| HA + Radiesse | HA only | CaHA residue persists |
| HA + Sculptra | HA only | PLLA nodules persist |
| HA + Ellanse | HA only | PCL residue persists |
| Multiple HA brands | Partially effective | Highly cross-linked HA may resist |
Reason 6: Excessively High Cross-Linking Density
Different brands of HA fillers have varying degrees of cross-linking. Higher cross-linking density means greater molecular stability and greater resistance to enzymatic breakdown. Certain highly cross-linked fillers—especially those designed for deep tissue injection—demonstrate significantly stronger resistance to hyaluronidase.
Additionally, over time, interactions between the filler and surrounding tissue can further stabilize the filler structure, reducing the enzyme's effectiveness even further.
Reason 7: Tissue Fibrosis (excess scar tissue formation) and Scar Formation
Repeated hyaluronidase injections can themselves trigger local tissue inflammation and fibrosis. Each injection constitutes tissue trauma, and the body responds with a repair response—generating more fibrous tissue. This creates a vicious cycle:
- Hyaluronidase injection fails to fully dissolve the filler
- The injection process causes local inflammation
- The body generates reparative fibrous tissue
- Fibrous tissue further encases the remaining filler
- The next hyaluronidase attempt is even less likely to penetrate
For more on the cumulative damage from repeated dissolving enzyme injections, see: Cumulative Damage from Repeated Hyaluronidase Injections.
Ultrasound-Guided Minimally Invasive Extraction: See It to Solve It
When hyaluronidase treatment fails repeatedly, continuing to inject blindly is not only ineffective but may cause further harm. Our Ultrasound-Guided Pinhole Extraction technique offers a fundamentally different treatment approach:
Treatment Process
- High-resolution ultrasound scanning: Precisely identifies the filler's material type, location, depth, extent, and relationship to surrounding structures
- Real-time image guidance: Under continuous ultrasound monitoring, a single pinhole entry is made at the exact location
- Physical extraction: Directly removes the filler material and capsule tissue rather than relying on chemical dissolution
- Post-procedure confirmation: Ultrasound verification of clearance completeness
The "See Before You Treat" Philosophy
The fundamental problem with traditional hyaluronidase injection is that it is performed blind—the practitioner cannot confirm the material, cannot locate the filler precisely, and cannot assess the degree of encapsulation. Ultrasound completely changes this equation, ensuring every step of the procedure is performed under visual confirmation.
Key Insight: Hyaluronidase failure does not mean the problem is unsolvable. It means a different treatment strategy is needed. Shifting from chemical dissolution to physical extraction, from blind injection to image-guided treatment—this is the correct approach for managing resistant filler complications.
When Should You Stop Trying Hyaluronidase and Pursue Extraction?
If any of the following conditions apply, it is advisable to stop further hyaluronidase attempts and seek an ultrasound evaluation as soon as possible:
- Two or more rounds of hyaluronidase with no significant improvement
- Uncertainty about the injected material
- More than two years since the filler injection
- The lump feels firm or has distinct borders on palpation
- Recurrent episodes of swelling or inflammation
- History of infection at the injection site
If you are facing repeated hyaluronidase failure, we recommend starting with a comprehensive ultrasound evaluation to identify the root cause before deciding on next steps.
Schedule a consultation and let us help you find a real solution.
Conclusion
Hyaluronidase is a useful tool, but it has clear limitations. Understanding those limitations is the key to avoiding wasted time, money, and further tissue damage. Effective filler complication management begins with accurate diagnosis—and accurate diagnosis begins with the ability to see.
Related Services
Specialties
Credentials
- Kaohsiung Medical University, School of Medicine
- Attending Physician, Dermatology, Kaohsiung Chang Gung Memorial Hospital
- Attending Physician, Aesthetic Center, Kaohsiung Chang Gung Memorial Hospital
- Visiting Physician, Dermatology, Xiamen Chang Gung Hospital
- Visiting Physician, Aesthetic Center, Xiamen Chang Gung Hospital
"For every surgery, I strive to achieve the best outcome through the smallest incision and finest technique. Minimally invasive surgery is not just a technique — it's a commitment of respect to every patient."
Recovery from filler complications needs peer support too
Want to learn more?
Schedule a consultation for professional evaluation and advice

